Home » Uncategorized (Page 100)
Category Archives: Uncategorized
TORCETRAPIB Revisted



Torcetrapib (CP-529,414, Pfizer) was a drug being developed to treat hypercholesterolemia (elevated cholesterol levels) and prevent cardiovascular disease. Its development was halted in 2006 when phase III studies showed excessive all-cause mortality in the treatment group receiving a combination of atorvastatin (Lipitor) and torcetrapib.

Medical uses
Torcetrapib has not been found to affect either cardiovascular disease or risk of death in those already taking a statin.[1]
Mechanism
Torcetrapib acts (as a CETP inhibitor) by inhibiting cholesterylester transfer protein (CETP), which normally transfers cholesterol from HDL cholesterol to very low density or low density lipoproteins (VLDL or LDL). Inhibition of this process results in higher HDL levels (the “good” cholesterol-containing particle) and reduces LDL levels (the “bad” cholesterol).[vague][citation needed]
Development
The first step in the synthesis was a recently created reaction of amination to p-chlorotrifluoryltoluene, a reaction that was created by Dr. Stephen Buchwald at MIT.[2]
Development of the drug began around 1990; it was first administered in humans in 1999, and manufacturing at production scale began in Ireland in 2005.[3]
Pfizer had previously announced that torcetrapib would be sold in combination with Pfizer’s statin, atorvastatin (Lipitor); however, following media and physician criticism, Pfizer had subsequently planned for torcetrapib to be sold independently of Lipitor.[4]
Clinical trials
A 2004 trial (19 subjects, non-randomised) showed that torcetrapib could increase HDL and lower LDL with and without an added statin.[5]
Nine phase III studies were completed.[6][7][8][9][10][11][12][13][14][15]
Early termination of study
On December 2, 2006 Pfizer cut off torcetrapib’s phase III trial because of “an imbalance of mortality and cardiovascular events” associated with its use.[16] This was a sudden and unexpected event and as late as November 30, 2006 Jeff Kindler, Pfizer’s chief executive, was quoted, “This will be one of the most important compounds of our generation.”[16] In the terminated trial, a 60% increase in deaths was observed among patients taking torcetrapib and atorvastatin versus taking atorvastatin alone.[17] Pfizer recommended that all patients stop taking the drug immediately.[18]
Six studies were terminated early.[6] One of the completed studies found it raised systolic blood pressure and concluded “Torcetrapib showed no clinical benefit in this or other studies, and will not be developed further.”[19]
The drug cost $800m+ to bring into Phase III development.[20]




| A Concise Asymmetric Synthesis of Torcetrapib�, M. Guino, P. H. Phua, J-C. Caille and K. K. Hii, J. Org. Chem., 2007, 72, 6290-6293.doi:10.1021/jo071031gAbstract: Optically active torcetrapib was synthesized in seven steps from achiral precursors without the need for protecting groups, utilizing an enantioselective aza-Michael reaction to achieve asymmetry. |

Example 9 Anhydrous, (-)-(2R,4S)-4-[(3,5-Bιs-trιfluoromethyl-benzyl)-methoxycarbonyl-amιnol-2- ethyl-6-trιfluoromethyl-3,4-dιhydro-2H-quιnolιne-1 -carboxylic acid ethyl ester.
A 2.6g portion of 4(S)-[(3,5-bιs-tπfluoromethyl-benzyl)-methoxycarbonyl-amιno]-2(R)- ethyl-6-tπfluoromethyl-3,4-dιhydro-2H-quιnolιne-1 -carboxylic acid ethyl ester (a mixture of predominantly amorphous material with traces of ethanolate crystalline form; the title compound was also prepared in an analogous manner starting from pure amorphous or pure ethanolate material) was charged to 13 milliliters of hexanes and heated to effect a solution at about 60°C The heat was removed and the reaction was allowed to cool to ambient over a one hour period The reaction was seeded with anhydrous (-)-(2R,4S)-4-[(3,5-bιs-tπfluoromethyl-benzyl)- methoxycarbonyl-amιno]-2-ethyl-6-trιfluoromethyl-3,4-dιhydro-2H-quιnolιne-1 – carboxylic acid ethyl ester and granulated for eighteen hours under ambient conditions. Alternately, the anhydrous crystals may be prepared from hexanes without seeding. The product was collected by filtration and air dried. The isolated product X-ray pattern matched the calculated powder pattern. Density: 1.406 Crystal System: Trigonal
Microscopy: Well formed rods and equant (fractured rods) crystals demonstrating high birefringence when viewed across the C axis. Being in the Trigonal crystal system the crystals do not demonstrate birefringence when viewed down the C axis. The crystals demonstrate a cleavage plane perpendicular to the C axis Fusion Microsocopy In Type A oil dissolution at 50°C.
