Home » Posts tagged 'Rare disease'
Tag Archives: Rare disease
FDA approves first U.S. treatment benznidazole for Chagas disease
The U.S. Food and Drug Administration today granted accelerated approval to benznidazole for use in children ages 2 to 12 years old with Chagas disease. It is the first treatment approved in the United States for the treatment of Chagas disease.
Chagas disease, or American trypanosomiasis, is a parasitic infection caused by Trypanosoma cruzi and can be transmitted through different routes, including contact with the feces of a certain insect, blood transfusions, or from a mother to her child during pregnancy. After years of infection, the disease can cause serious heart illness, and it also can affect swallowing and digestion. While Chagas disease primarily affects people living in rural parts of Latin America, recent estimates are that there may be approximately 300,000 persons in the United States with Chagas disease.
“The FDA is committed to making available safe and effective therapeutic options to treat tropical diseases,” said Edward Cox, M.D., director of the Office of Antimicrobial Products in the FDA’s Center for Drug Evaluation and Research.
The safety and efficacy of benznidazole were established in two placebo-controlled clinical trials in pediatric patients 6 to 12 years old. In the first trial, approximately 60 percent of children treated with benznidazole had an antibody test change from positive to negative compared with approximately 14 percent of children who received a placebo. Results in the second trial were similar: Approximately 55 percent of children treated with benznidazole had an antibody test change from positive to negative compared with 5 percent who received a placebo. An additional study of the safety and pharmacokinetics (how the body absorbs, distributes and clears the drug) of benznidazole in pediatric patients 2 to 12 years of age provided information for dosing recommendations down to 2 years of age.
The most common adverse reactions in patients taking benznidazole were stomach pain, rash, decreased weight, headache, nausea, vomiting, abnormal white blood cell count, urticaria (hives), pruritus (itching) and decreased appetite. Benznidazole is associated with serious risks including serious skin reactions, nervous system effects and bone marrow depression. Based on findings from animal studies, benznidazole could cause fetal harm when administered to a pregnant woman.
Benznidazole was approved using the Accelerated Approval pathway. The Accelerated Approval pathway allows the FDA to approve drugs for serious conditions where there is unmet medical need and adequate and well-controlled trials establish that the drug has an effect on a surrogate endpoint that is reasonably likely to predict a clinical benefit to patients. Further study is required to verify and describe the anticipated clinical benefit of benznidazole.
The FDA granted benznidazole priority review and orphan product designation. These designations were granted because Chagas disease is a rare disease, and until now, there were no approved drugs for Chagas disease in the United States.
With this approval, benznidazole’s manufacturer, Chemo Research, S. L., is awarded a Tropical Disease Priority Review Voucher in accordance with a provision included in the Food and Drug Administration Amendments Act of 2007 that aims to encourage development of new drugs and biological products for the prevention and treatment of certain tropical diseases.
 |
|
| Clinical data | |
|---|---|
| Trade names | Rochagan, Radanil[1] |
| AHFS/Drugs.com | Micromedex Detailed Consumer Information |
| Routes of administration |
by mouth |
| ATC code | |
| Pharmacokinetic data | |
| Bioavailability | High |
| Metabolism | Liver |
| Biological half-life | 12 hours |
| Excretion | Kidney and fecal |
| Identifiers | |
| CAS Number | |
| PubChem CID | |
| ChemSpider | |
| UNII | |
| KEGG | |
| ChEBI | |
| ChEMBL | |
| ECHA InfoCard | 100.153.448 |
| Chemical and physical data | |
| Formula | C12H12N4O3 |
| Molar mass | 260.249 g/mol |
| 3D model (JSmol) | |
| Melting point | 188.5 to 190 °C (371.3 to 374.0 °F) |
Benznidazole is an antiparasitic medication used in the treatment of Chagas disease.[2] While it is highly effective in early disease this decreases in those who have long term infection.[3] It is the first line treatment given its moderate side effects compared to nifurtimox.[1] It is taken by mouth.[2]
Side effects are fairly common. They include rash, numbness, fever, muscle pain, loss of appetite, and trouble sleeping.[4][5] Rare side effects include bone marrow suppression which can lead to low blood cell levels.[1][5] It is not recommended during pregnancy or in people with severe liver or kidney disease.[4][3]Benznidazole is in the nitroimidazole family of medication and works by the production of free radicals.[5][6]
Benznidazole came into medical use in 1971.[2] It is on the World Health Organization’s List of Essential Medicines, the most effective and safe medicines needed in a health system.[7] It is not commercially available in the United States, but can be obtained from the Centers of Disease Control.[2] As of 2012 Laboratório Farmacêutico do Estado de Pernambuco, a government run pharmaceutical company in Brazil was the only producer.[8]
Medical uses
Benznidazole has a significant activity during the acute phase of Chagas disease, with a therapeutical success rate up to 80%. Its curative capabilities during the chronic phase are, however, limited. Some studies have found parasitologic cure (a complete elimination of T. cruzi from the body) in pediatric and young patients during the early stage of the chronic phase, but overall failure rate in chronically infected individuals is typically above 80%.[6]
However, some studies indicate treatment with benznidazole during the chronic phase, even if incapable of producing parasitologic cure, because it reduces electrocardiographic changes and a delays worsening of the clinical condition of the patient.[6]
Benznidazole has proven to be effective in the treatment of reactivated T. cruzi infections caused by immunosuppression, such as in people with AIDS or in those under immunosuppressive therapy related to organ transplants.[6]
Children
Benznidazole can be used in children and infants, with the same 5–7 mg/kg per day weight-based dosing regimen that is used to treat adult infections.[9] Children are found to be at a lower risk of adverse events compared to adults, possibly due to increased hepatic clearance of the drug. The most prevalent adverse effects in children were found to be gastrointestinal, dermatologic, and neurologic in nature. However, the incidence of severe dermatologic and neurologic adverse events is lower in the pediatric population compared to adults.[10]
Pregnant women
Studies in animals have shown that benznidazole can cross the placenta.[11] Due to its potential for teratogenicity, use of benznidazole in pregnancy is not recommended.[9]
Side effects
Side effects tend to be common and occur more frequently with increased age.[12] The most common adverse reactions associated with benznidazole are allergic dermatitis and peripheral neuropathy.[1] It is reported that up to 30% of people will experience dermatitis when starting treatment.[11][13] Benznidazole may cause photosensitization of the skin, resulting in rashes.[1] Rashes usually appear within the first 2 weeks of treatment and resolve over time.[13] In rare instances, skin hypersensitivity can result in exfoliative skin eruptions, edema, and fever.[13] Peripheral neuropathy may occur later on in the treatment course and is dose dependent.[1] It is not permanent, but takes time to resolve.[13]
Other adverse reactions include anorexia, weight loss, nausea, vomiting, insomnia, and dysguesia, and bone marrow suppression.[1] Gastrointestinal symptoms usually occur during the initial stages of treatment and resolves over time.[13] Bone marrow suppression has been linked to the cumulative dose exposure.[13]
Contraindications
Benznidazole should not be used in people with severe liver and/or kidney disease.[12] Pregnant women should not use benznidazole because it can cross the placenta and cause teratogenicity.[11]
Pharmacology
Mechanism of action
