Home » Articles posted by DR ANTHONY MELVIN CRASTO Ph.D (Page 25)
Author Archives: DR ANTHONY MELVIN CRASTO Ph.D
Omaveloxolone



Omaveloxolone
CAS
1474034-05-3
N-[(4aS,6aR,6bS,8aR,12aS,14aR,14bS)-11-cyano-2,2,6a,6b,9,9,12a-heptamethyl-10,14-dioxo-1,2,3,4,4a,5,6,6a,6b,7,8,8a,9,10,12a,14,14a,14b-octadecahydropicen-4a-yl]-2,2-difluoropropanamide
N-[(4aS,6aR,6bS,8aR,12aS,14aR,14bS)-11-cyano-2,2,6a,6b,9,9,12a-heptamethyl-10,14-dioxo-1,3,4,5,6,7,8,8a,14a,14b-decahydropicen-4a-yl]-2,2-difluoropropanamide
FDA 2023, 2/28/2023, To treat Friedrich’s ataxia
Drug Trials Snapshot
WeightAverage: 554.723
Monoisotopic: 554.331999611
Chemical FormulaC33H44F2N2O3
- RTA 408
- RTA-408
- OriginatorDartmouth College; University of Texas M. D. Anderson Cancer Center
- DeveloperBiogen
- ClassAnalgesics; Anti-inflammatories; Antineoplastics; Eye disorder therapies; Neuroprotectants; Small molecules; Triterpenes
- Mechanism of ActionNF-E2-related factor 2 stimulants
- Orphan Drug StatusYes – Friedreich’s ataxia; Malignant melanoma
- MarketedFriedreich’s ataxia
- Phase IIMitochondrial disorders; Ocular inflammation; Ocular pain
- Phase I/IIMalignant melanoma
- PreclinicalBrain disorders
- DiscontinuedDuchenne muscular dystrophy; Non-small cell lung cancer; Radiation-induced skin damage
- 08 Apr 2025Biogen completes a phase I pharmacokinetics trial (In volunteers) in USA (PO) (NCT06612879)
- 17 Mar 2025Registered for Friedreich’s ataxia (In adolescents, In adults) in Canada (PO)
- 18 Oct 2024Biogen initiates enrolment in a phase I pharmacokinetics trial (In volunteers) in USA (PO) (NCT06612879)
Omaveloxolone, sold under the brand name Skyclarys, is a medication used for the treatment of Friedreich’s ataxia.[2][5] It is taken by mouth.[2]
The most common side effects include an increase in alanine transaminase and an increase of aspartate aminotransferase, which can be signs of liver damage, headache, nausea, abdominal pain, fatigue, diarrhea and musculoskeletal pain.[5]
Omaveloxolone was approved for medical use in the United States in February 2023,[2][5][6][7][8] and in the European Union in February 2024.[3] The US Food and Drug Administration (FDA) considers it to be a first-in-class medication.[9]
SYNTHESIS

PATENT
Sheikh, AY et al. (2018). Bardoxolonmethyl-2,2-difluoropropionamide derivatives, polymorphe forms and procedures for use thereof. DK/EP 2989114 T3. Danish Patent and Trademark Office. Available at https://patentimages.storage.googleapis.com/51/87/43/97d0fb3e69ee73/DK2989114T3.pdf
https://patentscope.wipo.int/search/en/detail.jsf?docId=EP159939262&_cid=P21-MAKI10-93498-1

[0164] Reagents and conditions: (a) (PhO) 2PON 3 (DPPA), triethylamine, toluene, 0 °C for 5 minutes, then ambient temperature overnight, ∼94%; (b) benzene, 80 °C for 2 hours; (c) HCl, CH 3CN, ambient temperature for 1 hour; (d) CH 3CF 2CO 2H, dicyclohexylcarbodiimide, 4-(dimethylamino)pyridine, CH 2Cl 2, ambient temperature overnight, 73% from RTA 401 (4 steps).
[0165]Compound 1: RTA 401 (20.0 g, 40.6 mmol), triethylamine (17.0 mL, 122.0 mmol), and toluene (400 mL) were added into a reactor and cooled to 0 °C with stirring. Diphenyl phosphoryl azide (DPPA) (13.2 mL, 61.0 mmol) was added with stirring at 0 °C over 5 minutes, and the mixture was continually stirred at room temperature overnight (HPLC-MS check shows no RTA 401 left). The reaction mixture was directly loaded on a silica gel column and purified by column chromatography (silica gel, 0% to 5% ethyl acetate in CH 2Cl 2) to give compound 1 (19.7 g, ∼94%, partially converted into compound 2) as a white foam.
[0166]Compound 2: Compound 1 (19.7 g, ∼38.1 mmol) and benzene (250 mL) were added into a reactor and heated to 80 °C with stirring for 2 hours (HPLC-MS check shows no compound 1 left). The reaction mixture was concentrated at reduced pressure to afford crude compound 2 as a solid residue, which was used for the next step without purification.
[0167]Compound 3: Crude compound 2 (≤38.1 mmol) and CH 3CN (200 mL) were added into a reactor and cooled to 0 °C with stirring. HCl (12 N, 90 mL) was added at 0 °C over 1 minute, and the mixture was continually stirred at room temperature for 1 hour (HPLC-MS check shows no compound 2 left). The reaction mixture was cooled to 0 °C and 10% NaOH (∼500 mL) was added with stirring. Then, saturated NaHCO 3 (1 L) was added with stirring. The aqueous phase was extracted by ethyl acetate (2×500 mL). The combined organic phase was washed by H 2O (200 mL), saturated NaCl (200 mL), dried over Na 2SO 4, and concentrated to afford crude compound 3 (16.62 g) as a light yellow foam, which was used for the next step without purification.
[0168]RTA 408: Crude amine 3 (16.62 g, 35.9 mmol), CH 3CF 2CO 2H (4.7388 g, 43.1 mmol), and CH 2Cl 2 (360 mL) were added into a reactor with stirring at room temperature. Then, dicyclohexylcarbodiimide (DCC) (11.129 g, 53.9 mmol) and 4-(dimethylamino)pyridine (DMAP) (1.65 g, 13.64 mmol) were added and the mixture was continually stirred at room temperature overnight (HPLC-MS check shows no compound 3 left). The reaction mixture was filtered to remove solid by-products, and the filtrate was directly loaded on a silica gel column and purified by column chromatography (silica gel, 0% to 20% ethyl acetate in hexanes) twice to give compound RTA 408 (16.347 g, 73% from RTA 401 over 4 steps) as a white foam: 1H NMR (400 MHz, CD 3Cl) δ ppm 8.04 (s, 1H), 6.00 (s, 1H), 5.94 (s, br, 1H), 3.01 (d, 1H, J = 4.8 Hz), 2.75-2.82 (m, 1H), 1.92-2.18 (m, 4H), 1.69-1.85 (m, 7H), 1.53-1.64 (m, 1H), 1.60 (s, 3H), 1.50 (s, 3H), 1.42 (s, 3H), 1.11-1.38 (m, 3H), 1.27 (s, 3H), 1.18 (s, 3H), 1.06 (s, 3H), 1.04 (s, 3H), 0.92 (s, 3H); m/z 555 (M+1).
SYNTHESIS
J. Med. Chem. 2025, 68, 2147−2182
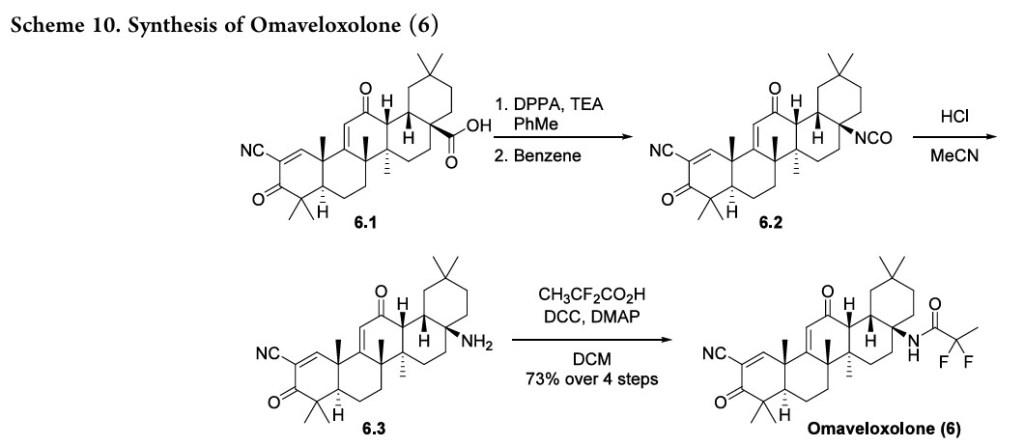
Omaveloxolone (Skyclarys). Omaveloxolone (6) was approved in February 2023 for the treatment of Friedreich’s Ataxia (FRDA), a genetic, neurodegenerative disease. Patients with FRDA have lowered activity of the frataxin gene (FXN), attributed to an expansion of a guanine-adenine-adenine (GAA)
triplet. The resulting decrease in frataxin limits the production of iron−sulfur clusters, leading to accumulation of iron in the mitochondria and oxidative stress which in turn leads to cell damageanddeath.49
Omaveloxoloneactivates the nuclear factor erythroid 2-related factor 2 (Nrf2), an important pathway in
oxidative stress. It acts by preventing ubiquitination and subsequent degradation of Nrf2, keeping levels high enough to counteract the oxidative stress associated with FRDA. 50
Omaveloxolone was developed by Reata Pharmaceuticals (which was acquired by Biogen in September 2023) and was granted orphan drug, fast track, priority review, and rare pediatric disease designations. 51Omaveloxolone (6) is a semisynthetic triterpenoid based on the oleanolic acid scaffold.52
advanced intermediate 6.1,The synthesis started from the53also known as CDDO orbardoxolone, which has individually been investigated fortherapeutic benefits from Nrf2 activation (Scheme 10).
Treatment of acid 6.1 with DPPA produced the azide, and subsequent heating in benzene generated isocyanate 6.2 via aCurtius rearrangement. Hydrolysis with aqueous acid generated amine 6.3, and an amidation with 2,2-difluoropropanoic acid produced omaveloxolone (6). A yield of 73% over the sequence was reported, and intermediates were used crude with no purification between steps.
(49) Ghanekar, S. D.; Miller, W. W.; Meyer, C. J.; Fenelon, K. J.;
Lacdao, A.; Zesiewicz, T. A. Orphan drugs in development for the
treatment of Friedreich’s ataxia: focus on omaveloxolone. Degener.
Neurol. Neuromuscular Dis. 2019, 9, 103−107.
(50) Abeti, R.; Baccaro, A.; Esteras, N.; Giunti, P. Novel Nrf2-inducer
prevents mitochondrial defects and oxidative stress in Friedreich’s
ataxia models. Front. Cell. Neurosci. 2018, 12, 188.
(51) Lee,A.Omaveloxolone:first approval. Drugs 2023, 83, 725−729.
(52) Anderson, E.; Decker, A.; Liu, X. Synthesis, pharmaceutical use,
and characterization of crystalline forms of 2,2-difluoropropionamide
derivatives of bardoxolone methyl. WO 2013163344, 2013.
(53) Honda, T.; Rounds, B. V.; Gribble, G. W.; Suh, N.; Wang, Y.;
Sporn, M. B. Design and synthesis of 2-cyano-3,12-dioxoolean-1,9
dien-28-oic acid, a novel and highly active inhibitor of nitric oxide
production in mouse macrophages. Bioorg. Med. Chem. Lett. 1998, 8,
2711−2714.
SYN
European Journal of Medicinal Chemistry 265 (2024) 116124
Omaveloxolone (Skyclarys)
Omaveloxolone was granted FDA approval on February 28, 2023, to treat Friedrich’s ataxia in individuals aged 16 and older [2]. Omaveloxolone possesses antioxidant and anti-inflammatory properties, making it a semi-synthetic triterpenoid compound. It has the ability to function as a stimulator of nuclear factor-erythroid 2 related factor 2(Nrf2), a transcription factor that reduces oxidative stress. In individuals
suffering from FA, a genetic disorder characterized by mitochondrial dysfunction, the Nrf2 pathway is compromised, leading to a decrease in Nrf2 activity. Hence, Omaveloxolone, an Nrf2 activator, can be
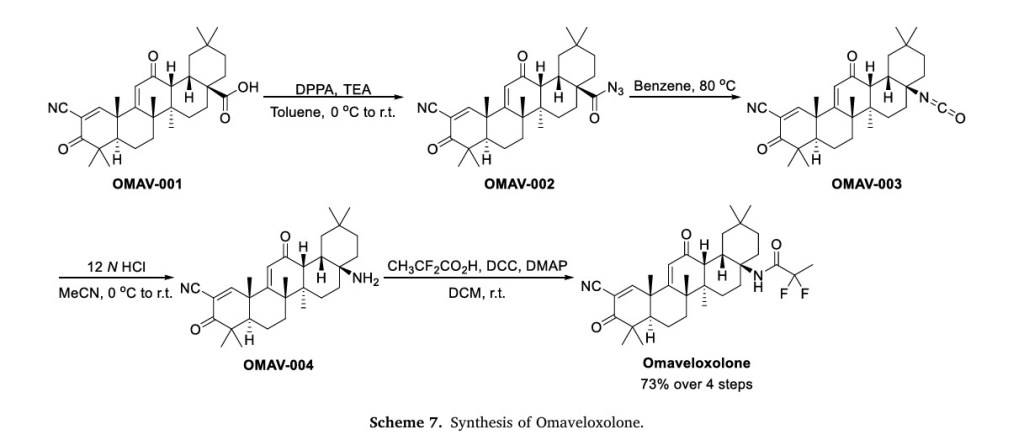
employed as a therapeutic option for the management of these in dividuals [23].The process route of Omaveloxolone is described below in Scheme 724]. The substitution reaction of carboxylic acid OMAV-001 with diphenylphosphoryl azide (DPPA) gave the acyl azide OMAV-002,which underwent Curtius-rearrangement under heating conditions to produce isocyanate OMAV-003. The amine OMAV-004 was obtained under acidic conditions. OMAV-004 was condensed with 2,2-difluoro propionic acid to obtain the final product Omaveloxolone.
[23] B.L. Probst, I. Trevino, L. McCauley, R. Bumeister, I. Dulubova, W.C. Wigley, D.
A. Ferguson, RTA 408, A novel synthetic triterpenoid with broad anticancer and
anti-inflammatory activity, PLoS One 10 (2015) e0122942.
[24] E. Anderson, A. Decker, X. Liu Synthesis, Pharmaceutical Use, and
Characterization of Crystalline Forms of 2,2-difluoropropionamide Derivatives of
Bardoxolone Methyl, 2013. WO2013163344.
.
Medical uses
Omaveloxolone is indicated for the treatment of Friedreich’s ataxia.[2][5]
Friedreich’s ataxia causes progressive damage to the spinal cord, peripheral nerves, and the brain, resulting in uncoordinated muscle movement, poor balance, difficulty walking, changes in speech and swallowing, and a shortened lifespan.[5] The condition can also cause heart disease.[5] This disease tends to develop in children and teenagers and gradually worsens over time.[5]
Although rare, Friedreich’s ataxia is the most common form of hereditary ataxia in the United States, affecting about one in every 50,000 people.[5]
Mechanism of action
The mechanism of action of omaveloxolone and its related compounds has been demonstrated to be through a combination of activation of the antioxidative transcription factor Nrf2 and inhibition of the pro-inflammatory transcription factor NF-κB.[10]
Nrf2 transcriptionally regulates multiple genes that play both direct and indirect roles in producing antioxidative potential and the production of cellular energy (i.e., adenosine triphosphate or ATP) within the mitochondria. Consequently, unlike exogenously administered antioxidants (e.g., vitamin E or Coenzyme Q10), which provide a specific and finite antioxidative potential, omaveloxolone, through Nrf2, broadly activates intracellular and mitochondrial antioxidative pathways, in addition to pathways that may directly increase mitochondrial biogenesis (such as PGC1α) and bioenergetics.[11]
History
Omaveloxolone is a second generation member of the synthetic oleanane triterpenoid compounds and in clinical development by Reata Pharmaceuticals. Preclinical studies have demonstrated that omaveloxolone possesses antioxidative and anti-inflammatory activities[10][12] and the ability to improve mitochondrial bioenergetics.[11] Omaveloxolone is under clinical investigation for a variety of indications, including Friedreich’s ataxia, mitochondrial myopathies, immunooncology, and prevention of corneal endothelial cell loss following cataract surgery.
The efficacy and safety of omaveloxolone was evaluated in a 48-week randomized, placebo-controlled, and double-blind study [Study 1 (NCT02255435)] and an open-label extension.[5] Study 1 enrolled 103 individuals with Friedreich’s ataxia who received placebo (52 individuals) or omaveloxolone 150 mg (51 individuals) for 48 weeks.[5] Of the research participants, 53% were male, 97% were white, and the mean age was 24 years at study entry.[5] Nine (18%) patients were younger than age 18.[5] The primary objective was to evaluate the change in the modified Friedreich’s Ataxia Rating Scale (mFARS) score compared to placebo at week 48.[5] The mFARS is a clinical assessment that measures disease progression, namely swallowing and speech (bulbar), upper limb coordination, lower limb coordination, and upright stability.[5] Individuals receiving omaveloxolone performed better on the mFARS than people receiving placebo.[5]
The US Food and Drug Administration (FDA) granted the application for omaveloxolone orphan drug, fast track, priority review, and rare pediatric disease designations.[5][9]
Society and culture
Legal status
Omaveloxolone was approved for medical use in the United States in February 2023.[2][5]
In December 2023, the Committee for Medicinal Products for Human Use (CHMP) of the European Medicines Agency adopted a positive opinion, recommending the granting of a marketing authorization for the medicinal product Skyclarys, intended for the treatment of Friedreich’s ataxia.[3] The applicant for this medicinal product is Reata Ireland Limited.[3] Omaveloxolone was approved for medical use in the European Union in February 2024.[3][4]
References
- ^ “Register of Innovative Drugs”. Health Canada. 3 November 2006. Retrieved 17 April 2025.
- ^ Jump up to:a b c d e f “Skyclarys- omaveloxolone capsule”. DailyMed. 12 May 2023. Archived from the original on 1 July 2023. Retrieved 16 December 2023.
- ^ Jump up to:a b c d e “Skyclarys EPAR”. European Medicines Agency (EMA). 14 December 2023. Archived from the original on 15 December 2023. Retrieved 16 December 2023. Text was copied from this source which is copyright European Medicines Agency. Reproduction is authorized provided the source is acknowledged.
- ^ Jump up to:a b “Skyclarys product information”. Union Register of medicinal products. 12 February 2024. Retrieved 19 February 2024.
- ^ Jump up to:a b c d e f g h i j k l m n o p q “FDA approves first treatment for Friedreich’s ataxia”. U.S. Food and Drug Administration (FDA). 28 February 2023. Archived from the original on 1 March 2023. Retrieved 28 February 2023.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain. - ^ “Reata Pharmaceuticals Announces FDA Approval of Skyclarys (Omavaloxolone), the First and Only Drug Indicated for Patients with Friedreich’s Ataxia”. Reata Pharmaceuticals Inc. (Press release). 28 February 2023. Archived from the original on 1 March 2023. Retrieved 28 February 2023.
- ^ Lee A (June 2023). “Omaveloxolone: First Approval”. Drugs. 83 (8): 725–729. doi:10.1007/s40265-023-01874-9. PMID 37155124. S2CID 258567442. Archived from the original on 9 December 2023. Retrieved 16 December 2023.
- ^ Subramony SH, Lynch DL (May 2023). “A Milestone in the Treatment of Ataxias: Approval of Omaveloxolone for Friedreich Ataxia”. Cerebellum. 23 (2): 775–777. doi:10.1007/s12311-023-01568-8. PMID 37219716. S2CID 258843532.
- ^ Jump up to:a b New Drug Therapy Approvals 2023 (PDF). U.S. Food and Drug Administration (FDA) (Report). January 2024. Archived from the original on 10 January 2024. Retrieved 9 January 2024.
- ^ Jump up to:a b Reisman SA, Lee CY, Meyer CJ, Proksch JW, Ward KW (July 2014). “Topical application of the synthetic triterpenoid RTA 408 activates Nrf2 and induces cytoprotective genes in rat skin”. Archives of Dermatological Research. 306 (5): 447–454. doi:10.1007/s00403-013-1433-7. PMID 24362512. S2CID 25733020.
- ^ Jump up to:a b Neymotin A, Calingasan NY, Wille E, Naseri N, Petri S, Damiano M, et al. (July 2011). “Neuroprotective effect of Nrf2/ARE activators, CDDO ethylamide and CDDO trifluoroethylamide, in a mouse model of amyotrophic lateral sclerosis”. Free Radical Biology & Medicine. 51 (1): 88–96. doi:10.1016/j.freeradbiomed.2011.03.027. PMC 3109235. PMID 21457778.
- ^ Reisman SA, Lee CY, Meyer CJ, Proksch JW, Sonis ST, Ward KW (May 2014). “Topical application of the synthetic triterpenoid RTA 408 protects mice from radiation-induced dermatitis”. Radiation Research. 181 (5): 512–520. Bibcode:2014RadR..181..512R. doi:10.1667/RR13578.1. PMID 24720753. S2CID 23906747.
External links
Clinical trial number NCT02255435 for “RTA 408 Capsules in Patients With Friedreich’s Ataxia – MOXIe” at ClinicalTrials.gov
| Clinical data | |
|---|---|
| Trade names | Skyclarys |
| Other names | RTA 408 |
| AHFS/Drugs.com | Monograph |
| License data | US DailyMed: Omaveloxolone |
| Routes of administration | By mouth |
| ATC code | N07XX25 (WHO) |
| Legal status | |
| Legal status | CA: ℞-only[1]US: ℞-only[2]EU: Rx-only[3][4] |
| Identifiers | |
| showIUPAC name | |
| CAS Number | 1474034-05-3 |
| PubChem CID | 71811910 |
| IUPHAR/BPS | 7573 |
| DrugBank | DB12513 |
| ChemSpider | 34980948 |
| UNII | G69Z98951Q |
| KEGG | D10964 |
| ChEBI | CHEBI:229661 |
| CompTox Dashboard (EPA) | DTXSID101138251 |
| Chemical and physical data | |
| Formula | C33H44F2N2O3 |
| Molar mass | 554.723 g·mol−1 |
| 3D model (JSmol) | Interactive image |
| showSMILES | |
| showInChI | |
- Zesiewicz TA, Hancock J, Ghanekar SD, Kuo SH, Dohse CA, Vega J: Emerging therapies in Friedreich’s Ataxia. Expert Rev Neurother. 2020 Dec;20(12):1215-1228. doi: 10.1080/14737175.2020.1821654. Epub 2020 Sep 21. [Article]
- Jiang Z, Qi G, Lu W, Wang H, Li D, Chen W, Ding L, Yang X, Yuan H, Zeng Q: Omaveloxolone inhibits IL-1beta-induced chondrocyte apoptosis through the Nrf2/ARE and NF-kappaB signalling pathways in vitro and attenuates osteoarthritis in vivo. Front Pharmacol. 2022 Sep 27;13:952950. doi: 10.3389/fphar.2022.952950. eCollection 2022. [Article]
- Shekh-Ahmad T, Eckel R, Dayalan Naidu S, Higgins M, Yamamoto M, Dinkova-Kostova AT, Kovac S, Abramov AY, Walker MC: KEAP1 inhibition is neuroprotective and suppresses the development of epilepsy. Brain. 2018 May 1;141(5):1390-1403. doi: 10.1093/brain/awy071. [Article]
- Probst BL, Trevino I, McCauley L, Bumeister R, Dulubova I, Wigley WC, Ferguson DA: RTA 408, A Novel Synthetic Triterpenoid with Broad Anticancer and Anti-Inflammatory Activity. PLoS One. 2015 Apr 21;10(4):e0122942. doi: 10.1371/journal.pone.0122942. eCollection 2015. [Article]
- Lynch DR, Farmer J, Hauser L, Blair IA, Wang QQ, Mesaros C, Snyder N, Boesch S, Chin M, Delatycki MB, Giunti P, Goldsberry A, Hoyle C, McBride MG, Nachbauer W, O’Grady M, Perlman S, Subramony SH, Wilmot GR, Zesiewicz T, Meyer C: Safety, pharmacodynamics, and potential benefit of omaveloxolone in Friedreich ataxia. Ann Clin Transl Neurol. 2018 Nov 10;6(1):15-26. doi: 10.1002/acn3.660. eCollection 2019 Jan. [Article]
- Zighan M, Arkadir D, Douiev L, Keller G, Miller C, Saada A: Variable effects of omaveloxolone (RTA408) on primary fibroblasts with mitochondrial defects. Front Mol Biosci. 2022 Aug 12;9:890653. doi: 10.3389/fmolb.2022.890653. eCollection 2022. [Article]
- FDA Approved Drug Products: SKYCLARYS (omaveloxolone) capsules for oral use (February 2023) [Link]
- EMA Approved Drug Products: Skyclarys (omaveloxolone) Oral Capsules [Link]
- Health Canada Approved Drug Products: SKYCLARYS (Omaveloxolone) Capsules For Oral Use [Link]
///////////Omaveloxolone, Skyclarys, Friedrich’s ataxia, FDA 2023, APPROVALS 2023, RTA 408, RTA-408, omaveloxolona, RTA 408, 63415, PP415, orphan drug, fast track, priority review, rare pediatric disease