Dry — clear melt at 86°C.
NMR: No trace of ethanolate
Degree of crystallmity: Highly crystalline Hygroscopicity. Non-hygroscopic at 100% relative humidity over 48 hours.
Appearance: Free flowing white powder

References
- Clark, RW; Sutfin TA, Ruggeri RB, Willauer AT, Sugarman ED, Magnus-Aryitey G, Cosgrove PG, Sand TM, Wester RT, Williams JA, Perlman ME, Bamberger MJ (January 22, 2004). “Raising high-density lipoprotein in humans through inhibition of cholesteryl ester transfer protein: an initial multidose study of torcetrapib”. Arteriosclerosis, Thrombosis, and Vascular Biology 24 (3): 490–497. doi:10.1161/01.ATV.0000118278.21719.17. PMID 14739125. Retrieved 2006-12-03.
- Clark, RW; Ruggeri RB; Cunningham D; Bamberger MJ (March 2006). “Description of the torcetrapib series of cholesteryl ester transfer protein inhibitors, including mechanism of action”. Journal of Lipid Research 47 (3): 537–552. doi:10.1194/jlr.M500349-JLR200. PMID 16326978. Retrieved 2006-12-03.
- Davidson, MH; McKenny JM; Shear CL; Revkin JH (November 7, 2006). “Efficacy and safety of torcetrapib, a novel cholesteryl ester transfer protein inhibitor, in individuals with below-average high-density lipoprotein cholesterol levels”. Journal of the American College of Cardiology 48 (9): 1774–1781. doi:10.1016/j.jacc.2006.06.067.PMID 17084249. Retrieved 2006-12-03.
- McKenny, JM; Davidson MH; Shear CL; Revkin JH (November 7, 2006). “Efficacy and safety of torcetrapib, a novel cholesteryl ester transfer protein inhibitor, in individuals with below-average high-density lipoprotein cholesterol levels on a background of atorvastatin”. Journal of the American College of Cardiology 48 (9): 1782–1790.doi:10.1016/j.jacc.2006.06.066. PMID 17084250. Retrieved 2006-12-03.
Notes
- Keene, D; Price, C; Shun-Shin, MJ; Francis, DP (Jul 18, 2014). “Effect on cardiovascular risk of high density lipoprotein targeted drug treatments niacin, fibrates, and CETP inhibitors: meta-analysis of randomised controlled trials including 117,411 patients.”. BMJ (Clinical research ed.) 349: g4379. PMID 25038074.
- Buchwald, Stephen (July 23, 2004). “Research Projects”. Retrieved 2007-10-04.
- “Pfizer Begins Production at Torcetrapib/Atorvastatin Manufacturing Facility” (Press release). Pfizer. June 22, 2005. Retrieved 2006-12-03.
- Berenson, Alex (July 26, 2006). “Heart Pill to Be Sold by Itself”. Business (The New York Times). Retrieved 2006-12-03.
- Brousseau, ME; Schaefer EJ; Wolfe ML; Bloedon LT; Digenio AG; Clark RW; Mancuso JP; Rader DJ (April 8, 2004). “Effects of an inhibitor of cholesteryl ester transfer protein on HDL cholesterol” (abstract). New England Journal of Medicine 350 (15): 1505–1515. doi:10.1056/NEJMoa031766. PMID 15071125. Retrieved 2006-12-03.