Benznidazole is a nitroimidazole antiparasitic with good activity against acute infection with Trypanosoma cruzi, commonly referred to as Chagas disease.[11] Like other nitroimidazoles, benznidazole’s main mechanism of action is to generate radical species which can damage the parasite’s DNA or cellular machinery.[14] The mechanism by which nitroimidazoles do this seems to depend on whether or not oxygen is present.[15] This is particularly relevant in the case of Trypanosoma species, which are considered facultative anaerobes.[16]
Under anaerobic conditions, the nitro group of nitroimidazoles is believed to be reduced by the pyruvate:ferredoxin oxidoreductase complex to create a reactive nitro radical species.[14] The nitro radical can then either engage in other redox reactions directly or spontaneously give rise to a nitrite ion and imidazole radical instead.[15] The initial reduction takes place because nitroimidazoles are better electron acceptors for ferredoxin than the natural substrates.[14] In mammals, the principal mediators of electron transport are NAD+/NADH and NADP+/NADPH, which have a more positive reduction potential and so will not reduce nitroimidazoles to the radical form.[14] This limits the spectrum of activity of nitroimidazoles so that host cells and DNA are not also damaged. This mechanism has been well-established for 5-nitroimidazoles such as metronidazole, but it is unclear if the same mechanism can be expanded to 2-nitroimidazoles (including benznidazole).[15]
In the presence of oxygen, by contrast, any radical nitro compounds produced will be rapidly oxidized by molecular oxygen, yielding the original nitroimidazole compound and a superoxide anion in a process known as “futile cycling“.[14] In these cases, the generation of superoxide is believed to give rise to other reactive oxygen species.[15] The degree of toxicity or mutagenicity produced by these oxygen radicals depends on cells’ ability to detoxify superoxide radicals and other reactive oxygen species.[15] In mammals, these radicals can be converted safely to hydrogen peroxide, meaning benznidazole has very limited direct toxicity to human cells.[15] In Trypanosoma species, however, there is a reduced capacity to detoxify these radicals, which results in damage to the parasite’s cellular machinery.[15]
Pharmacokinetics
Oral benznidazole has a bioavailability of 92%, with a peak concentration time of 3–4 hours after administration.[17] 5% of the parent drug is excreted unchanged in the urine, which implies that clearance of benznidazole is mainly through metabolism by the liver.[18] Its elimination half-life is 10.5-13.6 hours.[17]
Interactions
Benznidazole and other nitroimidazoles have been shown to decrease the rate of clearance of 5-fluorouracil (including 5-fluorouracil produced from its prodrugs capecitabine, doxifluridine, and tegafur).[19]While co-administration of any of these drugs with benznidazole is not contraindicated, monitoring for 5-fluorouracil toxicity is recommended in the event they are used together.[20]
The GLP-1 receptor agonist lixisenatide may slow down the absorption and activity of benznidazole, presumably due to delayed gastric emptying.[21]
Because nitroimidazoles can kill Vibrio cholerae cells, use is not recommended within 14 days of receiving a live cholera vaccine.[22]
Alcohol consumption can cause a disulfiram like reaction with benznidazole.[1]
References
- ^ Jump up to:a b c d e f g h Bern, Caryn; Montgomery, Susan P.; Herwaldt, Barbara L.; Rassi, Anis; Marin-Neto, Jose Antonio; Dantas, Roberto O.; Maguire, James H.; Acquatella, Harry; Morillo, Carlos (2007-11-14). “Evaluation and Treatment of Chagas Disease in the United States: A Systematic Review”. JAMA. 298 (18): 2171–81. ISSN 0098-7484. PMID 18000201. doi:10.1001/jama.298.18.2171.
- ^ Jump up to:a b c d “Our Formulary | Infectious Diseases Laboratories | CDC”. http://www.cdc.gov. 22 September 2016. Retrieved 7 December2016.
- ^ Jump up to:a b “Chagas disease”. World Health Organization. March 2016. Retrieved 7 December 2016.
- ^ Jump up to:a b Prevention, CDC – Centers for Disease Control and. “CDC – Chagas Disease – Resources for Health Professionals – Antiparasitic Treatment”. http://www.cdc.gov. Retrieved 2016-11-05.
- ^ Jump up to:a b c Castro, José A.; de Mecca, Maria Montalto; Bartel, Laura C. (2006-08-01). “Toxic side effects of drugs used to treat Chagas’ disease (American trypanosomiasis)”. Human & Experimental Toxicology. 25 (8): 471–479. ISSN 0960-3271. PMID 16937919. doi:10.1191/0960327106het653oa.
- ^ Jump up to:a b c d Urbina, Julio A. “Nuevas drogas para el tratamiento etiológico de la Enfermedad de Chagas” (in Spanish). Retrieved March 24, 2012.
- Jump up^ “WHO Model List of Essential Medicines (19th List)” (PDF). World Health Organization. April 2015. Retrieved 8 December 2016.
- Jump up^ “Treatment for Chagas: Enter Supplier Number Two | End the Neglect”. endtheneglect.org. 21 March 2012. Retrieved 7 December 2016.
- ^ Jump up to:a b Carlier, Yves; Torrico, Faustino; Sosa-Estani, Sergio; Russomando, Graciela; Luquetti, Alejandro; Freilij, Hector; Vinas, Pedro Albajar (2011-10-25). “Congenital Chagas Disease: Recommendations for Diagnosis, Treatment and Control of Newborns, Siblings and Pregnant Women”. PLOS Negl Trop Dis. 5 (10): e1250. ISSN 1935-2735. PMC 3201907
 . PMID 22039554. doi:10.1371/journal.pntd.0001250.
. PMID 22039554. doi:10.1371/journal.pntd.0001250. - Jump up^ Altcheh, Jaime; Moscatelli, Guillermo; Moroni, Samanta; Garcia-Bournissen, Facundo; Freilij, Hector (2011-01-01). “Adverse Events After the Use of Benznidazole in Infants and Children With Chagas Disease”. Pediatrics. 127 (1): e212–e218. ISSN 0031-4005. PMID 21173000. doi:10.1542/peds.2010-1172.
- ^ Jump up to:a b c d Pérez-Molina, José A.; Pérez-Ayala, Ana; Moreno, Santiago; Fernández-González, M. Carmen; Zamora, Javier; López-Velez, Rogelio (2009-12-01). “Use of benznidazole to treat chronic Chagas’ disease: a systematic review with a meta-analysis”. Journal of Antimicrobial Chemotherapy. 64 (6): 1139–1147. ISSN 0305-7453. PMID 19819909. doi:10.1093/jac/dkp357.
- ^ Jump up to:a b Prevention, CDC – Centers for Disease Control and. “CDC – Chagas Disease – Resources for Health Professionals – Antiparasitic Treatment”. http://www.cdc.gov. Retrieved 2016-11-07.
- ^ Jump up to:a b c d e f Grayson, M. Lindsay; Crowe, Suzanne M.; McCarthy, James S.; Mills, John; Mouton, Johan W.; Norrby, S. Ragnar; Paterson, David L.; Pfaller, Michael A. (2010-10-29). Kucers’ The Use of Antibiotics Sixth Edition: A Clinical Review of Antibacterial, Antifungal and Antiviral Drugs. CRC Press. ISBN 9781444147520.
- ^ Jump up to:a b c d e Edwards, David I (1993). “Nitroimidazole drugs – action and resistance mechanisms. I. Mechanism of action”. Journal of Antimicrobial Chemotherapy. 31: 9–20. doi:10.1093/jac/31.1.9.
- ^ Jump up to:a b c d e f g Eller, Gernot. “Synthetic Nitroimidazoles: Biological Activities and Mutagenicity Relationships”. Scientia Pharmaceutica. 77: 497–520. doi:10.3797/scipharm.0907-14.
- Jump up^ Cheng, Thomas C. (1986). General Parasitology. Orlando, Florida: Academic Press. p. 140. ISBN 0-12-170755-5.
- ^ Jump up to:a b Raaflaub, J; Ziegler, WH (1979). “Single-dose pharmacokinetics of the trypanosomicide benznidazole in man”. Arzneimittelforschung. 29 (10): 1611–1614.
- Jump up^ Workman, P.; White, R. A.; Walton, M. I.; Owen, L. N.; Twentyman, P. R. (1984-09-01). “Preclinical pharmacokinetics of benznidazole.”. British Journal of Cancer. 50 (3): 291–303. ISSN 0007-0920. PMC 1976805
 . PMID 6466543. doi:10.1038/bjc.1984.176.
. PMID 6466543. doi:10.1038/bjc.1984.176. - Jump up^ Product Information: Teysuno oral capsules, tegafur gimeracil oteracil oral capsules. Nordic Group BV (per EMA), Hoofddorp, The Netherlands, 2012.
- Jump up^ Product Information: TINDAMAX(R) oral tablets, tinidazole oral tablets. Mission Pharmacal Company, San Antonio, TX, 2007.
- Jump up^ Product Information: ADLYXIN(TM) subcutaneous injection, lixisenatide subcutaneous injection. sanofi-aventis US LLC (per manufacturer), Bridgewater, NJ, 2016.
- Jump up^ Product Information: VAXCHORA(TM) oral suspension, cholera vaccine live oral suspension. PaxVax Inc (per manufacturer), Redwood City, CA, 2016.
External links
- “Rochagan [Patient Information]” (PDF) (in Portuguese). Hoffmann-La Roche. Retrieved 2006-11-27.
////////////benznidazole, Chemo Research, Tropical Disease Priority Review Voucher, Chagas disease, rare disease, FDA 2017
FDA approves first drug to treat a rare enzyme disorder in pediatric and adult patients