AS ON JUNE2025 4.45 LAKHS VIEWS ON BLOG WORLDREACH AVAILABLEFOR YOUR ADVERTISEMENT

join me on Linkedin
Anthony Melvin Crasto Ph.D – India | LinkedIn
join me on Researchgate
RESEARCHGATE

join me on Facebook
Anthony Melvin Crasto Dr. | Facebook
join me on twitter
Anthony Melvin Crasto Dr. | twitter
+919321316780 call whatsaapp
EMAIL. amcrasto@gmail.com

……
Dasminapant




Dasminapant
CAS 1570231-89-8
| Molecular Weight | 1157.40 |
|---|---|
| Formula | C60H72N10O10S2 |
| APG-1387, SM-1387, E53VN70K2X, INN 12430, APG-1387 UNII-E53VN70K2X APG-1387 (SMAC MIMETIC) SMAC-mimetic APG-1387 IAP Inhibitor APG-1387 |
| (5S,5’S,8S,8’S,10aR,10’aR)-3,3′-[1,3-phenylenebis(sulfonyl)]bis{N-(diphenylmethyl)-5-[(2S)-2-(methylamino)propanamido]-6-oxodecahydropyrrolo[1,2-a][1,5]diazocine-8-carboxamide} |
(5S,8S,10aR)-3-[3-[[(5S,8S,10aR)-8-(benzhydrylcarbamoyl)-5-[[(2S)-2-(methylamino)propanoyl]amino]-6-oxo-1,2,4,5,8,9,10,10a-octahydropyrrolo[1,2-a][1,5]diazocin-3-yl]sulfonyl]phenyl]sulfonyl-N-benzhydryl-5-[[(2S)-2-(methylamino)propanoyl]amino]-6-oxo-1,2,4,5,8,9,10,10a-octahydropyrrolo[1,2-a][1,5]diazocine-8-carboxamide
Dasminapant (APG-1387), a bivalent SMAC mimetic and an IAP antagonist, blocks the activity of IAPs family proteins (XIAP, cIAP-1, cIAP-2, and ML-IAP). Dasminapant induces degradation of cIAP-1 and XIAP proteins, as well as caspase-3 activation and PARP cleavage, which leads to apoptosis. Dasminapant can be used for the research of hepatocellular carcinoma, ovarian cancer, and nasopharyngeal carcinoma.
Dasminapant, also known as APG-1387 and SM-1387, is a IAP inhibitor. APG-1387 promotes the rapid degradation of cIAP1/2 and XIAP, and it exerts an antitumor effect on nasopharyngeal carcinoma cancer stem cells. Further studies show that APG-1387 enhances the chemosensitivity and promotes apoptosis in combination with CDDP and 5-FU of NPC in vitro and vivo.
PATENTS
WO2022012671
PATENT
WO2014031487 …
https://patentscope.wipo.int/search/en/detail.jsf?docId=WO2014031487&_cid=P11-MAJOJ5-33000-1
PATENT
US20140057924


SCHEME

///////////////Dasminapant, APG-1387, SM-1387, E53VN70K2X, INN 12430, APG 1387, UNII-E53VN70K2X, APG-1387 (SMAC MIMETIC), SMAC-mimetic APG-1387, IAP Inhibitor APG-1387, SM 1387
Crisugabalin