- http://clinicaltrials.gov/ct2/results?term=torcetrapib
- http://clinicaltrials.gov/ct2/show/NCT00139061 Phase III Assess HDL-C Increase And Non-HDL Lowering Effect Of Torcetrapib/Atorvastatin Vs. Fenofibrate
- http://clinicaltrials.gov/ct2/show/NCT00134511 Phase III Study To Evaluate The Effect Of Torcetrapib/Atorvastatin In Patients With Genetic High Cholesterol Disorder
- http://clinicaltrials.gov/ct2/show/NCT00134485 Phase III Study To Evaluate The Safety And Efficacy Of Torcetrapib/Atorvastatin In Subjects With Familial Hypercholerolemia
- http://clinicaltrials.gov/ct2/show/NCT00134498 Phase III Study Comparing The Efficacy & Safety Of Torcetrapib/Atorvastatin And Atorvastatin In Subjects With High Triglycerides
- http://clinicaltrials.gov/ct2/show/NCT00267254 Phase III Clinical Trial Comparing Torcetrapib/Atorvastatin To Simvastatin In Subjects With High Cholesterol
- http://clinicaltrials.gov/ct2/show/NCT00138762 Phase III Study of Torcetrapib/Atorvastatin vs Atorvastatin Alone or Placebo in Patients With High Cholesterol
- http://clinicaltrials.gov/ct2/show/NCT00134173 Phase III Coronary IVUS Study to Compare Torcetrapib/Atorvastatin to Atorvastatin Alone in Subjects With Coronary Heart Disease (ILLUSTRATE)
- http://clinicaltrials.gov/ct2/show/NCT00137462 Phase III Lipitor Trial To Study The Effect Of Torcetrpib/Atorvastatin To Atorvastatin Alone.
- http://clinicaltrials.gov/ct2/show/NCT00136981 Phase III Carotid B-Mode Ultrasound Study to Compare Anti-Atherosclerotic Effect of Torcetrpib/Atorvastatin to Atorvastatin Alone. (RADIANCE 1)
- Berenson, Alex (December 3, 2006). “Pfizer Ends Studies on Drug for Heart Disease”. The New York Times. Retrieved 2006-12-03. (registration required)
- Theresa Agovino (Associated Press) (December 3, 2006). “Pfizer ends cholesterol drug development”. Yahoo! News. Retrieved 2006-12-03.[dead link] Each study arm (torcetrapib + atorvastatin vs. atorvastatin alone) had 7500 patients enrolled; 51 deaths were observed in the atorvastatin alone arm, while 82 deaths occurred in the torcetrapib + atorvastatin arm. (Link dead as of 15 January 2007)
- Associated Press (December 2, 2006). “Pfizer cuts off cholesterol drug trials”. Yahoo! News (Yahoo.com). Retrieved 2006-12-03.[dead link] (Link dead as of 15 January 2007)
- Bots et al.; Visseren, Frank L; Evans, Gregory W; Riley, Ward A; Revkin, James H; Tegeler, Charles H; Shear, Charles L; Duggan, William T et al. (July 2007). “Torcetrapib and carotid intima-media thickness in mixed dyslipidaemia (RADIANCE 2 study): a randomised, double-blind trial”. The Lancet 370 (9582): 153–160. doi:10.1016/S0140-6736(07)61088-5.
- Cutler, D. M. (2007-03-29). “The Demise of the Blockbuster?”. The New England Journal of Medicine (Massachusetts Medical Society) 356 (13): 1292–1293. doi:10.1056/NEJMp078020.ISSN 1533-4406. PMID 17392299. Retrieved 2007-04-23.
External links
Troglitazone (Romglizone) an antidiabetic Revisted

Troglitazone, GR-92132X, CI-991, CS-045, Romozin, Prelay, Rezulin, Noscal
CAS 97322-87-7
- CI 991
- CS 045
- Depotox
- GR 92132X
- Noscal
- Rezulin
- Romglizone
- Troglitazone
Withdrawn – 2000
Crystals, m.p. 184-6 °C
Daiichi Sankyo Co., Ltd. INNOVATOR
Troglitazone
 Type-II diabetes mellitus (DM) is characterized by insulin resistance, glucose intolerance, increased hepatic glucose production, and decreased pancreatic insulin secretion. In the past, the drug classes used for type-II DM have targeted the last three of these abnormalities. Sulfonylurea agents bind to ATP-dependent potassium efflux channels to stimulate pancreatic insulin secretion at b-islet cells. The biguanides decrease hepatic glucose production, and thea-glucosidase inhibitors delay carbohydrate digestion to improve glucose tolerance. Until the recent advent of the thiazolidinedione drugs (ciglitazone was first synthesized in 1982), there was no therapy specifically targeting insulin resistance. Drugs of this class all share a common thiazolidine-2-4-dione structure. Marketed drugs of this class include pioglitazone, rosiglitazone, and troglitazone [Figure 1] – the first to reach the market.