December 8, 2015
Release
Today, the U.S. Food and Drug Administration approved Kanuma (sebelipase alfa) as the first treatment for patients with a rare disease known as lysosomal acid lipase (LAL) deficiency.
Patients with LAL deficiency (also known as Wolman disease and cholesteryl ester storage disease [CESD]) have no or little LAL enzyme activity. This results in a build-up of fats within the cells of various tissues that can lead to liver and cardiovascular disease and other complications. Wolman disease often presents during infancy (around 2 to 4 months of age) and is a rapidly progressive disease. Patients with Wolman disease rarely survive beyond the first year of life. CESD is a milder, later-onset form of LAL deficiency and presents in early childhood or later. Life expectancy of patients with CESD depends on the severity of the disease and associated complications. Wolman disease affects one to two infants per million births, and CESD affects 25 individuals per million births.
Today’s action involved approvals from two FDA centers. The Center for Veterinary Medicine (CVM) approved an application for a recombinant DNA (rDNA) construct in chickens that are genetically engineered (GE) to produce a recombinant form of human lysosomal acid lipase (rhLAL) protein in their egg whites. The FDA regulates GE animals under the new animal drug provisions of the Federal Food, Drug, and Cosmetic Act, because an rDNA construct introduced into an animal to change its structure or function meets the definition of a drug. The Center for Drug Evaluation and Research (CDER) approved the human therapeutic biologic (Kanuma), which is purified from those egg whites, based on its safety and efficacy in humans with LAL deficiency.
“LAL deficiency is a rare inherited genetic disorder that can lead to serious and life-threatening organ damage, especially when onset begins in infancy,” said CDER Director Janet Woodcock, M.D. “Using this technology, these patients for the first time ever have access to a treatment that may improve their lives and chances of survival.”
The new therapy, Kanuma, provides an rhLAL protein that functions in place of the missing, partially active or inactive LAL protein in the patient. Kanuma is produced by GE chickens containing an rDNA construct responsible for producing rhLAL protein in their egg whites. These egg whites are refined to extract the rhLAL protein that is eventually used to produce Kanuma and treat patients with LAL deficiency. The GE chickens are used only for producing the drug substance, and neither the chicken nor the eggs are allowed in the food supply.
Kanuma is approved for use in patients with LAL deficiency. Treatment is provided via intravenous infusion once weekly in patients with rapidly progressive LAL deficiency presenting in the first six months of life, and once every other week in all other patients.
CDER evaluated the safety and efficacy of Kanuma in an open-label, historically controlled trial in nine infants with rapidly progressive Wolman disease and in a double-blind, placebo-controlled trial in 66 pediatric and adult patients with CESD. In the trial in infants with Wolman disease, six of nine infants (67 percent) treated with Kanuma were alive at 12 months of age, whereas none of the 21 infants in the historical control group survived. In the trial in CESD patients, there was a statistically significant improvement in LDL-cholesterol levels and other disease-related parameters in those treated with Kanuma versus placebo after 20 weeks of treatment.
The most common side effects observed in patients treated with Kanuma are diarrhea, vomiting, fever, rhinitis, anemia, cough, headache, constipation, and nausea.
In its review of the GE chicken application, CVM assessed the safety of the rDNA construct, including the safety of the rDNA construct to the animals, as well as a full review of the construct and its stability in the genome of the chicken over several generations. No adverse outcomes were noted in the chickens. As required by the National Environmental Policy Act and its implementing regulations, CVM evaluated the potential environmental impacts of approval of the sponsor’s GE chickens and determined that the approval does not cause any significant impact on the environment, because the chickens are raised in highly secure indoor facilities.
“We reviewed all of the data to ensure that the hens do produce rhLAL in their egg whites, without suffering any adverse health effects from the introduced rDNA construct. The company has taken rigorous steps to ensure that neither the chickens nor the eggs will enter the food supply, and we have confirmed their containment systems by inspecting the manufacturing facilities,” said CVM Director Bernadette Dunham, D.V.M., Ph.D.
The FDA granted Kanuma orphan drug designation because it treats a rare disease affecting fewer than 200,000 patients in the United States. Orphan drug designation provides financial incentives for rare disease drug development such as clinical trial tax credits, user fee waivers, and eligibility for market exclusivity to promote rare disease drug development. Kanuma was also granted breakthrough therapy designation as it is the first and only treatment available for Wolman disease, the very severe infant form of the disease. The breakthrough therapy designation program encourages the FDA to work collaboratively with sponsors, by providing timely advice and interactive communications, to help expedite the development and review of important new drugs for serious or life-threatening conditions. The Kanuma application was also granted a priority review, which is granted to drug applications that show a significant improvement in safety or effectiveness in the treatment of a serious condition. The manufacturer of Kanuma was granted a rare pediatric disease priority review voucher –– a provision intended to encourage development of new drugs and biologics for the prevention and treatment of rare pediatric diseases.
Kanuma is produced by Alexion Pharmaceuticals Inc., based in Cheshire, Connecticut.