Crisugabalin
Cas 2209104-84-5
2-[(1S,2S,3R,6S,8S)-2-(aminomethyl)-2-tricyclo[4.2.1.03,8]nonanyl]acetic acid
WeightAverage: 209.289
Monoisotopic: 209.141578856
Chemical FormulaC12H19NO2
- HSK 16149
- HSK-16149
- HSK16149
- Q3MK7E8686
- PHASE 2
Tricyclo[4.2.1.03,8]nonane-2-acetic acid, 2-(aminomethyl)-, (1S,2S,3R,6S,8S)-
(1S,2S,3R,6S,8S)-2-(Aminomethyl)tricyclo[4.2.1.03,8]nonane-2-acetic acid
- (1S,2S,3R,6S,8S)-2-(Aminomethyl)tricyclo[4.2.1.03,8]nonane-2-acetic acid
- 2-[(1S,2S,3R,6S,8S)-2-(aminomethyl)-2-tricyclo[4.2.1.03,8]nonanyl]acetic acid
- Tricyclo[4.2.1.03,8]nonane-2-acetic acid, 2-(aminomethyl)-, (1S,2S,3R,6S,8S)-
Crisugabalin (HSK16149) is a selective GABA analog in development for the treatment of chronic pain. It has a wider therapeutic index than pregabalin, which has a similar mechanism of action. In China, it was approved in May 2024 for the treatment of diabetic peripheral neuropathic pain[1] and approved in July 2024 for the treatment of postherpetic neuralgia.[2] In the United States, it is in Phase III trials as of 2023.[3][4] The drug can be administered with or without food.[5]
Crisugabalin is under investigation in clinical trial NCT06490484 (Efficacy and Safety of HSK16149 Capsule in Chinese Patients With Diabetic Peripheral Neuropathic Pain Who Had an Inadequate Response to Pregabalin).
SCHEME

PATENTS
WO2020029762
https://patentscope.wipo.int/search/en/detail.jsf?docId=WO2020029762&_cid=P10-MAI1TM-34428-1


[0414]2-((1S,2S,3R,6S,8S)-2-(aminomethyl)tricyclo[4.2.1.0
3,8 ]nonanyl-2-yl)acetate benzenesulfonate (1:1) (Compound 1)
[0415]
2-((1S,2S,3R,6S,8S)-2-(aminomethyl)tricyclo[4.2.1.0 3,8]nonan-2-yl)acetic acid compound with benzenesulfonic acid(1:1)
[0416]
[0417]
[0418]Step 1: 3-(Cyclohexyl-3-en-1-yl)propanoic acid (1B)
[0419]
3-(cyclohex-3-en-1-yl)propanoic acid
[0420]
[0421]Anhydrous formic acid (18.82kg, 409.09mol) was pumped into a 100-liter reactor. The temperature was lowered to 10°C. Triethylamine (16.53kg, 163.64mol) was added dropwise to the reaction solution. After addition, it was stirred for 20 minutes. When the internal temperature was 10°C, cycloisopropyl malonate (7.86kg, 54.55mol) was added to the reactor. Then 3-cyclohexene-1-carboxaldehyde (6.00kg, 54.55mol) was added dropwise to the reaction solution at an internal temperature of 40°C. After addition, the temperature was raised to 140-150°C and the reaction was continued until no gas was released. The pH of the reaction solution was adjusted to 1-2 with 6N hydrochloric acid (24.0L). The aqueous phase was extracted with dichloromethane (12L×2), and the organic phases were combined and washed with saturated brine (10L×2). The organic phase was dried over anhydrous sodium sulfate (2.0 kg) for 1 hour, filtered, and the filtrate was concentrated and evaporated to dryness to obtain a yellow oil 1B (8.80 kg).
[0422]
1H NMR(400MHz,CDCl 3)δ10.23(s,1H),5.73–5.55(m,2H),2.46–2.30(m,2H),2.09–1.96(m,2H),1.81–1.53(m,6H),1.35–1.17(m,1H)。
[0423]
[0424]Step 2: 3-(Cyclohexyl-3-en-1-yl)-1-(pyrrolidin-1-yl)propyl-1-one (1C)
[0425]
3-(cyclohex-3-en-1-yl)-1-(pyrrolidin-1-yl)propan-1-one
[0426]
[0427]Dissolve 1B (11.20kg, 72.727mol) in dichloromethane (60.0L) and pump into a 100L reactor. Add DMF (3.0mL) and drop oxalyl chloride (9.046kg, 71.272mol) into the reaction solution. After addition, stir at room temperature for 2.0 hours. Add tetrahydropyrrole (5.689kg, 79.999mol) and triethylamine (8.814kg, 87.272mol) dropwise into the reactor. Control the internal temperature below 10℃, after addition, stir at room temperature overnight. Cool the reaction solution to 10℃. Add 3N hydrochloric acid (20.0L) dropwise to adjust the pH of the reaction solution to between 1-2. Let stand, separate the liquids, and extract the aqueous phase with dichloromethane (10.0L×1). The organic phases were combined and washed with 5% sodium hydroxide solution (10.0 L x 1) and saturated ammonium chloride solution (20.0 L x 1) in sequence. The organic phase was dried over anhydrous sodium sulfate (2.0 kg) for 30 minutes, filtered, and the filtrate was concentrated to obtain brown liquid 1C (15.00 kg, yield 99.6%).
[0428]
1H NMR(400MHz,CDCl 3)δ5.73–5.56(m,2H),3.43(dd,4H),2.37–2.22(m,2H),2.16–2.01(m,4H),1.90(dt,4H),1.81–1.51(m,6H),1.30–1.15(m,2H)。
[0429]
[0430]Step 3: Tricyclo[4.2.1.0
3,8 ]nonanyl-2-one (1R,3S,6R,8R and 1S,3R,6S,8S racemate) (1D)
[0431]
tricyclo[4.2.1.0 3,8]nonan-2-one(1R,3S,6R,8R and 1S,3R,6S,8S racemate)
[0432]
[0433]Dissolve 1C (5.64kg, 27.22mol) in dichloromethane (40.0L) and pump it into a 100L reactor. Cool to -10°C and add 2,4,6-trimethylpyridine (4.94kg, 40.83mol). Add a dichloromethane solution (16.0L) of trifluoromethanesulfonic anhydride (11.50kg, 40.83mol) dropwise to the reaction solution until complete. Heat and reflux for 12 hours. After the reaction is complete as detected by the central control, add an aqueous solution (23.0L) of sodium hydroxide (3.10kg, 77.5mol) dropwise to the reaction solution and adjust the pH of the reaction solution to between 10-11. Continue to reflux for 5-6 hours. Stand and separate the liquids, extract the aqueous phase with dichloromethane (5.0L×1), and combine the organic phases. Pump the organic phase into the reactor and cool to 10°C. 2.0N hydrochloric acid solution (20.0L) was added dropwise to adjust the pH of the reaction solution to between 1 and 2. The solution was separated by standing, and the organic phase was washed with saturated brine (20L×1), concentrated, and the residue was dissolved with acetone (20.0L), then pumped into a 100L reactor and stirred, and a solution of concentrated sulfuric acid (4.0L) and water (20.0L) was added dropwise, and refluxed for 2 hours after addition. The temperature was lowered to 15°C, saturated brine (20.0L) was added to the reaction solution, and extracted with n-hexane (15.0L×2). The organic phases were combined, washed with saturated brine (20.0L×1), and the organic phase was dried over anhydrous sodium sulfate overnight. After filtration, the filtrate was concentrated under reduced pressure to obtain a yellow solid crude product 1D (3.00kg, yield 81%) with a purity of 50%.
[0434]1D Further purification steps:
[0435]Method 1: Anhydrous sodium bisulfite (5.735 kg, 55.147 mol) was dissolved in 66 L of purified water and added to a 100 L reactor. A solution of crude 1D (3.00 kg, 22.059 mol) in ethanol (3.0 L) was added under stirring at room temperature. The mixture was stirred overnight at room temperature and extracted with ethyl acetate (20 L × 2). The aqueous phase was added to the reactor, stirred and cooled to 10°C. A solution of sodium hydroxide (2.250 kg, 56.250 mol) in water (10 L) was added dropwise. The pH was adjusted to 10-12. The mixture was stirred at room temperature for 2 hours. The mixture was extracted with n-hexane (20 L × 2). The organic phases were combined and washed with purified water (20 L × 1). The organic phases were dried with anhydrous sodium sulfate (2 kg) for 1 hour, filtered, and the filtrate was evaporated to dryness to obtain 1D as a colorless crystalline solid (2.7 kg, yield 90%) with a purity of 98.3%.
[0436]Method 2: Sodium bisulfite (1529g, 14.706mol) was dissolved in 22L water, and a solution of 1D crude product (1000g, 7.353mol) in anhydrous ethanol (1000mL) was added dropwise under stirring, and stirred overnight at room temperature (24 hours). The reaction solution was extracted with dichloromethane (5L×2) to remove impurities, and sulfuric acid solution (prepared with 6.4L concentrated sulfuric acid and 6kg crushed ice) was added dropwise to the aqueous phase, and stirred at room temperature for 5 hours. The reaction solution was extracted with n-hexane (extracted 3-4 times, 4L each time), the organic phases were combined and washed with saturated sodium chloride aqueous solution (5L×2), the organic phases were dried with 1kg anhydrous sodium sulfate for 2 hours, filtered, and the filtrate was evaporated to dryness to obtain 1D, a white solid (900g, yield: 90%), and the purity was determined to be 98.1%.
[0437]
1H NMR(400MHz,CDCl 3)δ3.39(m,1H),3.19(m,1H),2.77(m,1H),2.38(m,1H),2.05(m,1H),1.93(d,1H),1.77(m,1H),1.45(m,4H),1.20(m,1H)。
[0438]
[0439]Step 4: tert-Butyl 2-(tricyclo[4.2.1.0
3,8 ]nonanyl-2-ylidene) acetate (1R,3S,6R,8R and 1S,3R,6S,8S racemate) (1E)
[0440]
tert-butyl 2-tricyclo[4.2.1.0 3,8]nonan-2-ylidene)acetate(1R,3S,6R,8R and 1S,3R,6S,8S racemate)
[0441]
[0442]Potassium tert-butoxide (742.0g, 6.62mol) and tetrahydrofuran (6.20L) were added to a 20L reactor. The temperature was lowered to 5°C, and tert-butyl dimethoxyphosphonoacetate (1480g, 6.62mol, 1.1eq) was added dropwise to the reaction solution. The reaction temperature was controlled at 10°C-15°C, and stirring was continued for 1 hour. Then, a solution of 1D (820.0g, 6.02mol, 1.0eq) in tetrahydrofuran (2.0L) was added dropwise to the reaction solution. The addition was completed within 1 hour, and the temperature was naturally raised to room temperature for reaction for 2 hours. Saturated ammonium chloride solution (2.0L) and purified water (2.0L) were added to the reactor in sequence. After stirring for 20 minutes, the mixture was allowed to stand for stratification, and the aqueous phase was extracted with methyl tert-butyl ether (1.5L×2). The organic phases were combined, washed with saturated brine (2L×2), and dried over anhydrous sodium sulfate. Filtration and concentration afforded 1E as a yellow liquid (1.50 kg).
[0443]
[0444]Step 5: tert-Butyl 2-(2-(nitromethyl)tricyclo[4.2.1.0
3,8 ]nonanyl-2-yl)acetate (1R,2R,3S,6R,8R and 1S,2S,3R,6S,8S racemate) (1F)
[0445]
tert-butyl 2-(2-(nitromethyl)tricyclo[4.2.1.03,8]nonan-2-yl)acetate(1R,2R,3S,6R,8R and 1S,2S,3R,6S,8S racemate)
[0446]
[0447]1E (1.40 kg, 5.97 mol, 1.0 eq), nitromethane (1.82 kg, 29.85 mol, 5.0 eq) and dimethyl sulfoxide (9.8 L) were added to a 20 L reactor in sequence. Stir and add cesium carbonate (2.34 kg, 7.16 mol, 1.2 eq) to the reaction solution. After the addition, heat to 80°C-85°C, continue to keep the reaction for 5 hours, then cool to room temperature, add purified water (20.0 L) to the reactor, and extract the aqueous phase with methyl tert-butyl ether (8.0 L × 3). Combine the organic phases, wash with saturated brine (8.0 L × 2), and dry over anhydrous sodium sulfate. Filter and concentrate to obtain a brown liquid 1F (1.62 kg, yield: 92%).
[0448]
[0449]Step 6: tert-Butyl 2-((1S,2S,3R,6S,8S)-2-(aminomethyl)tricyclo[4.2.1.0
3,8 ]nonanyl-2-yl)acetate (S)-2-acetoxy-2-phenylacetic acid (1H)
[0450]
tert-butyl2-((1S,2S,3R,6S,8S)-2-(aminomethyl)tricyclo[4.2.1.03,8]nonan-2-yl)acetate(S)-2-acetoxy-2-phenylacetate
[0451]
[0452]Add 1F (730.0 g, 2.47 mol) and methanol (7.3 L) to a 50 L reactor. Stir, add nickel chloride hexahydrate (118 g, 0.49 mol, 0.2 eq) to the reaction, cool the reaction solution to 5 ° C, add sodium borohydride (374 g, 9.88 mol, 4.0 eq) in batches, keep the reaction system temperature at 20 ° C-30 ° C, and add it in about 3 hours. After the addition, continue to stir and react for 2 hours. Add ice water (16.4 L) to the reactor, and filter the aqueous phase with diatomaceous earth. Extract the filtrate with dichloromethane (3.0 L × 2) and combine the organic phases, wash with saturated brine (4 L × 1), and dry over anhydrous sodium sulfate. Filter, add (S)-(+)-O-acetyl-L-mandelic acid (384 g, 1.97 mol, 0.8 eq) to the filtrate, and stir for 20 minutes after the addition. The organic phase was concentrated by distillation until no solvent was evaporated, and then stirred with isopropanol (5.9 L) for 2 hours, cooled to 5°C and stirred for 1 hour. Filtered, the filter cake was washed with isopropanol (0.4 L × 1), and dried to obtain a white solid product 1H crude product (422 g, yield: 34.96%). The solid was taken and the ee value was determined to be 48.35% after derivatization.
[0453]First crystallization: Add crude product 1H (420.0 g, 0.92 mol), isopropanol (4.20 L) and water (0.21 L) to the reactor in sequence. Raise the temperature to 82 °C to completely dissolve the solid and keep warm for 0.5 hours. Cool down to 20 °C for crystallization for about 6 hours. When the internal temperature reaches 20 °C, filter and wash the filter cake with isopropanol (0.40 L × 1). Combine the solids and dry them at 60-65 °C for 4 hours to constant weight. Obtain the first crystal of 1H (260 g, yield: 62%). After taking the solid for derivatization, the ee value is 81.25%.
[0454]Second crystallization: Add the first crystal of 1H (177g, 0.39mol), isopropanol (2.53L) and water (0.126L) to the reactor in sequence. Raise the temperature to 82℃ to completely dissolve the solid and keep warm for 0.5 hours. Cool down to 20℃ for crystallization for about 4.5 hours. When the internal temperature reaches 30℃, filter and wash the filter cake with isopropanol (0.10L×1). Combine the solids and dry them at 60-65℃ for 4 hours to constant weight. Obtain pure white solid 1H (128g, yield: 72%). After taking the solid derivative, the ee value is determined to be 99.73%.
[0455]
[0456]Step 7: 2-((1S,2S,3R,6S,8S)-2-(aminomethyl)tricyclo[4.2.1.0
3,8 ]nonanyl-2-yl)acetic acid benzenesulfonic acid compound (1:1) (Compound 1)
[0457]
2-((1S,2S,3R,6S,8S)-2-(aminomethyl)tricyclo[4.2.1.0 3,8]nonan-2-yl)acetic acid compound with benzenesulfonic acid(1:1)
[0458]
[0459]Add 1H pure product (100.0g, 0.218mol) and purified water (0.8L) to the reactor in sequence and cool to 0-10℃. When the internal temperature reaches 0-10℃, add 1mol/L NaOH (218mL) aqueous solution to the reactor and adjust the pH of the reaction solution to 9-10. Let stand for stratification and extract the aqueous phase with dichloromethane (0.30L×2). Combine the organic phases and wash with 1mol/L NaOH (0.10L×1) solution and saturated brine (0.15L×1) in sequence. Add activated carbon (5.0g) to the organic phase for decolorization and dry with anhydrous sodium sulfate. Filter, concentrate the filtrate, and dissolve the residue in the concentration kettle with acetonitrile (280mL). Prepare a solution of benzenesulfonic acid monohydrate (77.0g, 0.437mol) with purified water (280mL) and add it dropwise to the above acetonitrile solution until complete. The temperature was raised to 80-85°C and kept for 4-6 hours. The reaction solution was cooled to 10-20°C for crystallization for about 4-6 hours. When the internal temperature reached 10-20°C, the solution was filtered and the filter cake was washed with water (30 mL × 1) and acetonitrile (50 mL × 1) in turn. After drying, compound 1 was obtained as a white solid (72 g, yield: 90%).
[0460]
1H NMR(400MHz,MeOD)δ7.83(m,2H),7.42(m,3H),3.31(dt,4H),2.86(m,1H),2.55(d,2H),2.48(ddd,1H),2.32(dd,1H),2.15(m,1H),2.04(m,1H),1.77(m,1H),1.62(m,4H),1.45(m,1H),1.28(dt,1H)。
[0461]
LCMS m/z=210.1[M+1]。
References
^ “Monthly Report: New Drug Approval in China, May 2024”.
- ^ “海思科苯磺酸克利加巴林胶囊获批新适应症”. PhIRDA. 19 July 2024. Retrieved 26 April 2025.
- ^ Gou, Xiaoli; Yu, Xiaojuan; Bai, Dongdong; Tan, Bowei; Cao, Pingfeng; Qian, Meilin; Zheng, Xiaoxiao; Chen, Lei; Shi, Zongjun; Li, Yao; Ye, Fei; Liang, Yong; Ni, Jia (March 2021). “Pharmacology and Mechanism of Action of HSK16149, a Selective Ligand of α2δ Subunit of Voltage-Gated Calcium Channel with Analgesic Activity in Animal Models of Chronic Pain”. The Journal of Pharmacology and Experimental Therapeutics. 376 (3): 330–337. doi:10.1124/jpet.120.000315. ISSN 1521-0103. PMID 33293377.
- ^ Guo, Xiaohui; Zhang, Tingting; Yuan, Geheng; Yukun, LI; Hua Ma, Jian; Hong-Mei, LI (2023). “224-OR: The Efficacy and Safety of HSK 16149 in Chinese with Diabetic Peripheral Neuropathic Pain—A Randomized, Double-Blinded, Placebo and Pregabalin-Controlled Phase II/III Study”. Diabetes. 72. doi:10.2337/db23-224-OR.
- ^ Wu, Qingqing; Zhu, Huijuan; Song, Rong; Zhang, Mengqi; Li, Fangqiong; Zeng, Weifang; Wang, Wei; Jia, Jingying; Yu, Chen; Liu, Yanmei (June 2023). “Effect of a high-fat and high-calorie food on the pharmacokinetics of a novel, potent GABA analog HSK16149 in healthy subjects”. Pharmacology Research & Perspectives. 11 (3): e01102. doi:10.1002/prp2.1102. PMC 10199234. PMID 37208866.
| Legal status | |
|---|---|
| Legal status | Investigational |
| Identifiers | |
| CAS Number | 2209104-84-5 |
| UNII | Q3MK7E8686 |
| Chemical and physical data | |
| Formula | C12H19NO2 |
| Molar mass | 209.289 g·mol−1 |
//////////Crisugabalin, HSK 16149, HSK-16149, HSK16149, Q3MK7E8686, PHASE 2
Elacestrant