Type-II diabetes mellitus (DM) is characterized by insulin resistance, glucose intolerance, increased hepatic glucose production, and decreased pancreatic insulin secretion. In the past, the drug classes used for type-II DM have targeted the last three of these abnormalities. Sulfonylurea agents bind to ATP-dependent potassium efflux channels to stimulate pancreatic insulin secretion at b-islet cells. The biguanides decrease hepatic glucose production, and thea-glucosidase inhibitors delay carbohydrate digestion to improve glucose tolerance. Until the recent advent of the thiazolidinedione drugs (ciglitazone was first synthesized in 1982), there was no therapy specifically targeting insulin resistance. Drugs of this class all share a common thiazolidine-2-4-dione structure. Marketed drugs of this class include pioglitazone, rosiglitazone, and troglitazone [Figure 1] – the first to reach the market.
The “glitazones” act to reduce insulin resistance and also correct hyperglycemia, hyperinsulinemia, and hypertriglyceridemia. Thiazolidinediones bind to the gisoform of the peroxisome proliferator-activated receptor (PPARg), a nuclear transcription factor that regulates the expression of several insulin-responsive genes involved in glucose and lipid metabolism, and the differentiation of fibroblasts into adipose tissue. The net effect is to reduce insulin resistance, mostly through increased glucose uptake by muscle tissue; however, the exact biochemical mechanism is unclear. Effects on lipid metabolism include decreased triglycerides and free fatty acids, and a slight increase or no change in high-density lipoprotein, low-density lipoprotein, and total cholesterol. There also appear to be acute increases in insulin-stimulated glucose uptake that are PPAR-independent. This effect is too rapid to occur via gene transcription, and in the case of troglitazone may result from action of its quinone metabolite. Troglitazone also decreases production of various inflammatory mediators and may antagonize TNFa.
Troglitazone�s most common adverse effect is fluid retention, which may increase preload and induce cardiac hypertrophy. Troglitazone is contraindicated in congestive heart failure, and cases of pulmonary edema have been reported. Troglitazone induces colon polyps in murine models and is therefore contraindicated for patients with familial polyposis coli. Troglitazone and pioglitazone (but not rosiglitazone) induce cytochrome P450 (CYP) 3A4. This enzyme induction can result in decreased drug levels or drug effects with estradiol, terfenadine, cyclosporine, simvistatin, tacrolimus, and other drugs metabolized by CYP 3A4. A small fraction of troglitazone is metabolized by CYP (not 3A4) to an active quinone metabolite, but it is mostly conjugated to sulfate and glucuronide. Troglitazone enhances the anticoagulant effect of warfarin, probably through competitive serum protein binding, and has other drug interactions at the PPAR level. Troglitazone interferes with gemfibrozil’s binding to PPARa, and may decrease NSAID effectiveness by competing for PPARg.
Rezulin� (tradename troglitazone by Parke-Davis) was FDA approved January 29, 1997, and was first marketed in March 1997. Over 600,000 American patients received troglitazone, with an additional 200,000 in Japan. Pre-marketing studies showed 1.9% of patients on troglitazone developed serum alanine aminotransferase levels in excess of three times the upper limit of normal, vs. 0.6% with placebo. Such hepatotoxicity was typically asymptomatic and reversible. A few patients developed overt liver injury, and two liver biopsies among these patients showed hepatocellular injury pattern. It was estimated that only 1 patient in 50,000 to 60,000 would die from liver failure or require liver transplantation. On November 3, 1997, the FDA released a warning regarding 150 adverse events with troglitazone, 35 with acute liver injury, and 3 deaths in Japan from liver failure. The warnings and restrictions about troglitazone were extended in December 1997, July 1998, and June 1999. Troglitazone was voluntarily withdrawn from the US market on March 21, 2000, after it had been demonstrated that Rezulin� was more toxic than either Avandia� (rosiglitazone) or Actos�(pioglitazone).