Ibudilast

IBUDILAST, MN 166
AV-411
KC-404
MN-166
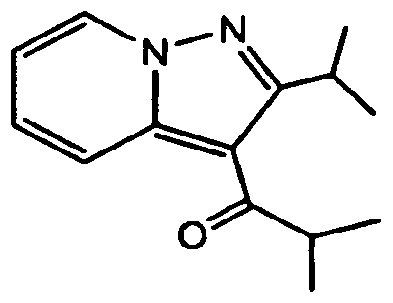
2-methyl-1-(2-propan-2-ylpyrazolo[1,5-a]pyridin-3-yl)propan-1-one
1-(2-isopropylpyrazolo[1,5-a]pyridin-3-yl)-2-methylpropan-1-one
KYORIN Kyorin Seiyaku Kk……….INNOVATOR

Ibudilast is an anti-inflammatory and neuroprotective oral agent which shows an excellent safety profile at 60 mg/day and provides significantly prolonged time-to-first relapse and attenuated brain volume shrinkage in patients with relapsing-remitting (RR) and/or secondary progressive (SP) multiple sclerosis (MS). Ibudilast is currently in development in the U.S. (codes: AV-411 or MN-166), but is approved for use as an antiinflammatory in Japan.



Ibudilast (development codes: AV-411 or MN-166) is an antiinflammatory drug used mainly in Japan, which acts as aphosphodiesterase inhibitor, inhibiting the PDE-4 subtype to the greatest extent,[1] but also showing significant inhibition of other PDE subtypes.[2][3]
Ibudilast has bronchodilator, vasodilator [4] and neuroprotective effects,[5][6] and is mainly used in the treatment of asthma andstroke.[7] It inhibits platelet aggregation,[8] and may also be useful in the treatment of multiple sclerosis.[9]
Ibudilast crosses the blood–brain barrier and suppresses glial cell activation. This activity has been shown to make ibudilast useful in the treatment of neuropathic pain and it not only enhances analgesia produced by opioid drugs, but also reduces the development oftolerance.[10]
It may have some use reducing methamphetamine[11] and alcohol[12] addiction.
It may have some use reducing methamphetamine addiction.[11]
Avigen has identified the potential of ibudilast (AV-411) for the treatment of neuropathic pain and other neurological indications, including opiate withdrawal. As an inhibitor of glial cells, ibudilast can deactivate these cells which produce various chemicals, including proinflammatory cytokines, in response to nerve damage or viral infection to amplify and maintain pain. Preclinical evaluation to date indicates that it reverses the painful sensory abnormality allodynia in chemotherapy- and trauma-induced neuropathic pain models.
Originator Kyorin and Banyu Pharmaceutical (now MSD KK following the merger of Banyu and Schering-Plough KK in 2010) have been developing ibudilast under a collaborative agreement. MediciNova obtained exclusive, worldwide rights outside of Japan, China, Taiwan and South Korea from Kyorin in October 2004 to develop and commercialize the compound for MS. In 2012, a codevelopment agreement was signed between MediciNova and the University of Colorado for the treatment of post-traumatic brain injury.