Elacestrant
(6R)-6-[2-[ethyl-[[4-[2-(ethylamino)ethyl]phenyl]methyl]amino]-4-methoxyphenyl]-5,6,7,8-tetrahydronaphthalen-2-ol
(6R)-6-{2-[ethyl({4-[2-(ethylamino)ethyl]phenyl}methyl)amino]-4-methoxyphenyl}-5,6,7,8-tetrahydronaphthalen-2-ol
FDA 1/27/2023, Orserdu
WeightAverage: 458.646
Monoisotopic: 458.293328472
Chemical FormulaC30H38N2O2
To treat estrogen receptor-positive, human epidermal growth factor receptor 2-negative, ESR1-mutated, advanced or metastatic breast cancer with disease progression following at least one line of endocrine therapy
Drug Trials Snapshot
- CAS 722533-56-4
- RAD-1901
- ER-306323
- FM6A2627A8
- WHO 10247
Elacestrant, sold under the brand name Orserdu, is a selective estrogen receptor degrader (SERD) used in the treatment of breast cancer.[1][4] It is taken by mouth.[1][4]
Elacestrant is an antiestrogen that acts as an antagonist of estrogen receptors, which are the biological targets of endogenous estrogens like estradiol.[1] The most common side effects of elacestrant include body pain, nausea and vomiting, increased serum lipids, elevated liver enzymes, fatigue, decreased hemoglobin, raised creatinine, decreased appetite, diarrhea, headache, constipation, abdominal pain, and hot flashes.[2]
Elacestrant was approved for medical use in the United States in January 2023,[1][2][5][6] and in the European Union in September 2023.[3][7]
PATENTS
Cruskie MP, et al. (2019). Polymorphic forms of RAD1901-2HCl (U.S. Patent No. 10,385,008 B2). U.S. Patent and Trademark Office. https://patentimages.storage.googleapis.com/42/82/b6/e9fcbbbd08054e/US10385008.pdf
| Patent Number | Pediatric Extension | Approved | Expires (estimated) | |
|---|---|---|---|---|
| US10071066 | No | 2018-09-11 | 2034-10-10 | |
| US10385008 | No | 2019-08-20 | 2038-01-05 | |
| US10420734 | No | 2019-09-24 | 2034-10-10 | |
| US10745343 | No | 2020-08-18 | 2038-01-05 | |
| US11779552 | No | 2023-10-10 | 2034-10-10 | |
| US11819480 | No | 2023-11-21 | 2036-11-29 | |
| US7612114 | No | 2009-11-03 | 2026-08-18 | |
| US8399520 | No | 2013-03-19 | 2023-12-25 |

PATENT
https://patents.google.com/patent/US10385008B2/en
Medical uses
Elacestrant is indicated for the treatment of postmenopausal women or adult men with estrogen receptor (ER)-positive, human epidermal growth factor receptor 2 (HER2)-negative, ESR1–mutated, advanced or metastatic breast cancer with disease progression following at least one other line of endocrine therapy.[2][4]
Pharmacology
Pharmacodynamics
Elacestrant is an antiestrogen that acts as an antagonist of estrogen receptors, specifically targeting the estrogen receptor alpha (ERα), which is the biological target of endogenous estrogens like estradiol.[1] Additionally, elacestrant is a selective estrogen receptor degrader (SERD), meaning it induces the degradation of ERα.[1][8]
Pharmacokinetics
Elacestrant has an oral bioavailability of approximately 10%.[1] Its plasma protein binding exceeds 99% and remains independent of concentration.[1] Elacestrant is metabolized in the liver, primarily by the cytochrome P450 enzyme CYP3A4 and to a lesser extent by CYP2A6 and CYP2C9.[1] The elimination half-life of elacestrant is 30 to 50 hours.[1] It is excreted primarily in feces (82%) and to a lesser extent in urine (7.5%).[1]
History
The efficacy of elacestrant was evaluated in the EMERALD trial, which was a randomized, open-label, active-controlled, multicenter study involving 478 postmenopausal women and men with ER-positive, HER2-negative advanced or metastatic breast cancer. Among them, 228 participants had ESR1 mutations. Eligible participants had experienced disease progression on one or two prior lines of endocrine therapy, including one line with a CDK4/6 inhibitor, and could have received up to one prior line of chemotherapy in the advanced or metastatic setting.[2]
Participants were randomly assigned in a 1:1 ratio to receive either elacestrant 345 mg orally once daily or investigator’s choice of endocrine therapy. The choices for the control arm included fulvestrant, or an aromatase inhibitor. Randomization was stratified based on whether the ESR1 mutation was detected or not, prior treatment with fulvestrant, and presence of visceral metastasis.[2]
The FDA granted the application for elacestrant priority review and fast track designations.[2]
Research
It is a nonsteroidal combined selective estrogen receptor modulator (SERM) and selective estrogen receptor degrader (SERD) (described as a “SERM/SERD hybrid (SSH)”) that was discovered by Eisai and is under development by Radius Health and Takeda for the treatment estrogen receptor (ER)-positive advanced breast cancer.[9] Elacestrant has dose-dependent, tissue-selective estrogenic and antiestrogenic activities, with biphasic weak partial agonist activity at the ER at low doses and antagonist activity at higher doses.[10] It shows agonistic activity on bone and antagonistic activity on breast and uterine tissues.[11] Unlike the SERD fulvestrant, elacestrant is able to readily cross the blood-brain-barrier into the central nervous system, where it can target breast cancer metastases in the brain,[10][11] and is orally bioavailable and does not require intramuscular injection.[10][11]
References
- ^ Jump up to:a b c d e f g h i j k l m n o p q “Orserdu- elacestrant tablet, film coated”. DailyMed. 8 February 2023. Archived from the original on 11 February 2023. Retrieved 11 February 2023.
- ^ Jump up to:a b c d e f g “FDA approves elacestrant for ER-positive, HER2-negative, ESR1-mutated advanced or metastatic breast cancer”. U.S. Food and Drug Administration (FDA). 27 January 2023. Archived from the original on 2 February 2023. Retrieved 1 February 2023.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain. - ^ Jump up to:a b “Orserdu Product information”. Union Register of medicinal products. 18 September 2023. Retrieved 1 October 2023.
- ^ Jump up to:a b c d “Orserdu EPAR”. European Medicines Agency (EMA). 9 October 2023. Retrieved 9 October 2023.
- ^ https://www.accessdata.fda.gov/drugsatfda_docs/appletter/2023/217639Orig1s000ltr.pdf Archived 2023-02-02 at the Wayback Machine
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain. - ^ “Stemline Therapeutics Inc., a wholly owned subsidiary of Menarini Group, Receives Approval from U.S. FDA for Orserdu (elacestrant) as the First and Only Treatment Specifically Indicated for Patients with ESR1 Mutations in ER+, HER2- Advanced or Metastatic Breast Cancer”. Radius (Press release). 31 January 2023. Archived from the original on 2 February 2023. Retrieved 1 February 2023.
- ^ “EC approves Menarini Group’s Orserdu for advanced or metastatic breast cancer”. PMLive. 21 September 2023. Retrieved 22 September 2023.
- ^ Lloyd MR, Wander SA, Hamilton E, Razavi P, Bardia A (2022). “Next-generation selective estrogen receptor degraders and other novel endocrine therapies for management of metastatic hormone receptor-positive breast cancer: current and emerging role”. Therapeutic Advances in Medical Oncology. 14: 17588359221113694. doi:10.1177/17588359221113694. PMC 9340905. PMID 35923930.
- ^ Clinical trial number NCT03778931 for “Phase 3 Trial of Elacestrant vs. Standard of Care for the Treatment of Patients With ER+/HER2- Advanced Breast Cancer” at ClinicalTrials.gov
- ^ Jump up to:a b c Wardell SE, Nelson ER, Chao CA, Alley HM, McDonnell DP (October 2015). “Evaluation of the pharmacological activities of RAD1901, a selective estrogen receptor degrader”. Endocrine-Related Cancer. 22 (5): 713–724. doi:10.1530/ERC-15-0287. PMC 4545300. PMID 26162914.
- ^ Jump up to:a b c Garner F, Shomali M, Paquin D, Lyttle CR, Hattersley G (October 2015). “RAD1901: a novel, orally bioavailable selective estrogen receptor degrader that demonstrates antitumor activity in breast cancer xenograft models”. Anti-Cancer Drugs. 26 (9): 948–956. doi:10.1097/CAD.0000000000000271. PMC 4560273. PMID 26164151.
| Clinical data | |
|---|---|
| Pronunciation | /ˌɛləˈsɛstrənt/ EL-ə-SES-trənt |
| Trade names | Orserdu |
| Other names | RAD-1901; ER-306323 |
| License data | US DailyMed: Elacestrant |
| Routes of administration | By mouth |
| ATC code | L02BA04 (WHO) |
| Legal status | |
| Legal status | US: ℞-only[1][2]EU: Rx-only[3][4] |
| Pharmacokinetic data | |
| Bioavailability | ~10%[1] |
| Protein binding | >99%[1] |
| Metabolism | Liver (major: CYP3A4, minor: CYP2A6, CYP2C9)[1] |
| Elimination half-life | 30–50 hours[1] |
| Excretion | Feces (82%), urine (7.5%)[1] |
| Identifiers | |
| showIUPAC name | |
| CAS Number | 722533-56-4 |
| PubChem CID | 23642301 |
| DrugBank | DB06374 |
| ChemSpider | 57583807 |
| UNII | FM6A2627A8 |
| KEGG | D11671 |
| ChEMBL | ChEMBL4297509 |
| PDB ligand | I0V (PDBe, RCSB PDB) |
| CompTox Dashboard (EPA) | DTXSID901045846 |
| ECHA InfoCard | 100.312.890 |
| Chemical and physical data | |
| Formula | C30H38N2O2 |
| Molar mass | 458.646 g·mol−1 |
| 3D model (JSmol) | Interactive image |
| showSMILES | |
| showInChI | |
/////////Elacestrant, Orserdu, FDA 2023, APPROVALS 2023, FM6A2627A8, WHO 10247, ER 306323, RAD 1901, RAD1901
Clofutriben



