Scioderm’s SD-101 Receives Breakthrough Therapy Designation from FDA for Treatment of Epidermolysis Bullosa
DURHAM, N.C., April 29, 2013 Scioderm announced its investigational product SD-101 has received Breakthrough Therapy designation by the U.S. Food and Drug Administration (FDA) for the treatment of patients with inherited Epidermolysis Bullosa (EB). SD-101 is Scioderm’s investigational therapy that is being evaluated for the treatment of skin blistering and erosions associated with this disease, including facilitation of healing of skin lesions and reduction of the incidence and/or severity of new lesions.
read all at
FDA Approves Kcentra for the Urgent Reversal of Anticoagulation in Adults with Major Bleeding

April 29, 2013
The U.S. Food and Drug Administration today approved Kcentra (Prothrombin Complex Concentrate, Human) for the urgent reversal of vitamin K antagonist (VKA) anticoagulation in adults with acute major bleeding. Plasma is the only other product approved for this use in the United States.
Patients receiving chronic anticoagulation therapy with warfarin and other VKA anticoagulants to prevent blood clotting in conditions such as atrial fibrillation or the presence of an artificial heart valve sometimes develop acute bleeding. Like plasma, Kcentra is used in conjunction with the administration of vitamin K to reverse the anticoagulation effect and stop the bleeding. Unlike plasma, Kcentra does not require blood group typing or thawing, so it can be administered more quickly than frozen plasma.
“The FDA’s approval of this new product gives physicians a choice when deciding how to treat patients requiring urgent reversal of VKA anticoagulation,” said Karen Midthun, M.D., director, Center for Biologics Evaluation and Research, FDA. “Kcentra is administered in a significantly lower volume than plasma at recommended doses, providing an alternative for those patients who may not tolerate the volume of plasma required to reverse VKA anticoagulation.”

Kcentra is associated with the occurrence of blood clots when used as indicated, and carries a boxed warning regarding the risk of blood clots. The warning also explains that patients receiving Kcentra should be monitored for signs and symptoms of thromboembolic events, as both fatal and non-fatal arterial and venous thromboembolic complications have been reported in clinical trials and post marketing surveillance.
Kcentra is made from the pooled plasma of healthy donors. It is processed in a way to minimize the risk of transmitting viral and other diseases. The FDA approval of Kcentra was based on a study of 216 patients who had been receiving VKA anticoagulation and who had acute major bleeding along with a clotting test value indicative of anticoagulant use. Kcentra was demonstrated to be similar to plasma in terms of the ability to stop acute major bleeding.
The drug is manufactured by CSL Behring, Marburg, Germany.

GSK announces regulatory submission for umeclidinium monotherapy in European Union
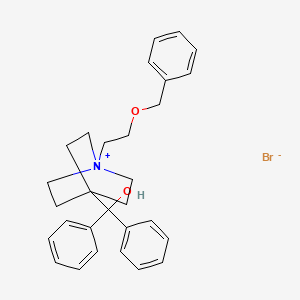
Umeclidinium bromide
http://www.ama-assn.org/resources/doc/usan/umeclidinium-bromide.pdf
26 April 2013
GlaxoSmithKline plc today announced the submission of a regulatory application in the European Union for the investigational once-daily medicine, umeclidinium bromide (UMEC), for patients with chronic obstructive pulmonary disease (COPD).
UMEC is an investigational bronchodilator molecule (formerly known as GSK573719), a long-acting muscarinic antagonist (LAMA), administered using the ELLIPTA™ inhaler.
A Marketing Authorisation Application (MAA) for UMEC monotherapy (55 mcg delivered dose) has been submitted to the European Medicines Agency (EMA), for a maintenance bronchodilator treatment to relieve symptoms in adult patients with COPD.
Regulatory filings for UMEC monotherapy are imminent in the US and planned in other countries during the course of 2013.
Daiichi Sankyo enrolls first patient in Nimotuzumab Phase 3 clinical trials