Troglitazone hepatotoxicity appears to be idiosyncratic. The onset is typically delayed, usually 2-5 months after initiating therapy, although one case was reported after only four doses. Although hypersensitivity has been suggested in several cases, the hallmarks of immune mechanisms, fever, rash, and eosinophilia, are usually absent. Histologic specimens usually show hepatocellular injury, bridging fibrosis and necrosis, intracanalicular cholestasis, and lack of regenerative activity. Samples vary in the amount of WBC infiltration (with or without eosinophils) and steatosis.
Idiosyncratic (or host-dependent) drug reactions are either due to hypersensitivity or to metabolic aberrations. It is not clear whether troglitazone hepatotoxicity is caused by hypersensitivity. Proposed metabolic aberrations include oxidation/reduction reactions with the a-tocopherol moiety on troglitazone (although it is usually considered an antioxidant), reactions from the quinone metabolite (similar to acetaminophen’s quinone metabolite), and genetic variations in cytokines and their receptors, the apoptosis cascade, mitochondrial respiration, and regenerative response. It is unlikely that CYP polymorphisms play a major role, as the incidence of troglitazone hepatotoxicity is too low. Two cases of hepatic toxicity associated with rosiglitazone have also been reported. Although the patients had co-morbidities, exposures to other drugs, and one case may have been due to shock, these cases suggest that hepatotoxicity may be an emerging “class-effect” of thiazolidinediones.
Troglitazone (Rezulin, Resulin, Romozin, Noscal) is an antidiabetic and anti-inflammatory drug, and a member of the drug class of the thiazolidinediones. It was prescribed for patients with diabetes mellitus type 2.[1] It was developed by Daiichi Sankyo Co.(Japan). In the United States, it was introduced and manufactured by Parke-Davis in the late 1990s, but turned out to be associated with an idiosyncratic reaction leading to drug-induced hepatitis. One F.D.A. medical officer evaluating troglitazone, John Gueriguian, did not recommend its approval due to potential high liver toxicity,[2] but a full panel of experts approved it in January 1997.[3] Once the prevalence of adverse liver effects became known, troglitazone was withdrawn from the British market in December 1997, from the United States market in 2000, and from the Japanese market soon afterwards. It didn’t get approval in the rest of Europe.
Approval history
Troglitazone was developed as the first anti-diabetic drug having a mechanism of action involving the enhancement of insulin sensitivity. At the time it was widely believed that such drugs, by addressing the primary metabolic defect associated with Type 2 diabetes, would have numerous benefits including avoiding the risk of hypoglycemia associated with insulin and earlier oral antidiabetic drugs. It was further believed that reducing insulin resistance would potentially reduce the very high rate of cardiovascular disease that is associated with diabetes.[4][5]
Parke-Davis/Warner Lambert submitted the diabetes drug Rezulin for U.S. Food and Drug Administration (F.D.A.) review on July 31, 1996. The medical officer assigned to the review, Dr. John L. Gueriguian, cited Rezulin’s potential to harm the liver and the heart and he questioned its viability in lowering blood sugar for patients with adult-onset diabetes, recommending against the drug’s approval. After complaints from the drugmaker, Gueriguian was removed on November 4, 1996 and his review was purged by the F.D.A.[6][7]Gueriguian and the company had a single meeting, at which Gueriguian used “intemperate” language; The company said it’s objections were based on inappropriate remarks made by Gueriguian.[8] Parke-Davis said at the advisory committee that the risk of liver toxicity was comparable to placebo and that additional data of other studies confirmed this.[9] According to Peter Gøtzsche, when the company provided these additional data one week after approval, they showed a substantial greater risk for liver toxicity.[10]
The F.D.A. approved the drug on January 29, 1997, and it appeared in pharmacies in late March. At the time Dr. Solomon Sobel, a director at the F.D.A., overseeing diabetes drugs, said in a New York Times interview that adverse effects of troglitazone appeared to be rare and relatively mild.[11]