Clofutriben
Cas 1204178-50-6
HCL 1203941-88-1
- ASP 3662
- 4-(5-(2-(4-Chloro-2,6-difluorophenoxy)propan-2-yl)-4-methyl-4H-1,2,4-triazol-3-yl)-3-fluorobenzamide
- 4-{5-[2-(4-Chloro-2,6-difluorophenoxy)propan-2-yl]-4-methyl-4H-1,2,4-triazol-3-yl}-3-fluorobenzamide
- 4-[5-[2-(4-chloro-2,6-difluorophenoxy)propan-2-yl]-4-methyl-1,2,4-triazol-3-yl]-3-fluorobenzamide
- 4L1TY1U5VC
| Molecular Weight | 424.80 |
|---|---|
| Formula | C19H16ClF3N4O2 |
Clofutriben (ASP3662) is a 11β-hydroxysteroid dehydrogenase type 1 inhibitor.
Clofutriben is an orally bioavailable selective inhibitor of the enzyme 11beta-hydroxysteroid dehydrogenase type 1 (11b-HSD1; 11bHSD1; HSD11B1; HSD1; HSD-1), with potential protective activity for disorders of corticosteroid excess. Upon oral administration, clofutriben selectively binds to and inhibits the activity of HSD-1. This prevents the conversion of cortisone to the active hormone cortisol and thereby preventing the activation of the glucocorticoid receptors (GRs). By blocking cortisol production in metabolic tissues, clofutriben may inhibit the adverse metabolic effects that are caused by exogenous administration of glucocorticoids or in disorders in which cortisol is secreted in excess. HSD-1 is highly expressed in metabolic tissues, such as liver, skeletal muscle, and adipose tissue. It plays a crucial role in regulating the production of cortisol to activate the GRs.
SCHEME

PATENTS
Clinical and Translational Science (2019), 12(3), 291-301
British Journal of Pharmacology (2018), 175(19), 3784-3796
Sparrow Pharmaceuticals, Inc. WO2020106337
WO2019075394
WO2018117063
WO2010001946
PATENT
PDT PAT FOR HCL SALT, WO2012033070
https://patentscope.wipo.int/search/en/detail.jsf?docId=WO2012033070
PATENT
PDT PAT FOR BASE, WO2018117063
PATENT
WO2010001946
[1]. Kiso T, et al. Analgesic effects of ASP3662, a novel 11尾-hydroxysteroid dehydrogenase 1 inhibitor, in rat models of neuropathic and dysfunctional pain. Br J Pharmacol. 2018 Oct;175(19):3784-3796. [Content Brief]
////////////Clofutriben, ASP 3662, orphan drug, 4L1TY1U5VC, Sparrow Pharmaceuticals,
Pirtobrutinib



Pirtobrutinib
- CAS 2101700-15-4
- JAYPIRCA
- RXC-005
- LY3527727
- LOXO-305
- WHO 11681
- WeightAverage: 479.436
- Monoisotopic: 479.158052208
- Chemical FormulaC22H21F4N5O3
5-amino-3-[4-[[(5-fluoro-2-methoxybenzoyl)amino]methyl]phenyl]-1-[(2S)-1,1,1-trifluoropropan-2-yl]pyrazole-4-carboxamide
FDA 2023, 1/27/2023, Jaypirca
To treat relapsed or refractory mantle cell lymphoma in adults who have had at least two lines of systemic therapy, including a BTK inhibitor
Drug Trials Snapshot
Pirtobrutinib, sold under the brand name Jaypirca, is an anticancer medication that is used to treat mantle cell lymphoma.[1][2][4] It inhibits B cell lymphocyte proliferation and survival by binding and inhibiting Bruton’s tyrosine kinase (BTK).[5] It is taken by mouth.[1]
The most common adverse reactions include fatigue, musculoskeletal pain, diarrhea, edema, dyspnea, pneumonia, and bruising.[4][6] The most common adverse reactions when used to treat chronic lymphocytic leukemia or small lymphocytic leukemia include fatigue, bruising, cough, musculoskeletal pain, COVID-19, diarrhea, pneumonia, abdominal pain, dyspnea, hemorrhage, edema, nausea, pyrexia, and headache.[7]
Pirtobrutinib was approved for medical use in the United States in January 2023,[4][8][9][10] and in the European Union in November 2023.[2]
PATENTS
Guisot, N. (2017). Compounds useful as kinase inhibitors (WO 2017/103611 A1). World Intellectual Property Organization. https://patentimages.storage.googleapis.com/d7/16/21/9300e49071a21a/WO2017103611A1.pdf
https://patentscope.wipo.int/search/en/detail.jsf?docId=WO2017103611&_cid=P10-MAG7OA-80884-1


[00381] Example 120: 5-amino-3-[4-[[(5-fluoro-2-methoxy-benzoyl)amino]methyl]phenyl]-1- (2,2,2-trifluoro-1 -methyl-ethyl)pyrazole-4-carboxamide
N-[(2,2,2-Trifluoro-1-methyl-ethylidene)aminolbenzamide
General procedure S, benzhydrazide (49.9 mmol) and 1,1,1- trifluoroacetone (74.9 mmol) gave, after washing, the titled compound as a white solid. UPLC-MS (ES + , Short acidic): 1.45 min, m/z 230.9 [M+H] +
-Amino-3-[4-[[(5-fluoro-2-methoxy-benzoyl)amino]methyl]phenyl]-1-(2,2,2-trifluoro-1-methyl-ethyl)pyrazole-4-carboxamide
General procedure M, N-[[4-[5-amino-4-cyano-1-(2,2,2-trifluoro-1-methyl-ethyl)pyrazol-3-yl]phenyl]methyl]-5-fluoro-2-methoxy-benzamide (0.83 mmol) gave, after purification, the titled compound (0.42 mmol) as a white solid. UPLC-MS (ES + , Short acidic): 1.55 min, m/z 480.1 [M+H] + . UPLC-MS (ES + , Long acidic): 3.57 min, m/z 480.1 [M+H] + . 1 H NMR (400 MHz, DMSO-d 6 , δ): 8.84 (t, J = 6.1 Hz, 1H), 7.52 (dd, J = 9.2, 3.3 Hz, 1H), 7.48-7.41 (m, 4H), 7.37-7.32 (m, 1H), 7.19 (dd, J = 9.1, 4.3 Hz, 1H), 6.67 (s, 2H), 5.35-5.24 (m, 1H), 4.56 (d, J = 6.0 Hz, 2H), 3.90 (s, 3H), 1.62 (d, J = 6.9 Hz, 3H).
MORE



Medical uses
In the United States, pirtobrutinib is indicated to treat relapsed or refractory mantle cell lymphoma after at least two lines of systemic therapy, including a Bruton’s tyrosine kinase (BTK) inhibitor.[1][11] In December 2023, the US Food and Drug Administration (FDA) expanded the indication for pirtobrutinib to include the treatment of adults with chronic lymphocytic leukemia or small lymphocytic leukemia.[7][12]
In the European Union, pirtobrutinib is indicated for the treatment of mantle cell lymphoma.[2]
Mechanism of action
B cells are white cells of the lymphocyte subtype that produce antibodies, but when some of them grow uncontrollably they can be a cause of cancer. A key enzyme in B cell stimulation and survival is BTK, and pirtobrutinib inhibits BTK in a way that is different from the prototypical BTK inhibitor ibrutinib by binding in a different way that avoids a genetic change (mutation at active site cysteine residue C481 in BTK) that can make some tumors less responsive to ibrutinib.[5]
History
Pirtobrutinib is manufactured by Eli Lilly and Company and was approved by the US Food and Drug Administration in January 2023, for the treatment of mantle cell lymphoma that has become refractory to other BTK inhibitors.[13]
Efficacy was evaluated in BRUIN (NCT03740529), an open-label, multicenter, single-arm trial of pirtobrutinib monotherapy that included 120 participants with mantle cell lymphoma previously treated with a Bruton’s tyrosine kinase (BTK) inhibitor.[4] Participants had a median of three prior lines of therapy, with 93% having two or more prior lines.[4] The most common prior Bruton’s tyrosine kinase inhibitors received were ibrutinib (67%), acalabrutinib (30%), and zanubrutinib (8%); 83% had discontinued their last Bruton’s tyrosine kinase inhibitor due to refractory or progressive disease.[4] The trial was conducted at 49 sites in 10 countries in the United States, Europe, Australia, and Asia.[6] The same trial was used to assess safety and efficacy.[6]
Efficacy was evaluated in BRUIN (NCT03740529], an open-label, international, single-arm, multicohort trial that included 108 participants with chronic lymphocytic leukemia or small lymphocytic lymphoma previously treated with at least two prior lines of therapy, including a Bruton’s tyrosine kinase (BTK) inhibitor and a B-cell lymphoma-2 (BCL-2) inhibitor.[7] Participants received a median of five prior lines of therapy (range: 2 to 11).[7] Seventy-seven percent of participants discontinued the last BTK inhibitor for refractory or progressive disease.[7] Pirtobrutinib was administered orally at 200 mg once daily and was continued until disease progression or unacceptable toxicity.[7]
Society and culture
Legal status
In April 2023, the Committee for Medicinal Products for Human Use (CHMP) of the European Medicines Agency (EMA) adopted a positive opinion, recommending the granting of a conditional marketing authorization for the medicinal product Jaypirca, intended for the treatment of relapsed or refractory mantle cell lymphoma (MCL).[14] The applicant for this medicinal product is Eli Lilly Nederland B.V.[14] Pirtobrutinib was approved for medical use in the European Union in November 2023.[2]
References
- ^ Jump up to:a b c d “Jaypirca- pirtobrutinib tablet, coated”. DailyMed. 27 January 2023. Archived from the original on 11 February 2023. Retrieved 11 February 2023.
- ^ Jump up to:a b c d e “Jaypirca EPAR”. European Medicines Agency (EMA). 20 November 2023. Archived from the original on 22 November 2023. Retrieved 22 November 2023.
- ^ “Jaypirca Product information”. Union Register of medicinal products. 31 October 2023. Archived from the original on 22 November 2023. Retrieved 22 November 2023.
- ^ Jump up to:a b c d e f “FDA grants accelerated approval to pirtobrutinib for relapsed or refractory mantle cell lymphoma”. FDA. 27 January 2023. Archived from the original on 28 January 2023. Retrieved 28 January 2023.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain. - ^ Jump up to:a b Aslan B, Kismali G, Iles LR, Manyam GC, Ayres ML, Chen LS, et al. (May 2022). “Pirtobrutinib inhibits wild-type and mutant Bruton’s tyrosine kinase-mediated signaling in chronic lymphocytic leukemia”. Blood Cancer Journal. 12 (5): 80. doi:10.1038/s41408-022-00675-9. PMC 9123190. PMID 35595730.
- ^ Jump up to:a b c “Drug Trials Snapshots: Jaypirca”. U.S. Food and Drug Administration (FDA). 27 January 2023. Retrieved 13 May 2024.
- ^ Jump up to:a b c d e f “FDA grants accelerated approval to pirtobrutinib for chronic lymphocytic leukemia and small lymphocytic lymphoma”. U.S. Food and Drug Administration (FDA). 1 December 2023. Archived from the original on 3 December 2023. Retrieved 3 December 2023.
 This article incorporates text from this source, which is in the public domain.
This article incorporates text from this source, which is in the public domain. - ^ “U.S. FDA Approves Jaypirca (pirtobrutinib), the First and Only Non-Covalent (Reversible) BTK Inhibitor, for Adult Patients with Relapsed or Refractory Mantle Cell Lymphoma After at Least Two Lines of Systemic Therapy, Including a BTK Inhibitor” (Press release). Eli Lilly. 27 January 2023. Archived from the original on 30 January 2023. Retrieved 31 January 2023 – via PR Newswire.
- ^ Keam SJ (April 2023). “Pirtobrutinib: First Approval”. Drugs. 83 (6): 547–553. doi:10.1007/s40265-023-01860-1. PMID 37004673. S2CID 257912433. Archived from the original on 19 November 2023. Retrieved 19 November 2023.
- ^ Telaraja D, Kasamon YL, Collazo JS, Leong R, Wang K, Li P, et al. (August 2023). “FDA Approval Summary: Pirtobrutinib for Relapsed or Refractory Mantle Cell Lymphoma”. Clinical Cancer Research. 30 (1): OF1 – OF6. doi:10.1158/1078-0432.CCR-23-1272. PMC 10841293. PMID 37624619. S2CID 265965744.
- ^ De SK (October 2023). “Pirtobrutinib: First Non-covalent Tyrosine Kinase Inhibitor for Treating Relapsed or Refractory Mantle Cell Lymphoma in Adults”. Current Medicinal Chemistry. 31. doi:10.2174/0109298673251030231004052822. PMID 37818564. S2CID 263828536.
- ^ “Jaypirca (pirtobrutinib) Now Approved by U.S. FDA for the Treatment of Adult Patients with Chronic Lymphocytic Leukemia or Small Lymphocytic Lymphoma Who Have Received at Least Two Lines of Therapy, Including a BTK Inhibitor and a BCL-2 Inhibitor” (Press release). Eli Lilly. 1 December 2023. Archived from the original on 3 December 2023. Retrieved 3 December 2023 – via PR Newswire.
- ^ “FDA approves Eli Lilly’s drug for rare blood cancer”. Reuters. 27 January 2023. Archived from the original on 28 January 2023.
- ^ Jump up to:a b “Jaypirca: Pending EC decision”. European Medicines Agency. 26 April 2023. Archived from the original on 26 April 2023. Retrieved 27 April 2023. Text was copied from this source which is copyright European Medicines Agency. Reproduction is authorized provided the source is acknowledged.
Further reading
- Mato AR, Woyach JA, Brown JR, Ghia P, Patel K, Eyre TA, et al. (July 2023). “Pirtobrutinib after a Covalent BTK Inhibitor in Chronic Lymphocytic Leukemia”. The New England Journal of Medicine. 389 (1): 33–44. doi:10.1056/NEJMoa2300696. hdl:11585/960014. PMID 37407001. S2CID 259358462.
External links
- “Pirtobrutinib”. National Cancer Institute. 16 February 2023.
- “Pirtobrutinib”. NCI Drug Dictionary.
| Clinical data | |
|---|---|
| Trade names | Jaypirca |
| Other names | LOXO-305 |
| AHFS/Drugs.com | Monograph |
| MedlinePlus | a623012 |
| License data | US DailyMed: Pirtobrutinib |
| Routes of administration | By mouth |
| Drug class | Protein kinase inhibitor |
| ATC code | L01EL05 (WHO) |
| Legal status | |
| Legal status | US: ℞-only[1]EU: Rx-only[2][3] |
| Identifiers | |
| showIUPAC name | |
| CAS Number | 2101700-15-4 |
| PubChem CID | 129269915 |
| DrugBank | DB17472 |
| ChemSpider | 114875989 |
| UNII | JNA39I7ZVB |
| KEGG | D12050 |
| ChEBI | CHEBI:229212 |
| ChEMBL | ChEMBL4650485 |
| PDB ligand | Y7W (PDBe, RCSB PDB) |
| Chemical and physical data | |
| Formula | C22H21F4N5O3 |
| Molar mass | 479.436 g·mol−1 |
| 3D model (JSmol) | Interactive image |
| showSMILES | |
| showInChI | |
- Jensen JL, Mato AR, Pena C, Roeker LE, Coombs CC: The potential of pirtobrutinib in multiple B-cell malignancies. Ther Adv Hematol. 2022 Jun 16;13:20406207221101697. doi: 10.1177/20406207221101697. eCollection 2022. [Article]
- Aslan B, Kismali G, Iles LR, Manyam GC, Ayres ML, Chen LS, Gagea M, Bertilaccio MTS, Wierda WG, Gandhi V: Pirtobrutinib inhibits wild-type and mutant Bruton’s tyrosine kinase-mediated signaling in chronic lymphocytic leukemia. Blood Cancer J. 2022 May 20;12(5):80. doi: 10.1038/s41408-022-00675-9. [Article]
- Alu A, Lei H, Han X, Wei Y, Wei X: BTK inhibitors in the treatment of hematological malignancies and inflammatory diseases: mechanisms and clinical studies. J Hematol Oncol. 2022 Oct 1;15(1):138. doi: 10.1186/s13045-022-01353-w. [Article]
- Mato AR, Shah NN, Jurczak W, Cheah CY, Pagel JM, Woyach JA, Fakhri B, Eyre TA, Lamanna N, Patel MR, Alencar A, Lech-Maranda E, Wierda WG, Coombs CC, Gerson JN, Ghia P, Le Gouill S, Lewis DJ, Sundaram S, Cohen JB, Flinn IW, Tam CS, Barve MA, Kuss B, Taylor J, Abdel-Wahab O, Schuster SJ, Palomba ML, Lewis KL, Roeker LE, Davids MS, Tan XN, Fenske TS, Wallin J, Tsai DE, Ku NC, Zhu E, Chen J, Yin M, Nair B, Ebata K, Marella N, Brown JR, Wang M: Pirtobrutinib in relapsed or refractory B-cell malignancies (BRUIN): a phase 1/2 study. Lancet. 2021 Mar 6;397(10277):892-901. doi: 10.1016/S0140-6736(21)00224-5. [Article]
- Wang E, Mi X, Thompson MC, Montoya S, Notti RQ, Afaghani J, Durham BH, Penson A, Witkowski MT, Lu SX, Bourcier J, Hogg SJ, Erickson C, Cui D, Cho H, Singer M, Totiger TM, Chaudhry S, Geyer M, Alencar A, Linley AJ, Palomba ML, Coombs CC, Park JH, Zelenetz A, Roeker L, Rosendahl M, Tsai DE, Ebata K, Brandhuber B, Hyman DM, Aifantis I, Mato A, Taylor J, Abdel-Wahab O: Mechanisms of Resistance to Noncovalent Bruton’s Tyrosine Kinase Inhibitors. N Engl J Med. 2022 Feb 24;386(8):735-743. doi: 10.1056/NEJMoa2114110. [Article]
- FDA Approved Drug Products: JAYPIRCA (pirtobrutinib) tablets for oral use [Link]
- BioSpace: U.S. FDA Approves Jaypirca (pirtobrutinib), the First and Only Non-Covalent (Reversible) BTK Inhibitor, for Adult Patients with Relapsed or Refractory Mantle Cell Lymphoma After at Least Two Lines of Systemic Therapy, Including a BTK Inhibitor [Link]
//////////////Jaypirca, FDA 2023, APPROVALS 2023, Pirtobrutinib, RXC-005, LY3527727, LOXO-305, LOXO 305, WHO 11681
Clesacostat