Nimotuzumab
25 April 2013
Daiichi Sankyo Company, Limited announced today that the first patient has been enrolled in two pivotal phase 3 clinical trials of nimotuzumab (DE-766), a recombinant humanized monoclonal antibody targeting the Epidermal Growth Factor Receptor (EGFR), which is being evaluated for the treatment of patients diagnosed with lung cancer and with gastric cancer.
About Phase 3 Clinical Trials for Lung Cancer
The phase 3 clinical trial is a multicenter, randomized, double-blind, placebo-controlled study investigating nimotuzumab for the first-line therapy in patients with unresectable and locally advanced squamous cell lung cancer. The patients will receive either nimotuzumab in combination with concurrent chemoradiotherapy or placebo in combination with concurrent chemoradiotherapy. The primary endpoint is overall survival (OS), and the secondary endpoints are progression free survival (PFS) and safety. Approximately 420 patients are planned to be enrolled at approximately 60 clinical centers in Japan. Additional details of the trial are available onwww.clinicaltrials.jp/user/cteSearch.jsp.
About Phase 3 Clinical Trials for Gastric Cancer (ENRICH study)
The ENRICH study is a randomized, open-label, Japan-Korea collaborative study of previously treated patients with EGFR overexpressed advanced gastric and gastroesophageal junction cancer who will receive either nimotuzumab and irinotecan hydrochloride hydrate (hereafter, irinotecan) combination therapy or irinotecan monotherapy. The primary endpoint is overall survival (OS), and the secondary endpoints are progression free survival (PFS) and safety. Approximately 400 patients are planned to be enrolled at approximately 40 clinical centers in Japan and South Korea. In Korea, Kuhnil Pharmaceutical Company, Limited (hereafter, Kuhnil) is implementing this trial. Additional details of the trial are available on www.clinicaltrials.gov.
About Unresectable and Locally Advanced Squamous Cell Lung Cancer
In Japan, lung cancer is the first leading cause of cancer death, with about 70,000 deaths in 2011.i Non-small cell lung cancer (adenocarcinoma, squamous cell carcinoma, and large cell carcinoma) occupies more than 80 percent of lung cancer. Concurrent chemoradiotherapy for a radical cure is currently used as the standard treatment for patients with stage III locally advanced non-small cell lung cancer, in which radical surgery is not possible but radiotherapy is.ii Of these cases, between 30 and 40 percent are squamous cell carcinoma and EGFR is known to be overexpressed.iii
About Gastric Cancer
Half of the total number of gastric cancer cases worldwide occurs in Eastern Asia.iv In Japan, gastric cancer is the second leading cause of cancer death, with an estimated about 50,000 deaths. i In South Korea, about 10,000 gastric cancer deaths in 2011 were reported.v Numerous improvements have occurred in the management of gastric cancer; however, gastric cancer still has a poor prognosis. For patients with earlier stages of disease, more than 50% undergo surgery, but even after a curative resection, 60% of these patients eventually relapse locally or with distant metastases. vi
About Nimotuzumab and EGFR
Nimotuzumab is an intravenously administered recombinant humanized monoclonal antibody directed against human EGFR and is produced by CIMAB S.A. (Cuba). Nimotuzumab blocks the binding of EGF to its receptor interfering with the cell signaling pathway. Nimotuzumab has been approved for head and neck cancer, glioma, and esophageal cancer in several countries. EGFR is known to be overexpressed in a wide variety of human tumors.vii Overexpression of EGFR in tumors correlates with increased metastasis, decreased survival, and a poor prognosis. It is known that EGFR is activated by exposure to radiation.
In 2006, Daiichi Sankyo introduced nimotuzumab from CIMAB S.A. and CIMYM BioSciences Inc. (Canada) and has the rights to develop and commercialize in Japan. In Korea, Kuhnil has the rights to develop and commercialize.
15 top blockbuster drug contenders, compiled:Fiercebiotech, by John Carroll and Ryan McBride
15 top blockbuster drug contenders, compiled fiercebiotech, by John Carroll and Ryan McBride
read all this at
http://www.fiercebiotech.com/special-reports/top-15-blockbuster-contenders