Sixteenth revised Japanese Pharmacopoeia chemicals, etc. IBUDILAST Ibudilast C14H18N2O: 230.31 [ 50847-11-5 ] that this product was dried when to quantify, including ibudilast (C14H18N2O) 98.5 ~ 101.0%.

http://www.google.co.in/patents/US3850941PATENT
EXAMPLE 1 Synthesis of 2-isopropyl-3-is0butyrylpyrazolo[1,5-a] pyridine (KC404) A mixture of 1-amino-Z-methylpyridinium iodide g.), isobutyric anhydride (500 g.) and K CO (81 g.) was refluxed for 8 hr. After cooling, the precipitated crystals were filtered off and water was added to the filtrate, The solution was made basic to pH 11 with K CO’ and extracted with ethyl acetate (1000 ml.). The extract’was washed with water (400 ml.), dried over Na SO and concentrated under reduced pressure. The residue was distilled to give 58 g. of colorless crystalline product, hp, 110- 175 (7.5 mm. Hg). Recrystallization from hexane gave colorless prisms, melting point 53.554.
Analysis- Calcd.: C, 73.01; H, 7.88; N, 12.17 Found: C, 72.86; H, 7.94; N, 12.09
CLIP

http://www.customsynthesis.com/ibud.html
PATENT
http://www.google.com/patents/US8119657
FIG. 6 is a synthetic reaction scheme illustrating one approach for preparing (S)-AV1013; the approach employs chiral chromatography of an N-protected form of the racemate as described in detail in Example 1.
FIG. 7 demonstrates additional reaction schemes for synthesizing (S)-AV1013.


Example 1Synthesis of (S)-2-amino-1-(2-isopropylpyrazolo[1,5-a]pyridin-3-yl)propan-1-one hydrochloride
(S)-2-Amino-1-(2-isopropylpyrazolo[1,5-a]pyridin-3-yl)propan-1-one hydrochloride (also referred to herein as S-AV1013.HCl) was prepared on a preparative scale using two different routes to obtain the intermediate isopropylpyrazolo[1,5-a]pyridine (IPPP). In the first approach (method 1), ibudilast was employed as the starting material to obtain IPPP; an alternate synthetic approach (method 2) employed ibudilast acid as the starting material.
Step 1Method 1Preparation of Isopropylpyrazolo[1,5-a]pyridine (IPPP) from ibudilast
A 5 L 3-neck round-bottom flask was equipped with a mechanical stirrer, thermocouple, heating mantle and a Y-adapter with a nitrogen inlet. The flask was charged with water (350 mL, USP), concentrated sulfuric acid (350 mL) and ibudilast (3-isobutyryl-2-isopropylpyrazolo[1,5-a]pyridine) (140 g, 0.608 mol). The flask was purged with nitrogen, and the mixture was stirred while it was heated to 135° C. An aliquot was removed for HPLC analysis, which showed that all starting material was consumed after 5 hours at 135° C., so the mixture was allowed to cool to room temperature overnight. The mixture was cooled in an ice bath, and water (1400 mL, USP) was added over 10 min, with the temperature maintained below 25° C. With continuous cooling in an ice bath, the mixture was neutralized by adding sodium hydroxide (50% w/w aq., 1150 mL) dropwise, with the temperature maintained below 25° C. Ethyl acetate (250 mL) was added, and the layers were separated. The aqueous layer was washed with ethyl acetate (2×300 mL). The combined ethyl acetate extracts were washed sequentially with 250 mL portions of saturated aqueous sodium bicarbonate and saturated aqueous sodium chloride, then dried over anhydrous sodium sulfate for 30 minutes. Activated carbon (20 g) and silica (60 g) were added and stirred before filtering over a pad of Celite. The filtrate was concentrated under reduced pressure to obtain 96.5 g of IPPP (2-isopropyl-pyrazolo[1,5-a]pyridine, 99% crude yield, 99.6 area % pure by HPLC) as an amber oil.
1H-NMR (CDCl3) δ 1.4 (d, 6H), 3.2 (m, 1H), 6.3 (s, 1H), 6.6 (t, 1H), 7.0 (m, 1H), 7.4 (d, 1H), 8.4 (d, 1H). HPLC: RT=9.1 min (99.6 area %).
CLIP
Ibudilast (3-isobutyryl-2-isopropylpyrazolo[l,5-α]pyridine) is a small molecule drug that has been used for many years in Japan and Korea for the treatment of bronchial asthma as well as for treatment of cerebrovascular disorders such as post-stroke dizziness. It is sold in these countries under the tradename, Ketas®. Marketed indications for ibudilast in Japan include its use as a vasodilator, for treating allergy, eye tissue regeneration, ocular disease, and treatment of allergic ophthalmic disease (Thompson Current Drug Reports). Its use in the treatment of both chronic brain infarction (ClinicalTrials.gov) and multiple sclerosis (News.Medical.Net; Pharmaceutical News, 2 Aug 2005) is currently being explored in separate, ongoing clinical trials.
The mechanisms of action of ibudilast have been widely explored. Its role as a non-selective inhibitor of cyclic nucleotide phosphodiesterase (PDE) has been described
(Fujimoto, T., et al., J. of Neuroimmunology, 95 (1999) 35-92). Additionally, ibudilast has been reported to act as an LTD4 antagonist, an anti-inflammatory, a PAF antagonist, and a vasodilatator agent (Thompson Current Drug Reports). Ibudilast is also thought to exert a neuroprotective role in the central nervous system of mammals, presumably via suppression of the activation of glial cells (Mizuno et al. (2004) Neuropharmacology 46: 404-411). New uses for ibudilast continue to be explored.http://www.google.com/patents/WO2007146087A2?cl=en
PATENT
http://www.google.com/patents/WO2007142924A1?cl=en
IBUDILAST
Ibudilast is a small molecule drug (molecular weight of 230.3) having the structure shown below.
Ibudilast is also found under ChemBank ID 3227, CAS # 50847-1 1-5, and Beilstein Handbook Reference No. 5-24-03-00396. Its molecular formula corresponds to [Ci4HIgN2O]. Ibudilast is also known by various chemical names which include 2- methyl-l-(2-(l-methylethyI)pyrazolo(l,5-a)pyridin-3-yl)l-propanone; 3-isobutyryl-2- isopropylpyrazolo(l,5-a)pyridine]; and l-(2-isopropyl-pyrazolo[l,5-a]pyridin-3-yl)-2- methyl-propan-1-one. Other synonyms for ibudilast include Ibudilastum (Latin), BRN 0656579, KC-404, and the brand name Ketas®. Ibudilast, as referred to herein, is meant to include any and all pharmaceutically acceptable salt forms thereof, prodrug forms (e.g., the corresponding ketal), and the like, as appropriate for use in its intended formulation for administration.
Ibudilast is a non-selective nucleotide phosphodiesterase (PDE) inhibitor (most active against PDE-3 and PDE-4), and has also been reported to have LTD4 and PAF antagonistic activities. Its profile appears effectively anti-inflammatory and unique in comparison to other PDE inhibitors and anti-inflammatory agents. PDEs catalyze the hydrolysis of the phosphoester bond on the 3 ‘-carbon to yield the corresponding 5′- nucleotide monophosphate. Thus, they regulate the cellular concentrations of cyclic nucleotides. Since extracellular receptors for many hormones and neurotransmitters utilize cyclic nucleotides as second messengers, the PDEs also regulate cellular responses to these extracellular signals. There are at least eight classes of PDEs: Ca2+/calmodul in-dependent PDEs (PDEl); cGMP-stimulated PDEs (PDE2); cGMP- inhibited PDEs (PDE3); cAMP-specific PDEs (PDE4); cGMP-binding PDEs (PDE5); photoreceptor PDEs (PDE6); high affinity, cAMP-specific PDEs (PDE7); and high affinity cGMP-specific PDEs (PDE9).
SYNTHESIS