Clesacostat
PF 05221304, 752DF9PPPI
CAS 1370448-25-1
WeightAverage: 502.571
Monoisotopic: 502.221620082
Chemical FormulaC28H30N4O5
4-[6-methoxy-4-(7-oxo-1-propan-2-ylspiro[4,6-dihydroindazole-5,4′-piperidine]-1′-carbonyl)pyridin-2-yl]benzoic acid
- Originator Pfizer
- ClassBenzoic acids; Carboxylic acids; Ethers; Hepatoprotectants; Indazoles; Piperidines; Pyridines; Small molecules; Spiro compounds
- Mechanism of ActionAcetyl-CoA carboxylase inhibitors
- Phase IINon-alcoholic fatty liver disease; Non-alcoholic steatohepatitis
- 21 Feb 2024Pfizer completes a phase II trial in Non-alcoholic steatohepatitis (Combination therapy) in Slovakia, Japan, Bulgaria, Canada, China, Hong Kong, India, Poland, Puerto Rico, South Korea, Taiwan (PO) (NCT04321031) (EudraCT2019-004775-39)
- 26 May 2022Clesacostat – Pfizer receives Fast Track designation for Non-alcoholic steatohepatitis [PO] (Combination therapy) in USA
- 28 Apr 2022Pfizer completes a phase II trial for Non-alcoholic fatty liver disease (Combination therapy) in USA and Canada (PO) (NCT04399538)
Clesacostat is under investigation in clinical trial NCT04321031 (Metabolic Interventions to Resolve Non-alcoholic Steatohepatitis (NASH) With Fibrosis (MIRNA)).
CLESACOSTAT is a small molecule drug with a maximum clinical trial phase of II (across all indications) and has 4 investigational indications.
SCHEME
SIDECHAIN

MAIN

PATENT
WO2021171164 89%
https://patentscope.wipo.int/search/en/detail.jsf?docId=WO2021171164&_cid=P20-MAF4R3-69728-1
4-(4-(1-lsopropyl-7-oxo-1 ,4,6,7-tetrahydrospiro[indazole-5,4′-piperidine]-1′-carbonyl)-6-methoxypyridin-2-yl)benzoic acid,
A preparation of (S)- 2-(5-((3-ethoxypyridin-2-yl)oxy)pyridin-3-yl)-N-(tetrahydrofuran-3-yl)pyrimidine-5-carboxamide is presented in Example 1 of US 2018-0051012A1 , hereby incorporated herein by reference in its entireties for all purposes. A preparation of 4-(4-(1-lsopropyl-7-oxo-1 ,4,6,7-tetrahydrospiro[indazole-5,4′-piperidine]-1 ‘-carbonyl)-6-methoxypyridin-2-yl)benzoic acid is in Example 9 of US 8,859,577, hereby incorporated herein by reference in its entireties for all purposes. Preparation of [(1 R,5S,6R)-3-{2-[(2S)-2-methylazetidin-1-yl]-6-(trifluoromethyl)pyrimidin-4-yl}-3-azabicyclo[3.1 0]hex-6-yl]acetic acid (including a crystalline free acid form thereof) is described in Example 4 of U.S. Patent No. 9,809,579. Preparation of GLP-1 R agonists are described in U.S. Patent No.10,208,019.
Step 6: (S)-2-(5-((3-ethoxypyridin-2-yl)oxy)pyridin-3-yl)-N-(tetrahydrofuran-3-yl)pyrimidine-5-carboxamide (Example 1 (DGAT2i Compound))
Oxalyl chloride (13.8 ml_, 160 mmol, 1.2 equiv) and dimethylformamide (0.510 ml_, 6.65 mmol, 0.05 equiv) were added to a suspension of 2-(5-((3-ethoxypyridin-2-yl)oxy)pyridin-3-yl)pyrimidine-5-carboxylic acid (45.0 g, 133 mmol, 1.0 equiv) in dichloromethane (500 ml_). The suspension was stirred for 2 hours when a solution was achieved. The reaction mixture was concentrated to yield crude acid chloride as a red solid. A solution of (S)-tetrahydrofuran-3-amine (12.2 g, 140 mmol, 1.05 equiv) and diisopropylethylamine (51.0 ml_, 293 mmol, 2.2 equiv) in tetrahydrofuran (100 ml_) was added dropwise to a solution of the crude acid chloride in dichloromethane (200 ml_) at 0 °C. The reaction was allowed to warm to room temperature and stirred for 16 hours. Water (1 .0 L) and ethyl acetate (600 ml_) were added and the organic layer was separated, washed with saturated sodium bicarbonate, dried over magnesium sulfate, and filtered. The filtrate was treated with activated charcoal (20 g) was stirred at 65 °C for 20 minutes. The suspension was filtered warm and filtrate was concentrated to a pale, yellow solid which was recrystallized from methanol in ethyl acetate (1 :4, 1 L) to yield (S)-2-(5-((3-ethoxypyridin-2-yl)oxy)pyridin-3-yl)-A/-(tetrahydrofuran-3-yl)pyrimidine-5-carboxamide (43.5 g, 81%) as a colorless solid. The title compound was combined with previous batches (108.7 g, 266.8 mmol) prepared in the same manner and slurried with ethyl acetate (1.0 L) at 80 °C for 4 hours. The suspension was allowed to cool to room temperature and stirred for 4 days. The solid was filtered, washed with ethyl acetate (3×200 ml_) and dried under high vacuum at 50 °C for 24 hours to yield (S)-2-(5-((3-ethoxypyridin-2-yl)oxy)pyridin-3-yl)-A/-(tetrahydrofuran-3-yl)pyrimidine-5-carboxamide (100.5 g, 92%) as a colorless solid. 1H NMR (300 MHz, DMSO-d6) 6 1.38 (t, 3H), 1.89-1.98 (m, 1H), 2.15-2.26 (m, 1H), 3.65 (dd, 1H), 3.70-3.78 (m, 1H), 3.85-3.92 (m, 2H), 4.18 (q, 2H), 4.46-4.55 (m, 1H), 7.18 (dd, 1H), 7.58 (dd, 1H), 7.69 (dd, 1H), 8.37 (dd,
1 H), 8.64 (d, 1 H), 8.95 (d, 1 H), 9.28 (s, 2H), 9.39 (d, 1 H). MS (ES+) 408.4 (M+H). Melting point 177.5 °C. Elemental analysis for C21H21N5O4: calculated C, 61.91 ; H, 5.20; N, 17.19; found C, 61.86; H, 5.18; N, 17.30.
PATENT
WO2021171163 65%
WO2020234726 65%
Journal of Medicinal Chemistry (2020), 63(19), 10879-10896
WO2020044266 89%
WO2019102311 89%
//////////Clesacostat, PF 05221304, PHASE 2, 752DF9PPPI
Civorebrutinib


Civorebrutinib
WS-413, 933NK55FMX
5-amino-3-[4-(5-chloropyridin-2-yl)oxyphenyl]-1-[(6R)-4-cyano-4-azaspiro[2.5]octan-6-yl]pyrazole-4-carboxamide
| Molecular Weight | 463.92 |
|---|---|
| Formula | C23H22ClN7O2 |
| CAS No. | 2155853-43-1 |
Civorebrutinib (WS-413) is a Bruton’s tyrosine kinase inhibitor with antineoplastic effect.
Scheme


Patent
Zhejiang Yukon Pharma Co., Ltd. WO2017198050
WO2019091440
WO2019091438
PATENT
WO2019091441
https://patentscope.wipo.int/search/en/detail.jsf?docId=WO2019091441&_cid=P10-MADPL7-76599-1
[0116]Preparation of (R)-5-amino-3-(4-((5-chloropyridin-2-yl)oxy)phenyl)-1-(4-cyano-4-azaspiro[2.5]octan-6-yl)-1H-pyrazole-4-carboxamide (Compound 1)
[0119]
[0120]DIPEA (185 g, 1.44 mol, 250 mL, 3 eq) was added to a solution of intermediate compound 11 (167 g, 479 mmol, 1 eq) in EtOH (1670 mL) at 0 ° C. Intermediate compound 17 (187 g, 575 mmol, 1.2 eq) was added to the mixture. The mixture was then stirred at 25 ° C for 12 h under a N2 atmosphere. LCMS (ET14245-55-P1A2, product: RT = 1.723 min) showed that the reaction was complete. The reaction was filtered to obtain the product. The product was used directly in the next step without purification. Intermediate compound 18 (243 g, 407 mmol, yield 85%, purity 93.1%) was obtained as a white solid.
[0122]
[0123]Intermediate compound 18 (121 g, 218 mmol, 1 eq) was stirred in H
2 SO
4 (1200 mL) at 30° C. for 36 h. TLC (DCM: MeOH=10:1, Rf=0.9) showed that compound 18 was completely consumed and only one desired spot was formed (DCM: MeOH=10:1, Rf=0.2). Multiple batches of reaction mixtures were combined, and the combined mixture was poured into MTBE (20 L), solids were precipitated and the filtrate was collected by suction filtration. The pH of the filtrate was adjusted to 10 with aqueous ammonia, extracted with EtOAc (2 L x 10), dried with Na
2 SO
4 , filtered and concentrated under reduced pressure to give intermediate compound 19 (crude product 311 g, equivalent to 238 g product) as a yellow solid.
[0125]
[0126]To a solution of intermediate compound 19 (199 g, 453 mmol, 1 eq) in DMF (1400 mL) was added cesium carbonate (295 g, 907 mmol, 2 eq) and stirred at 15 ° C for 0.5 hours. Then BrCN (52.8 g, 499 mmol, 36.7 mL, 1.1 eq) was added and stirred at 15 ° C for 2 hours. TLC (DCM: MeOH = 10: 1, R
f = 0.2) showed that compound 19 was completely reacted and only one desired spot was generated (DCM: MeOH = 10: 1, R
f = 0.6). Multiple batches of reaction mixtures were combined and the resulting mixture was filtered to remove cesium carbonate. The filtrate was then concentrated under reduced pressure to remove DMF. The residue was diluted with water (2 L) and extracted with ethyl acetate (1 L × 4). The organic phases were combined and washed with water (2 L × 2) and brine (2 L), dried over sodium sulfate, filtered and concentrated under reduced pressure. Acetonitrile (1 L) was added to the residue to precipitate a white solid, which was filtered and the filter cake was washed with acetonitrile (200 mL×2) to give Compound 1 (140 g, 302 mmol, yield 55%, purity 97.0%).
[0127]
1H NMR:CDCl 3400MHzδ8.05(d,J=2.4Hz,1H),7.60(dd,J=2.4,8.8Hz,1H),7.51(d,J=8.8Hz,2H),7.15(d,J=8.8Hz,2H),6.86(d,J=8.8Hz,1H),5.60(s,2H),5.23(br.s.,2H),4.22-4.16(m,1H),3.59-3.41(m,2H),2.39-2.24(m,2H),2.12-2.09(m,1H),1.23-1.10(m,2H),0.80-0.74(m,2H),0.62-0.61(m,1H).
////////Civorebrutinib, WS-413, WS 413, 933NK55FMX
Cinsebrutinib



Cinsebrutinib
CAS 2724962-58-5
2-fluoro-1-[(3S)-1-prop-2-enoylpiperidin-3-yl]-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide
- 2-fluoro-1-[(3S)-1-(prop-2-enoyl)piperidin-3-yl]-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide
- 2-fluoro-1-[(3S)-1-prop-2-enoylpiperidin-3-yl]-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide
| Molecular Weight | 383.46 |
|---|---|
| Formula | C22H26FN3O2 |
CINSEBRUTINIB is a small molecule drug with a maximum clinical trial phase of II and has 1 investigational indication.
Cinsebrutinib is a Bruton’s tyrosine kinase inhibitor, extracted from patent WO2021207549 (compound 5-6). Cinsebrutinib has the potential for cancer study.
SCHEME
INTERMEDIATE