Glaxo Wellcome P.L.C. received approval from the British Medicines Control Agency (MCA) to market troglitazone, as Romozin, in July 1997.[12] After reports of sudden liver failure in patients receiving the drug, the Parke-Davis and the FDA added warnings to the drug label requiring monthly monitoring of liver enzyme levels.[13] Glaxo removed troglitazone from the market in Britain on December 1, 1997.[6] Glaxo had licensed the drug from Sankyo Company of Japan and had sold it in Britain from October 1, 1997.[14][15]
On May 17, 1998, a 55-year old patient named Audrey LaRue Jones died of acute liver failure after taking troglitazone. Importantly, she had been monitored closely by physicians at the National Institutes of Health as a participant in the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) diabetes prevention study.[16][17] This called into question the efficacy of the monitoring strategy. The N.I.H. responded on June 4 by dropping troglitazone from the study.[7][18] Dr. David J. Graham, an F.D.A. epidemiologist charged with evaluating the drug, warned on March 26, 1999 of the dangers of using it and concluded that patient monitoring was not effective in protecting against liver failure. He estimated that the drug could be linked to over 430 liver failures and that patients incurred 1,200 times greater risk of liver failure when taking Rezulin.[7][19] Dr. Janet B. McGill, an endocrinologist who had assisted in the Warner–Lambert’s early clinical testing of Rezulin, wrote in a March 1, 2000 letter to Sen. Edward M. Kennedy (D-Mass.): “I believe that the company . . . deliberately omitted reports of liver toxicity and misrepresented serious adverse events experienced by patients in their clinical studies.”[20]
On March 21, 2000, the F.D.A. withdrew the drug from the market.[21] Dr. Robert I. Misbin, an F.D.A. medical officer, wrote in a July 3, 2000 letter to the House Energy and Commerce Committee of strong evidence that Rezulin could not be used safely, after having been threatened by the FDA with dismissal in March 2000.[6][22] By that time the drug had been linked to 63 liver-failure deaths and had generated sales of more than $2.1 billion for Warner-Lambert.[19] The drug cost $1,400 a year per patient in 1998.[15] Pfizer, which had acquired Warner-Lambert in February 2000, reported the withdrawal of Rezulin cost $136 million.[23]
Lawsuits
In 2009 Pfizer Inc. resolved all but three of 35,000 claims over its withdrawn diabetes drug Rezulin for a total of about $750 million. Pfizer, which acquired rival Wyeth for almost $64 billion, paid about $500 million to settle Rezulin cases consolidated in federal court in New York, according to court filings. The company also paid as much as $250 million to resolve state-court suits. In 2004, it set aside $955 million to end Rezulin cases.[24]
Mode of action
Troglitazone, like the other thiazolidinediones (pioglitazone and rosiglitazone), works by activating peroxisome proliferator-activated receptors (PPARs).
Troglitazone is a ligand to both PPARα and – more strongly – PPARγ. Troglitazone also contains an α-tocopheroyl moiety, potentially giving it vitamin E-like activity in addition to its PPAR activation. It has been shown to reduce inflammation:[25] troglitazone use was associated with a decrease of nuclear factor kappa-B (NF-κB) and a concomitant increase in its inhibitor (IκB). NFκB is an important cellular transcription regulator for the immune response.


rosiglitazone, ciglitazone, darglitazone, englitazone, rosiglitazone, pioglitazone, rosiglitazone, troglitazone
| Systematic (IUPAC) name | |
|---|---|
| (RS)-5-(4-[(6-hydroxy-2,5,7,8-tetramethylchroman-2-yl)methoxy]benzyl)thiazolidine-2,4-dione | |
| Clinical data | |
| Legal status |
?
|
| Pharmacokinetic data | |
| Half-life | 16-34 hours |
| Identifiers | |
| CAS number | 97322-87-7 |
| ATC code | A10BG01 |
| PubChem | CID 5591 |
| IUPHAR ligand | 2693 |
| DrugBank | DB00197 |
| ChemSpider | 5389 |
| UNII | I66ZZ0ZN0E |
| KEGG | D00395 |
| ChEBI | CHEBI:9753 |
| ChEMBL | CHEMBL408 |
| Chemical data | |
| Formula | C24H27NO5S |
| Mol. mass | 441.541 g/mol |
………………….

………………..