DE 2315801; FR 2182914; JP 7714799, WO 0196278
By condensation of 1-amino-2-methylpyridinium iodide (I) with isobutyric anhydride (II) by means of K2CO3 at reflux temperature.
Patent
PATENT
2-methyl -l- [2- (l- methylethyl) – pyrazolo [l, 5_a] pyrimidine _3_ yl] _1_ acetone (ibudilast, generic drug name: IBUDILAST ) is an anti-allergic asthma drugs, anti-leukotrienes can twist and platelet-activating factor, promote the secretion of mucus in the respiratory tract, respiratory cilia function, enhance the role of prostacyclin, increase cerebral blood flow, improve brain metabolism. For the treatment of bronchial asthma, sequelae of cerebral embolism, cerebral arteriosclerosis.
ibudilast preparation methods are mainly the following two:
Method a: (The Jourrtal of Organic Chemistry, 1968, 33, 3766 ~3770) Synthesis Road
Lines are as follows:
The route to 2-picoline as starting material to give amino-2-methyl-pyridine iodide I-, after pyrimidine, the role of isobutyryl chloride to give the title compound. The final product obtained by this route need be purified by column chromatography, thereby increasing the difficulty of the operation, in addition to column chromatography, eluent used larger benzene toxicity, is not suitable for industrial production.
Method II: (Journal of the American Chemical Society, 2005,127, 751-760) co
A route is as follows:
The route to 2-picoline as starting material to obtain the sulfamic acid, potassium iodide I- amino-2-picoline under the action of potassium carbonate, then with isobutyric anhydride to give the title compound effect. This route of the first-stage reaction process locked, the yield is low, is not suitable for industrial production.
so there ibudilast conventional method for preparing the operational difficulties or low yield, making it impossible to achieve industrial production problems.
DETAILED DESCRIPTION IX: with a specific embodiment of the present embodiment is one of one to eight different points: in the second step of the recrystallization specific operation is as follows: First, the collected fractions was cooled to 10 ° c~25 ° C, to give a pale yellow solid, and then n-hexane was added to the pale yellow solid, and the temperature was raised to 50 ° C~68 ° C, at a temperature of 50 ° C~68 ° C incubation 5min~IOmin, then cooled to 10 ° C~ 25 ° C, and at a temperature of 10 ° C~25 ° C incubated O. 5h~Ih, and finally filtered to obtain ibudilast; the volume of the pale yellow solid quality and hexane ratio of Ig: (ImL~2mL), to obtain ibudilast.
PAPER
Bioorganic & medicinal chemistry letters (2011), 21(11), 3307-12.
Ibudilast [1-(2-isopropylpyrazolo[1,5-a]pyridin-3-yl)-2-methylpropan-1-one] is a nonselective phosphodiesterase inhibitor used clinically to treat asthma. Efforts to selectively develop the PDE3- and PDE4-inhibitory activity of ibudilast led to replacement of the isopropyl ketone by a pyridazinone heterocycle. Structure–activity relationship exploration in the resulting 6-(pyrazolo[1,5-a]pyridin-3-yl)pyridazin-3(2H)-ones revealed that the pyridazinone lactam functionality is a critical determinant for PDE3-inhibitory activity, with the nitrogen preferably unsubstituted. PDE4 inhibition is strongly promoted by introduction of a hydrophobic substituent at the pyridazinone N(2) centre and a methoxy group at C-7′ in the pyrazolopyridine. Migration of the pyridazinone ring connection from the pyrazolopyridine 3′-centre to C-4′ strongly enhances PDE4 inhibition. These studies establish a basis for development of potent PDE4-selective and dual PDE3/4-selective inhibitors derived from ibudilast.
UPDATE AS ON JAN 2016
…………..MediciNova’s ibudilast gets FDA rare paediatric disease status to treat Krabbe disease
MediciNova has received rare paediatric disease status from the US Food and Drug Administration (FDA) for its MN-166 (ibudilast) to treat Type 1 Early Infantile Krabbe disease.