MAIN

SYN
5-6 enantiomer A [WO2021207549A1]
GB005, Inc. WO2021207549
WO2021207549
https://patentscope.wipo.int/search/en/detail.jsf?docId=WO2021207549&_cid=P22-MAAYAJ-91905-1
EXAMPLES 5-5, 5-6, 5-7
Preparation of rac-1-(1-acryloylpiperidin-3-yl)-2-fluoro-5,6,7,8,9,10-hexahydrocyclo- hepta[b]indole-4-carboxamide (Compound 5-5), (S)-1-(1-acryloylpiperidin-3-yl)-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide (Compound 5-6) and (R)-1-(1-acryloylpiperidin-3-yl)-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4- carboxamide (Compound 5-7)

STEP 1: 5-bromo-4-fluoro-2-iodoaniline
To a solution of 3-bromo-4-fluoroaniline (100.0 g, 526.3 mmol) in acetic acid (500 mL) was added N-iodosuccinimide (124.3 g, 552.5 mmol) in portions at 25 °C.
The reaction mixture was stirred for 2 hours at 25 °C. The mixture was concentrated under vacuum. The residue was diluted with saturated aqueous sodium carbonate (500 mL) and extracted with ethyl acetate (500 mL x 3). The combined organic layers were washed with water (500 mL) and brine (500 mL), dried over anhydrous sodium sulfate and concentrated under vacuum. The residue was triturated with mixed solvents of ethyl acetate and petroleum ether (300 mL, 1:4, v/v) and filtered. The solid was washed with mixed solvents of ethyl acetate and petroleum ether (50 mL x 2, 1:4, v/v) and dried under reduced pressure to give 5-bromo-4-fluoro-2-iodoaniline (88.6 g, 53%) as a light blue solid.1H NMR (300 MHz, DMSO-d6) δ 7.55 (d, J = 8.1 Hz, 1H), 6.98 (d, J = 6.3 Hz, 1H), 5.27 (brs, 2H).
STEP 2: (5-bromo-4-fluoro-2-iodophenyl)hydrazine hydrochloride
To a stirred suspension of 5-bromo-4-fluoro-2-iodoaniline (88.6 g, 280.5 mmol) in concentrated hydrochloric acid (443 mL) was added dropwise a solution of sodium nitrite (23.22 g, 337.0 mmol) in water (90 mL) at 0 °C. After stirring for 1 hour at 0 °C, the resulting mixture was added dropwise to a solution of stannous chloride dihydrate (126.61 g, 561.1 mmol) in concentrated hydrochloric acid (295 mL) at 0 °C and stirred for 1 hour at this temperature. The precipitate was collected by filtration, washed with concentrated hydrochloric acid (150 mL x 5) and ethyl acetate (300 mL), dried under reduced pressure to give (5-bromo-4-fluoro-2-iodophenyl)hydrazine hydrochloride (100.3 g, crude) as a light yellow solid.1H NMR (400 MHz, DMSO-d6) δ 10.23 (brs, 3H), 7.89 (d, J = 8.0 Hz, 1H), 7.82 (brs, 1H), 7.31-7.22 (m, 1H).
STEP 3: 1-(5-bromo-4-fluoro-2-iodophenyl)-2-cycloheptylidenehydrazine To a solution of (5-bromo-4-fluoro-2-iodophenyl)hydrazine hydrochloride (80.0 g, 217.6 mmol) in methanol (400 mL) was added cycloheptanone (24.40 g, 217.6 mmol) at 20 °C. The reaction mixture was stirred for 1 hour at 20 °C. The precipitate was collected by filtration and dried under reduced pressure to give 1-(5-bromo-4-fluoro-2-iodophenyl)-2-cycloheptylidenehydrazine (72.0 g, 78%) as an off-white solid.
1H NMR (400 MHz, DMSO-d6) δ 7.77 (d, J = 8.0 Hz, 1H), 7.44 (d, J = 6.8 Hz, 1H), 7.39 (brs, 1H), 2.50-2.44 (m, 4H), 1.80-1.67 (m, 2H), 1.64-1.48 (m, 6H).
STEP 4: 1-bromo-2-fluoro-4-iodo-5,6,7,8,9,10-hexahydrocyclohepta[b]indole A mixture of 1-(5-bromo-4-fluoro-2-iodophenyl)-2-cycloheptylidenehydrazine (72.0 g, 169.4 mmol) and concentrated sulfuric acid (18 mL) in methanol (360 mL) was stirred for 16 hours at 80 °C. The methanol was removed under reduced pressure. The residue was basified with saturated aqueous sodium carbonate until pH = 10 and extracted with ethyl acetate (600 mL x 3). The combined organic layers were washed with water (500 mL x 2) and brine (500 mL), dried over anhydrous sodium sulfate and
filtered. The filtrate was concentrated under vacuum to give 1-bromo-2-fluoro-4-iodo-5,6,7,8,9,10-hexahydrocyclohepta[b]indole (43.0 g, 80% purity, 50%) as a brown solid.
1H NMR (300 MHz, DMSO-d6) δ 10.95 (s, 1H), 7.37 (d, J = 8.7 Hz, 1H), 3.23-3.15 (m, 2H), 2.94-2.85 (m, 2H), 1.89-1.76 (m, 2H), 1.72-1.58 (m, 4H).
STEP 5: 1-bromo-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4- carbonitrile
A mixture of 1-bromo-2-fluoro-4-iodo-5,6,7,8,9,10-hexahydrocyclohepta[b]indole (43.0 g, 80% purity, 84.3 mmol), zinc cyanide (4.95 g, 42.2 mmol) and tetrakis(triphenylphosphine)palladium (9.74 g, 8.4 mmol) in N,N-dimethylformamide (215 mL) was degassed and backfilled with nitrogen for three times. The reaction mixture was stirred under nitrogen at 90 °C for 2 hours. The cooled reaction mixture was diluted with water (1 L) and extracted with ethyl acetate (800 mL x 3). The combined organic layers were washed with water (500 mL x 3) and brine (800 mL), dried over anhydrous sodium sulfate, filtered and concentrated under vacuum. The residue was triturated with acetonitrile (100 mL) and filtered. The solid was washed with acetonitrile (30 mL x 2) and dried under reduced pressure to give 1-bromo-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carbonitrile (25.5 g, 94%) as a light yellow solid. ESI-MS [M-H]- calculated for (C14H12BrFN2) 305.02, 307.02, found: 304.95, 306.95.1H NMR (300 MHz, DMSO-d6) δ 11.99 (s, 1H), 7.58 (d, J = 9.0 Hz, 1H), 3.24-3.17 (m, 2H), 2.91-2.85 (m, 2H), 1.87-1.78 (m, 2H), 1.70-1.61 (m, 4H).
STEP 6: Tert-butyl 5-(4-cyano-2-fluoro-5,6,7,8,9,10- hexahydrocyclohepta[b]indol-1-yl)-3,6-dihydropyridine-1(2H)-carboxylate A mixture of 1-bromo-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carbonitrile (25.0 g, 81.4 mmol), tert-butyl 5-(4,4,5,5-tetramethyl-1,3,2-dioxaborolan-2-yl)-3,6-dihydropyridine-1(2H)-carboxylate (30.2 g, 97.7 mmol), [1,1′-bis(diphenylphosphino)ferrocene]dichloro-palladium(II) (5.96 g, 8.1 mmol) and potassium phosphate (51.8 g, 244.2 mmol) in tetrahydrofuran (125 mL) and water (31 mL) was degassed and backfilled with nitrogen for three times and stirred for 2 hours at 60 °C under nitrogen atmosphere. The cooled mixture was diluted with water (600 mL) and extracted with ethyl acetate (500 mL x 3). The combined organic layers was washed with water (500 mL x 2) and brine (500 mL), dried over anhydrous sodium sulfate, filtered and concentrated under vacuum to give tert-butyl 5-(4-cyano-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indol-1-yl)-3,6-dihydropyridine-1(2H)-carboxylate (45 g, crude) as a brown solid, which was used directly in next step without purification. ESI-MS [M+H-tBu]+ calculated for (C24H28FN3O2) 354.22, found: 354.05.
STEP 7: Tert-butyl 5-(4-carbamoyl-2-fluoro-5,6,7,8,9,10- hexahydrocyclohepta[b]indol-1-yl)-3,6-dihydropyridine-1(2H)-carboxylate To a mixture of 5-(4-cyano-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indol-1-yl)-3,6-dihydro-pyridine-1(2H)-carboxylate (45 g, crude) in ethanol (100 mL), tetrahydrofuran (100 mL) and water (100 mL) was added Parkin’s catalyst (2.0 g, 4.68 mmol). The reaction mixture was stirred for 16 hours at 90 °C. The cooled mixture was diluted with water (500 mL) and extracted with ethyl acetate (500 mL x 3). The combined organic layers were washed with water (500 mL x 2) and brine (500 mL), dried over anhydrous sodium sulfate, filtered and concentrated under vacuum. The residue was purified by column chromatography on silica gel eluting with ethyl acetate in petroleum ether (0 to 60%) to give tert-butyl 5-(4-carbamoyl-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indol-1-yl)-3,6-dihydropyridine-1(2H)-carboxylate (20.0 g, 57% over two steps) as a light yellow solid. ESI-MS [M+H]+ calculated for (C24H30FN3O3) 428.23, found: 428.15.1H NMR (400 MHz, DMSO-d6) δ 10.77 (s, 1H), 8.02 (s, 1H), 7.46-7.38 (m, 2H), 5.79 (s, 1H), 4.10-3.97 (m, 1H), 3.95-3.83 (m, 1H), 3.80-3.57 (m, 1H), 3.51-3.23 (m, 1H), 2.99-2.85 (m, 2H), 2.82-2.69 (m, 2H), 2.30-2.21 (m, 2H), 1.86-1.72 (m, 2H), 1.70-1.50 (m, 4H), 1.41 (s, 9H).
STEP 8: Tert-butyl 3-(4-carbamoyl-2-fluoro-5,6,7,8,9,10- hexahydrocyclohepta[b]indol-1-yl)piperidine-1-carboxylate
To a solution of tert-butyl 5-(4-carbamoyl-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indol-1-yl)-3,6-dihydropyridine-1(2H)-carboxylate (20 g, 46.8 mmol) in ethanol (300 mL) and tetrahydrofuran (300 mL) was added 10% Pd/C (15.0 g) under nitrogen atmosphere. The reaction mixture was degassed and backfilled with hydrogen for three times and stirred for 4 days at 50 °C under hydrogen (2 atm). The cooled mixture was filtered. The filtrate was concentrated under vacuum. The residue was recrystallized with tetrahydrofuran (100 mL) and petroleum ether (100 mL) to give tert-butyl 3-(4-carbamoyl-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indol-1-yl)piperidine-1-carboxylate (12.1 g, 60%) as an off-white solid. ESI-MS [M+H]+ calculated for (C24H32FN3O3) 430.24, found: 430.25.1H NMR (400 MHz, DMSO-d6) δ 10.75 (s, 1H), 8.00 (s, 1H), 7.46-7.35 (m, 2H), 4.17-3.86 (m, 2H), 3.55-3.43 (m, 1H), 3.31-3.10 (m, 1H), 3.08-2.63 (m, 5H), 2.14-1.96 (m, 1H), 1.93-1.60 (m, 9H), 1.39 (s, 9H).
STEP 9: 2-fluoro-1-(piperidin-3-yl)-5,6,7,8,9,10-hexahydrocyclohepta[b]indole- 4-carboxamide hydrochloride
Tert-butyl 3-(4-carbamoyl-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indol-1-yl)piperidine-1-carboxylate (12.1 g, 28.2 mmol) was dissolved in hydrogen chloride (150 mL, 4 M in 1,4-dioxane) and the solution was stirred for 2 hours at 25 °C. The mixture was concentrated under vacuum to give 2-fluoro-1-(piperidin-3-yl)-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide hydrochloride (13.4 g, crude) as a yellow solid. ESI-MS [M+H]+ calculated for (C19H24FN3O) 330.19, found: 330.10.
STEP 10: 1-(1-acryloylpiperidin-3-yl)-2-fluoro-5,6,7,8,9,10- hexahydrocyclohepta[b]indole-4-carboxamide
To a mixture of 2-fluoro-1-(piperidin-3-yl)-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide hydrochloride (13.4 g, crude) and sodium bicarbonate (23.7 g, 282.0 mmol) in tetrahydrofuran (300 mL) and water (150 mL) was added acryloyl chloride (2.81 g, 31.0 mmol) at 0 °C. After stirring for 1 hour at 0 °C, the mixture was diluted with water (500 mL) and extracted with ethyl acetate (400 mL x 3). The combined organic layers were washed with water (500 mL x 2) and brine (500 mL), dried over anhydrous sodium sulfate, filtered and concentrated under vacuum. The residue was recrystallized with tetrahydrofuran (290 mL), methanol (48 mL) and petroleum ether (330 mL) to give 1-(1-acryloylpiperidin-3-yl)-2-fluoro-
5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide (6.0 g, 56% over two steps) as a white solid. ESI-MS [M+H]+ calculated for (C22H26FN3O2) 384.20, found: 384.15.
STEP 11: (S)-1-(1-acryloylpiperidin-3-yl)-2-fluoro-5,6,7,8,9,10- hexahydrocyclohepta[b]indole-4-carboxamide and (R)-1-(1-acryloylpiperidin-3- yl)-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]-indole-4-carboxamide
1-(1-acryloylpiperidin-3-yl)-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide (6.0 g) was separated by Prep-SFC with the following conditions: Column: (R,R)-Whelk-01, 2.12 x 25 cm, 5 um; Mobile Phase A: CO2, Mobile Phase B: IPA/DCM = 5:1; Flow rate: 200 mL/min; Gradient: 50% B; 220 nm; Injection Volume: 19 mL; Number Of Runs: 29; RT1: 4.97 min to afford assumed (S)-1-(1-acryloylpiperidin-3-yl)-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide (2.55 g, 43%) as an off-white solid and RT2: 8.2 min to afford assumed (R)-1-(1-acryloylpiperidin-3-yl)-2-fluoro-5,6,7,8,9,10-hexahydrocyclohepta[b]indole-4-carboxamide (2.63 g, 44%) as an off-white solid.
Compound 5-6
ESI-MS [M+H]+ calculated for (C22H26FN3O2) 384.20, found: 384.20.1H NMR (300 MHz, DMSO-d6) δ 10.75 (s, 1H), 8.00 (s, 1H), 7.49-7.31 (m, 2H), 6.93-6.72 (m, 1H), 6.18-6.02 (m, 1H), 5.73-5.56 (m, 1H), 4.67-4.42 (m, 1H), 4.27-4.05 (m, 1H), 3.63-3.41 (m, 1.5H), 3.19-3.02 (m, 1H), 3.00-2.79 (m, 4H), 2.70-2.62 (m, 0.5H), 2.21-2.02 (m, 1H), 2.01-1.87 (m, 1H), 1.86-1.61 (m, 7H), 1.57-1.37 (m, 1H).
Protein kinases are a large group of intracellular and transmembrane signaling proteins in eukaryotic cells. These enzymes are responsible for transfer of the terminal (gamma) phosphate from ATP to specific amino acid residues of target proteins.
Phosphorylation of specific amino acid residues in target proteins can modulate their activity leading to profound changes in cellular signaling and metabolism. Protein kinases can be found in the cell membrane, cytosol and organelles such as the nucleus and are responsible for mediating multiple cellular functions including metabolism, cellular growth and differentiation, cellular signaling, modulation of immune responses, and cell death. Serine kinases specifically phosphorylate serine or threonine residues in target proteins. Similarly, tyrosine kinases, including tyrosine receptor kinases, phosphorylate tyrosine residues in target proteins. Tyrosine kinase families include: TEC, SRC, ABL, JAK, CSK, FAK, SYK, FER, ACK and the receptor tyrosine kinase subfamilies including ERBB, FGFR, VEGFR, RET and EPH. Subclass I of the receptor tyrosine kinase superfamily includes the ERBB receptors and comprises four members: ErbB1 (also called epidermal growth factor receptor (EGFR)), ErbB2, ErbB3 and ErbB4.
Kinases exert control on key biological processes related to health and disease. Furthermore, aberrant activation or excessive expression of various protein kinases are implicated in the mechanism of multiple diseases and disorders characterized by benign and malignant proliferation, as well as diseases resulting from inappropriate activation of the immune system. Thus, inhibitors of select kinases or kinase families are considered useful in the treatment of cancer, vascular disease, autoimmune diseases, and inflammatory conditions including, but not limited to: solid tumors, hematological malignancies, thrombus, arthritis, graft versus host disease, lupus erythematosus, psoriasis, colitis, illeitis, multiple sclerosis, uveitis, coronary artery vasculopathy, systemic sclerosis, atherosclerosis, asthma, transplant rejection, allergy, ischemia, dermatomyositis, pemphigus, and the like.
Tec kinases are a family of non-receptor tyrosine kinases predominantly, but not exclusively, expressed in cells of hematopoietic origin. The Tec family includes TEC, Bruton’s tyrosine kinase (BTK), inducible T-cell kinase (ITK), resting lymphocyte kinase (RLK/TXK for Tyrosine Protein Kinase), and bone marrow-expressed kinase (BMX/ETK).
BTK is important in B-cell receptor signaling and regulation of B-cell development and activation. Mutation of the gene encoding BTK in humans leads to X-linked agammaglobulinemia which is characterized by reduced immune function, including impaired maturation of B-cells, decreased levels of immunoglobulin and peripheral B cells, and diminished T-cell independent immune response. BTK is activated by Src-family kinases and phosphorylates PLC gamma leading to effects on B-cell function and survival. Additionally, BTK is important for cellular function of mast cells, macrophage and neutrophils indicating that BTK inhibition is effective in treatment of diseases mediated by these and related cells including inflammation, bone disorders, and allergic disease. BTK inhibition is also important in survival of lymphoma cells indicating that inhibition of BTK is useful in the treatment of lymphomas and other cancers. As such, inhibitors of BTK and related kinases are of great interest as anti-inflammatory, as well as anti-cancer, agents. BTK is also important for platelet function and thrombus formation indicating that BTK-selective inhibitors are also useful as antithrombotic agents. Furthermore, BTK is required for inflammasome activation, and inhibition of BTK may be used in treatment of inflammasome-related disorders, including; stroke, gout, type 2 diabetes, obesity-induced insulin resistance, atherosclerosis and Muckle-Wells syndrome. In addition, BTK is expressed in HIV infected T-cells and treatment with BTK inhibitors sensitizes infected cells to apoptotic death and results in decreased virus production. Accordingly, BTK inhibitors are considered useful in the treatment of HIV-AIDS and other viral infections.
Further, BTK is important in neurological function. Specifically targeting BTK in the brain and CNS has the potential to significantly advance the treatment of neurological diseases such as progressive and relapsing forms of MS and primary CNS lymphoma (PCNSL).
PCNSL is a rare brain tumor with an annual incidence in the United States of approximately 1900 new cases each year and constitutes approximately 3% of all newly diagnosed brain tumors.
PCNSL is highly aggressive and unlike other lymphomas outside the CNS, prognosis remains poor despite improvements in treatments in the front-line setting. High dose methotrexate remains the backbone of treatment and is used in combination with other cytotoxic agents, and more recently the addition of rituximab. From initial diagnosis, 5-year survival has improved from 19% to 30% between 1990 and 2000 but has not improved in the elderly population (>70 years), due to 20% or more of these patients being considered unfit for chemotherapy. Tumor regression is observed in ~85% of patients regardless of the treatment modality in the front-line setting, however, approximately half of these patients will experience recurrent disease within 10 -18 months after initial treatment and most relapses occur within the first 2 years of diagnosis.
Thus, the prognosis for patients with relapsed/refractory PCNSL (R/R PCNSL) remains poor with a median survival of ~ 2 months without further treatment. As there is no uniform standard of care for the treatment of R/R PCNSL, participation in clinical trials is encouraged. New safe and effective treatments are urgently needed.
BTK is involved in the signal transduction in the B cell antigen receptor (BCR) signaling pathway and integrates BCR and Toll-like receptor (TLR) signaling. Genes in these pathways frequently harbor mutations in diffuse large B-cell lymphoma (DLBCL), including CD79B and myeloid differentiation primary response 88 (MyD88). Ibrutinib, a first-generation irreversible selective inhibitor of BTK, has been approved for chronic lymphocytic leukemia/small cell lymphocytic lymphoma (CLL/SLL), previously treated Mantle Cell lymphoma (MCL) and Marginal Zone
Lymphoma (MZL), Waldenström’s macroglobulin, and previously treated chronic Graft Versus Host Disease. In clinical studies the recommended dose of Ibrutinib (480 mg/d in CLL or 560 mg/d in MCL) was escalated to 840 mg to achieve adequate brain exposure in primary CNS lymphoma.
Aberrant activation of the NF-κB pathway in PCNSL is emerging as a potential mechanism for more targeted therapy. In particular, activating mutations of CARD11 as well as of MyD88 (Toll-like receptor pathway) have been implicated. The activating exchange of leucine to proline at position 265 of MyD88, noted to occur in between 38% (11/29) and50% (7/14) of patients, is the most frequent mutation identified thus far in PCNSL. In addition, the coding region of CD79B, a component of the B-cell receptor signaling pathway, appears to contain mutations in 20% of cases, suggesting that dysregulation of the B-cell receptor and NF-κB pathways contribute to the pathogenesis of PCNSL. These data suggest that BCR pathway mutations and BTK dependence are of particular relevance to PCNSL.
Recently, several clinical studies have reported substantial single-agent clinical activity in the treatment of PCNSL with response rates of 70-77%. The majority of patients, however, discontinued therapy by 9 months. Although Ibrutinib therapy has been reported to be generally well tolerated with manageable adverse events, there are reports of sometimes fatal fungal infections. Of note, escalating doses beyond 560 mg to 840mg/day have been used to achieve higher brain exposure and these higher doses may be associated with off-target effects mediated by Ibrutinib’s kinase selectivity profile. Finally, the combination of high dose Ibrutinib in conjunction with high-dose steroids may contribute to exacerbate the increased fungal infections. Therefore, there remains a need for BTK inhibitors with an improved efficacy and safety profile due to greater brain penetration and BTK inactivation rate with greater kinase selectivity.
There remains a need for compounds that modulate protein kinases generally, as well as compounds that modulate specific protein kinases, such as BTK, as well as compounds that modulate specific protein kinases and selectively cross the blood/brain barrier for related compositions and methods for treating diseases, disorders and conditions that would benefit from such modulation and selectivity.
/////////////Cinsebrutinib, 7BS8743F3E, PHASE 1
CEFILAVANCIN