Top 20 Best-Selling Drugs Approved and Launched During 2012
Biotechnology from bench to business
Top 20 Best-Selling Drugs Approved and Launched During 2012
What new medicines are shaking things up?
read all this at http://www.genengnews.com/insight-and-intelligence/top-20-best-selling-drugs-approved-and-launched-during-2012/77899791/
have a good reading
Biosimilars: 10 Drugs to Watch
Biotechnology from bench to business
Biosimilars: 10 Drugs to Watch
Which innovator drugs are companies scrambling to copy?
read at
http://www.genengnews.com/insight-and-intelligence/biosimilars-10-drugs-to-watch/77899804/
http://www.genengnews.com/insight-and-intelligence
have a great reading
Researchers at Northeastern University in Boston have developed a gene therapy approach that may one day stop Parkinson’s disease (PD) in it tracks, preventing disease progression and reversing its symptoms
Glial cell derived neurotrophic factor structure (credit: Wikimedia Commons)
http://experimentalbiology.org/EB/pages/default.aspx?splashpage=1
A noninvasive avenue for Parkinson’s disease gene therapy
April 26, 2013
Researchers at Northeastern University in Boston have developed a gene therapy approach that may one day stop Parkinson’s disease (PD) in it tracks, preventing disease progression and reversing its symptoms.
The novelty of the approach lies in the nasal route of administration and nanoparticles containing a gene capable of rescuing dying neurons in the brain.
Parkinson’s is a devastating neurodegenerative disorder caused by the death of dopamine neurons in a key motor area of the brain, the substantia nigra (SN). Loss of these neurons leads to the characteristic tremor and slowed movements of PD, which get increasingly worse with time.
Currently, more than 1% of the population over age 60 has PD and approximately 60,000 Americans are newly diagnosed every year. The available drugs on the market for PD mimic or replace the lost dopamine but do not get to the heart of the problem, which is the progressive loss of the dopamine neurons.
The focus of Dr. Barbara Waszczak‘s lab at Northeastern University in Boston is to find a way to harvest the potential of glial cell line-derived neurotrophic factor (GDNF) as a treatment for PD. GDNF is a protein known to nourish dopamine neurons by activating survival and growth-promoting pathways inside the cells.
Bypassing the blood-brain barrier
Not surprisingly, GDNF is able to protect dopamine neurons from injury and restore the function of damaged and dying neurons in many animal models of PD. However, the action of GDNF is limited by its inability to cross the blood-brain barrier (BBB), thus requiring direct surgical injection into the brain.
To circumvent this problem, Waszczak’s lab is investigating intranasal delivery as a way to bypass the BBB. Their previous work showed that intranasal delivery of GDNF protects dopamine neurons from damage by the neurotoxin, 6-hydroxydopamine (6-OHDA), a standard rat model of PD.
Taking this work a step further, Brendan Harmon, working in Waszczak’s lab, has adapted the intranasal approach so that cells in the brain can continuously produce GDNF. His work utilized nanoparticles, developed by Copernicus Therapeutics, Inc., which are able to transfect brain cells with an expression plasmid carrying the gene for GDNF (pGDNF).
When given intranasally to rats, these pGDNF nanoparticles increase GDNF production throughout the brain for long periods, avoiding the need for frequent re-dosing.
Now, in new research presented at Experimental Biology 2013 in Boston, Harmon reported that intranasal administration of Copernicus’ pGDNF nanoparticles results in GDNF expression sufficient to protect SN dopamine neurons in the 6-OHDA model of PD.
Waszczak and Harmon believe that intranasal delivery of Copernicus’ nanoparticles may provide an effective and non-invasive means of GDNF gene therapy for PD, and an avenue for transporting other gene therapy vectors to the brain.
This work, which was funded in part by the Michael J. Fox Foundation for Parkinson’s Research and Northeastern University, has the potential to greatly expand treatment options for PD and many other central nervous system disorders.
Potential diabetes breakthrough Harvard researchers discover hormone that spurs beta cell production
Betatrophin causes a specific increase in pancreatic β cell replication. Betatrophin is a secreted protein expressed in liver and fat. The increase in β cell replication and mass improves glycemic control. (Credit: Peng Yi, Ji-Sun Park, Douglas A. Melton/Cell)
Potential diabetes breakthrough
Researchers at the Harvard Stem Cell Institute (HSCI) have discovered a hormone that holds promise for a dramatically more effective treatment of type 2 diabetes, a metabolic illness afflicting an estimated 26 million Americans.
The researchers believe that the hormone might also have a role in treating type 1, or juvenile, diabetes.
The work was published by the journal Cell.
The hormone, called betatrophin, causes mice to produce insulin-secreting pancreatic beta cells at up to 30 times the normal rate. The new beta cells only produce insulin when called for by the body, offering the potential for the natural regulation of insulin and a great reduction in the complications associated with diabetes, the leading medical cause of amputations and non-genetic loss of vision.
The researchers who discovered betatrophin, HSCI co-director Doug Melton and postdoctoral fellow Peng Yi, caution that much work remains to be done before it could be used as a treatment in humans. But the results of their work, which was supported in large part by a federal research grant, already have attracted the attention of drug manufacturers.
“If this could be used in people,” said Melton, Harvard’s Xander University Professor and co-chair of the University’s Department of Stem Cell and Regenerative Biology, “it could eventually mean that instead of taking insulin injections three times a day, you might take an injection of this hormone once a week or once a month, or in the best case maybe even once a year.”
Type 2 diabetes, a disease associated with the national obesity epidemic, is usually caused by a combination of excess weight and lack of exercise. It causes patients to slowly lose beta cells and the ability to produce adequate insulin. One recent study has estimated that diabetes treatment and complications cost the United States $218 billion annually, or about 10 percent of the nation’s entire health bill.
“Our idea here is relatively simple,” Melton said. “We would provide this hormone, the type 2 diabetic will make more of their own insulin-producing cells, and this will slow down, if not stop, the progression of their diabetes. I’ve never seen any treatment that causes such an enormous leap in beta cell replication.”

 DRUG APPROVALS BY DR ANTHONY MELVIN CRASTO
DRUG APPROVALS BY DR ANTHONY MELVIN CRASTO