References
- Huang Z, Liu S, Zhang L, Salem M, Greig GM, Chan CC, Natsumeda Y, Noguchi K. Preferential inhibition of human phosphodiesterase 4 by ibudilast. Life Sciences. 2006 May 1;78(23):2663-8.
- Suzumura A, Ito A, Yoshikawa M, Sawada M. Ibudilast suppresses TNFalpha production by glial cells functioning mainly as type III phosphodiesterase inhibitor in the CNS. Brain Research. 1999 Aug 7;837(1-2):203-12.
- Gibson LC, Hastings SF, McPhee I, Clayton RA, Darroch CE, Mackenzie A, Mackenzie FL, Nagasawa M, Stevens PA, Mackenzie SJ. The inhibitory profile of Ibudilast against the human phosphodiesterase enzyme family. European Journal of Pharmacology. 2006 May 24;538(1-3):39-42.
- Kishi Y, Ohta S, Kasuya N, Sakita S, Ashikaga T, Isobe M. Ibudilast: a non-selective PDE inhibitor with multiple actions on blood cells and the vascular wall. Cardiovascular Drug Reviews. 2001 Fall;19(3):215-25.
- Mizuno T, Kurotani T, Komatsu Y, Kawanokuchi J, Kato H, Mitsuma N, Suzumura A. Neuroprotective role of phosphodiesterase inhibitor ibudilast on neuronal cell death induced by activated microglia. Neuropharmacology. 2004 Mar;46(3):404-11.
- Yoshioka M, Suda N, Mori K, Ueno K, Itoh Y, Togashi H, Matsumoto M. Effects of ibudilast on hippocampal long-term potentiation and passive avoidance responses in rats with transient cerebral ischemia. Pharmacological Research. 2002 Apr;45(4):305-11.
- Wakita H, Tomimoto H, Akiguchi I, Lin JX, Ihara M, Ohtani R, Shibata M. Ibudilast, a phosphodiesterase inhibitor, protects against white matter damage under chronic cerebral hypoperfusion in the rat. Brain Research. 2003 Nov 28;992(1):53-9.
- Rile G, Yatomi Y, Qi R, Satoh K, Ozaki Y. Potentiation of ibudilast inhibition of platelet aggregation in the presence of endothelial cells. Thrombosis Research. 2001 May 1;102(3):239-46.
- Feng J, Misu T, Fujihara K, Sakoda S, Nakatsuji Y, Fukaura H, Kikuchi S, Tashiro K, Suzumura A, Ishii N, Sugamura K, Nakashima I, Itoyama Y. Ibudilast, a nonselective phosphodiesterase inhibitor, regulates Th1/Th2 balance and NKT cell subset in multiple sclerosis. Multiple Sclerosis. 2004 Oct;10(5):494-8.
- Ledeboer A, Hutchinson MR, Watkins LR, Johnson KW. Ibudilast (AV-411). A new class therapeutic candidate for neuropathic pain and opioid withdrawal syndromes. Expert Opinion on Investigational Drugs. 2007 Jul;16(7):935-50.
- http://www.huffingtonpost.com/2013/04/03/meth-addiction-cure-ucla-ibudilast_n_2863126.html?utm_hp_ref=mostpopular#slide=more268305
- http://onlinelibrary.wiley.com/doi/10.1111/adb.12106/abstrac
SEE……Synthesis technology of ibudilast
Shandong Huagong (2014), 43, (8), 29-30. Publisher: (Shandong Huagong Bianjibu, ) CODEN:SHHUA4 ISSN:1008-021X.
Literature References:
Leukotriene D4 antagonist. Prepn: T. Irikura et al., DE 2315801; eidem, US 3850941 (1973, 1974 both to Kyorin).
Pharmacology and antiallergic activity: K. Nishino et al., Jpn. J. Pharmacol. 33, 267 (1983); H. Nagai et al., ibid. 1215.
In vitro cerebral vasodilating activity: M. Ohashi et al., Arch. Int. Pharmacodyn. 280, 216 (1986);
in vivo activity: W. M. Armstead et al., J. Pharmacol. Exp. Ther. 244, 138 (1988).
Bronchodilating activity in animals: S. Mue et al., Arch. Int. Pharmacodyn. 283,153 (1986).
Antiplatelet activity in animals: M. Ohashi et al., ibid. 321; M. Ohashi et al., Gen. Pharmacol. 17, 385 (1986).