CEFILAVANCIN, TD-1792
CAS 722454-12-8
C87H96Cl3N16O28S2, 1984.28
F76229E21M
Vancomycin, 26-[[[3-[[(Z)-[1-(2-amino-5-chloro-4-thiazolyl)-2-[[(6R,7R)-2-carboxy-8-oxo-3-(pyridiniomethyl)-5-thia-1-azabicyclo[4.2.0]oct-2-en-7-yl]amino]-2-oxoethylidene]amino]oxy]propyl]amino]carbonyl]-26-decarboxy-
1-{[(6R,7R)-7-[(2Z)-2-(2-amino-5-chloro-1,3-thiazol-4-yl)-2-[(3-{[(1S,2R,18R,19R,22S,25R,28R,40S)-48-{[(2S,3R,4S,5S,6R)-3-{[(2S,4S,5S,6S)-4-amino-5-hydroxy-4,6-dimethyloxan-2-yl]oxy}-4,5-dihydroxy-6-(hydroxymethyl)oxan-2-yl]oxy}-22-(carbamoylmethyl)-5,47-dichloro-2,18,32,35,37-pentahydroxy-19-[(2R)-4-methyl-2-(methylamino)pentanamido]-20,23,26,42,44-pentaoxo-7,13-dioxa-21,24,27,41,43-pentaazaoctacyclo[26.14.2.2^{3,6}.2^{14,17}.1^{8,12}.1^{29,33}.0^{10,25}.0^{34,39}]pentaconta-3,5,8,10,12(48),14,16,29(45),30,32,34(39),35,37,46,49-pentadecaen-40-yl]formamido}propoxy)imino]acetamido]-2-carboxylato-8-oxo-5-thia-1-azabicyclo[4.2.0]oct-2-en-3-yl]methyl}pyridin-1-ium
Phase III Skin and soft tissue infections
- OriginatorGlaxoSmithKline; Theravance
- DeveloperR-Pharm; Theravance Biopharma
- ClassAcetamides; Antibacterials; Azabicyclo compounds; Beta-lactams; Cephalosporins; Peptide antibiotics; Pyridines; Thiazoles
- Mechanism of ActionCell wall inhibitors
BUILDING BLOCK
Vancomycin,

| Formula | C66H75Cl2N9O24 |
| Molar mass | 1449.27 g·mol−1 |
Cefilavancin (TD-1792) is an experimental antibiotic medication developed for the treatment of bacterial infections such as drug-resistant strains of Staphylococcus aureus. It is a prodrug which is also a codrug, injected intravenously and then cleaved inside the body to two active components, one of which is a modified form of vancomycin and the other a cephalosporin antibiotic. In clinical trials cefilavancin has shown similar efficacy with reduced side effects compared to vancomycin itself.[1][2][3][4][5][6][7][8]
- 31 Jan 2020Cefilavancin is still in phase III trials for Skin and soft tissue infection in Russia and Georgia (R-Pharm pipeline, January 2020)
- 17 Jun 2015Phase II development is ongoing the USA
- 02 Jun 2014Theravance Biopharma is formed as a spin-off of Theravance
SCHEME

SYN
WO2003031449
https://patentscope.wipo.int/search/en/WO2003031449
cheme A
REF
Li, Huijuan; ET AL, Medicine (Philadelphia, PA, United States) (2022), 101(34), e30120
References
- ^ Long DD, Aggen JB, Chinn J, Choi SK, Christensen BG, Fatheree PR, et al. (October 2008). “Exploring the positional attachment of glycopeptide/beta-lactam heterodimers”. The Journal of Antibiotics. 61 (10): 603–614. doi:10.1038/ja.2008.80. PMID 19168974.
- ^ Tyrrell KL, Citron DM, Warren YA, Goldstein EJ (April 2012). “In vitro activity of TD-1792, a multivalent glycopeptide-cephalosporin antibiotic, against 377 strains of anaerobic bacteria and 34 strains of Corynebacterium species”. Antimicrobial Agents and Chemotherapy. 56 (4): 2194–2197. doi:10.1128/AAC.06274-11. PMC 3318369. PMID 22290981.
- ^ Stryjewski ME, Potgieter PD, Li YP, Barriere SL, Churukian A, Kingsley J, et al. (November 2012). “TD-1792 versus vancomycin for treatment of complicated skin and skin structure infections”. Antimicrobial Agents and Chemotherapy. 56 (11): 5476–5483. doi:10.1128/aac.00712-12. PMC 3486540. PMID 22869571.
- ^ Douglas EJ, Laabei M (September 2023). “Staph wars: the antibiotic pipeline strikes back”. Microbiology. 169 (9). Reading, England. doi:10.1099/mic.0.001387. PMC 10569064. PMID 37656158.
- ^ Surur AS, Sun D (2021). “Macrocycle-Antibiotic Hybrids: A Path to Clinical Candidates”. Frontiers in Chemistry. 9: 659845. Bibcode:2021FrCh….9..317S. doi:10.3389/fchem.2021.659845. PMC 8120311. PMID 33996753.
- ^ Saxena D, Maitra R, Bormon R, Czekanska M, Meiers J, Titz A, et al. (December 2023). “Tackling the outer membrane: facilitating compound entry into Gram-negative bacterial pathogens”. npj Antimicrobials and Resistance. 1 (1): 17. doi:10.1038/s44259-023-00016-1. PMC 11721184. PMID 39843585.
- ^ Koh AJ, Thombare V, Hussein M, Rao GG, Li J, Velkov T (2023). “Bifunctional antibiotic hybrids: A review of clinical candidates”. Frontiers in Pharmacology. 14: 1158152. doi:10.3389/fphar.2023.1158152. PMC 10313405. PMID 37397488.
- ^ Homer JA, Johnson RM, Koelln RA, Moorhouse AD, Moses JE (2024). “Strategic re-engineering of antibiotics”. Nature Reviews Bioengineering. doi:10.1038/s44222-024-00250-w.
| Clinical data | |
|---|---|
| Other names | TD-1792 |
| Routes of administration | Intravenous |
| Identifiers | |
| showIUPAC name | |
| CAS Number | 722454-12-8 |
| PubChem CID | 76960417 |
| DrugBank | DB05735 |
| ChemSpider | 34990483 |
| UNII | F76229E21M |
| ChEMBL | ChEMBL4297645 |
| Chemical and physical data | |
| Formula | C87H95Cl3N16O28S2 |
| Molar mass | 1983.27 g·mol−1 |
| 3D model (JSmol) | Interactive image |
| showSMILES | |
| showInChI | |
////////////CEFILAVANCIN, TD-1792, TD 1792, F76229E21M, цефилаванцин, 头孢拉凡星, سيفيلافانسين , GlaxoSmithKline, Theravance, PHASE 3

 DRUG APPROVALS BY DR ANTHONY MELVIN CRASTO
.....
DRUG APPROVALS BY DR ANTHONY MELVIN CRASTO
.....