| Patent | Submitted | Granted |
|---|---|---|
| Method for treating neuropathic pain and associated syndromes [US7534806] | 2006-07-20 | 2009-05-19 |
| Synergistic combination [US2006205806] | 2006-09-14 | |
| Pharmaceutical composition of a pde4 or pde 3/4 inhibitor and histamine receptor antagonist [US2005112069] | 2005-05-26 | |
| Methods and reagents for the treatment of immunoinflammatory disorders [US2005119160] | 2005-06-02 | |
| Methods of inducing ovulation using a non-polypeptide camp level modulator [US7507707] | 2005-07-07 | 2009-03-24 |
| Methods and reagents for the treatment of immunoinflammatory disorders [US2005192261] | 2005-09-01 | |
| Synergistic combination [US7056936] | 2004-02-19 | 2006-06-06 |
| Methods for the treatment of respiratory diseases and conditions with a selective iNOS inhibitor and a PDE inhibitor and compositions therefor [US2004087653] | 2004-05-06 | |
| Remedies for multiple sclerosis [US6395747] | 2002-05-28 | |
| Combination [US2005014762] | 2005-01-20 |
| Patent | Filing date | Publication date | Applicant | Title |
|---|---|---|---|---|
| US4097483 | Aug 31, 1976 | Jun 27, 1978 | Kyorin Pharmaceutical Co., Ltd. | Pyrazolo 1,5-a!pyridines |
| US7585875 * | Jun 6, 2007 | Sep 8, 2009 | Avigen, Inc. | Phosphodiesterase inhibitors; neuropathic pain, inflammation, opioid dependence or withdrawal; 2-amino-1-(2-isopropylpyrazolo[1,5-a]pyridin-3-yl)propan-1-one for example |
| US20070015924 | Jun 15, 2006 | Jan 18, 2007 | Cardiome Pharma Corp. | stereoselective preparation of aminocyclohexyl ether compounds such as trans-(1R,2R)-aminocyclohexyl ether compounds and/or trans-(1S,2S)-aminocyclohexyl ether compounds; useful in treating arrhythmias |
| US20080070912 | Jun 6, 2007 | Mar 20, 2008 | Avigen, Inc. | Phosphodiesterase inhibitors; neuropathic pain, inflammation, opioid dependence or withdrawal; 2-amino-1-(2-isopropylpyrazolo[1,5-a]pyridin-3-yl)propan-1-one for example |
| US20090062330 | Jul 8, 2008 | Mar 5, 2009 | Medicinova, Inc. | Treatment of progressive neurodegenerative disease with ibudilast |
| US20090318437 * | Jun 10, 2009 | Dec 24, 2009 | Gaeta Federico C A | SUBSTITUTED PYRAZOLO[1,5-a] PYRIDINE COMPOUNDS AND THEIR METHODS OF USE |
| WO2007142924A1 | May 29, 2007 | Dec 13, 2007 | Avigen Inc | Ibudilast for inhibiting macrophage migration inhibitory factor (mif) activity |
| WO2007146087A2 * | Jun 6, 2007 | Dec 21, 2007 | Avigen Inc | SUBSTITUTED PYRAZOLO [1,5-α] PYRIDINE COMPOUNDS AND THEIR METHODS OF USE |
| WO2010151551A1 * | Jun 22, 2010 | Dec 29, 2010 | Medicinova, Inc. | ENANTIOMERIC COMPOSITIONS OF 2-AMINO-1-(2-ISOPROPYLPYRAZOLO[1,5-a]PYRIDIN-3-YL)PROPAN-1-ONE AND RELATED METHODS |
| US8119657 | Jun 22, 2010 | Feb 21, 2012 | Medicinova, Inc. | Enantiomeric compositions of 2-amino-1-(2-isopropylpyrazolo[1,5-α]pyridin-3-yl)propan-1-one and related methods |
| Patent | Filing date | Publication date | Applicant | Title |
|---|---|---|---|---|
| WO2003104178A1 * | Jun 6, 2003 | Dec 18, 2003 | Cortical Pty Ltd | Napththalene derivatives which inhibit the cytokine or biological activity of macrophage migration inhibitory factor (mif) |
| WO2003104203A1 * | Jun 6, 2003 | Dec 18, 2003 | Cortical Pty Ltd | Therapeutic molecules and methods-1 |
| WO2004058713A1 * | Dec 18, 2003 | Jul 15, 2004 | Jason Chyba | Differential tumor cytotoxocity compounds and compositions |
| WO2005058304A1 * | Dec 17, 2004 | Jun 30, 2005 | Cortical Pty Ltd | Implantable device containing inhibitor of macrophage migration inhibitory factor |
| WO2006045505A1 * | Oct 19, 2005 | May 4, 2006 | Novartis Ag | Mif-inhibitors |
| WO2006108671A1 * | Apr 13, 2006 | Oct 19, 2006 | Novartis Ag | 3,4-dihydro-benzo[e][1,3]oxazin-2-ones |
 |
|
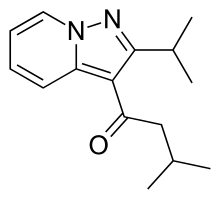
| Systematic (IUPAC) name | |
|---|---|
|
2-methyl-1-(2-propan-2-ylpyrazolo[1,5-a]pyridin-3-yl)propan-1-one
|
|
| Clinical data | |
| AHFS/Drugs.com | International Drug Names |
| Identifiers | |
| CAS Number | 50847-11-5 |
| ATC code | R03DC04 |
| PubChem | CID: 3671 |
| IUPHAR/BPS | 7399 |
| DrugBank | DB05266 |
| ChemSpider | 3543 |
| UNII | M0TTH61XC5 |
| KEGG | D01385 |
| ChEMBL | CHEMBL19449 |
| Chemical data | |
| Formula | C14H18N2O |
| Molecular mass | 230.31 g/mol |
Keywords: Antiallergic; Antiasthmatic (Nonbronchodilator); Leukotriene Antagonist; Vasodilator (Cerebral).

SEE………http://apisynthesisint.blogspot.in/2016/01/ibudilast.html
////////////////////
CC(C)C1=NN2C=CC=CC2=C1C(=O)C(C)C
BioMarin gets US priority review for rare disease drug

31 may 2013
BioMarin will be celebrating news that regulators on both sides of the Atlantic have agreed to review Vimzin under accelerated review processes.
Vimzin is an enzyme replacement therapy for which the drugmaker is seeking approval as a treatment for the rare lysosomal storage disorder Mucopolysaccharidosis Type IVA (MPS IVA), also known as Morquio A Syndrome.
During an initial review of the Biologics License Application the US Food and Drug Administration requested extra Chemistry, Manufacturing and Controls information, and following receipt of this from BioMarin it has extended the PDUFA action date by three months to February 28 next year.
In the EU, assuming the marketing application remains on the accelerated assessment timeline, a CHMP opinion is anticipated in December this year, which means a decision from the European Commission could be handed down in the first quarter of 2014, the firm said.
The estimated prevalence of MPS IVA is around 3,000 patients in the developed world, and it is believed that around 20% or patients are in North America and 50% in Europe.

 DRUG APPROVALS BY DR ANTHONY MELVIN CRASTO
.....
DRUG APPROVALS BY DR ANTHONY MELVIN CRASTO
.....