A new synthesis of [14C]-labeled CS-045 has been reported: The condensation of 5-acetoxy-2-hydroxy-3,4,6-trimethylacetophenone (I) with phenoxyacetone (II) by means of morpholine and p-toluenesulfonic acid in refluxing benzene gives 6-acetoxy-2,5,7,8-tetramethyl-2-(phenoxymethyl)-3,4-dihydro-2H-benzo[b]pyran-4-one (III), which is reduced with NaBH4 in methanol to the corresponding carbinol (IV). The dehydration of (IV) by means of p-toluenesulfonic acid in refluxing benzene affords 2-acetoxy-2,5,7,8-tetramethyl-2-(phenoxymethyl)-2H-benzo[b]pyran (V), which is hydrogenated with H2 over Pd/C in methanol to give the corresponding 3,4-dihydro derivative (VI). The hydrolysis of (VI) with NaOH in methanol yields the corresponding phenol (VII), which is chloromethylated with paraformaldehyde and dry HCl in dioxane to afford 2-[4-(chloromethyl)phenoxymethyl]-2,5,7,8-tetramethyl-3,4-dihydro-2H-benzo[b]pyran-6-ol (VIII). The protection of (VIII) with chloromethyl methyl ether by means of potassium tert-butoxide in THF gives the corresponding 6-(methoxymethoxy) derivative (IX), which is condensed with [5-14C]-thiazolidine-2,4-dione (X) by means of butyllithium in THF-HMPT to yield 5-[4-[6-(methoxymethoxy)-2,5,7,8-tetramethyl-3,4-dihydro-2H-benzo[b]pyran-2-ylmethoxy]benzyl]-[5-14C]-thiazolidine-2,4-dione (XI). Finally, this compound is deprotected with concentrated HCl in ethylene glycol monomethyl ether at 130 C.
……………….

A new short synthesis of troglitazone has been described: Condensation of the bromoacetal (I) with 4-hydroxybenzaldehyde (II) by means of K2CO3 and NaI in refluxing acetone gives the unsaturated ether (III), which is cyclized with trimethylhydroquinone (IV) by means of bis(trifluoromethylsulfonyl)imide in dichloromethane to yield the 6-hydroxybenzopyran (V). Acylation of (V) with acetic anhydride and DMAP in THF affords the expected acetoxybenzopyran (VI), which is condensed with thiazolidine-2,4-dione (VII) by means of piperidine in toluene to provide the 6-benzylidene-thiazolidine (VIII). The hydrogenation of (VIII) with H2 over Pd/C in methanol gives the corresponding benzyl derivative (IX), which is finally deacetylated with AcOH/HCl/water (3:1:1) in MeOH.
…………..
European Journal of Medicinal Chemistry, 51, 206-215; 2012
http://www.sciencedirect.com/science/article/pii/S0223523412001353

……………………………………….
see Indian Journal of Heterocyclic Chemistry, 15(4), 407-408; 2006
……………………………………………………….
Bioorganic & Medicinal Chemistry Letters, 14(10), 2547-2550; 2004
http://www.sciencedirect.com/science/article/pii/S0960894X04003038
(a) t-Butyldimethylsilyl chloride, imidazole, DMF; (b) LAH, rt, 3 h (75.9%, two steps); (c) 4-fluorobenzaldehyde, KtOBu, DMF, 80 °C, 8 h; (d) 2,4-thiazolidinedione, AcOH, piperidine, toluene, reflux, 4 h (37%, two steps); (e) HCl, MeOH, 15 min; (f) CoCl2, DMG (84%).
………………………
Patent
http://www.google.co.in/patents/US5700820
EXAMPLE-1
A mixture of 70 g of ethyl-3- 4-(6-acetoxy-2,5,7,8-tetramethylchroman-2-ylmethoxy)phenyl!-2-chloropropionate, 13.12 g of thiourea and 80.2 ml of sulpholane was reacted for 80 min., under a nitrogen stream at 115°-120° C. Subsequently, a 656.2 ml Acetic acid, 218.7 ml conc. hydrochloric acid and 109.4 ml water was added to this and the resulting mixture was further heated for 12 hrs at 85°-90° C. The reaction mixture was cooled to room temperature and 196.8 g of sodium bicarbonate was added and once the evolution of carbondioxide had ceased, the solvent was distilled off applying high vacuum. A 10:1 by volume mixture of benzene and ethyl acetate was added to the residue and the crude product was washed with a mixture of equal volumes of a saturated aq. sodium bicarbonate solution & water. The organic layer was dried over anhydrous sodium sulphate and the solvent was distilled off. The resulting crude product was quickly eluted from a silica gel column with 50% ethylacetate-hexane to furnish 40 g of the required 5-{4-(6-hydroxy-2, 5, 7, 8-tetramethylchroman-2-yl-methoxy) benzyl) thiazolidine-2,4-dione (Troglitazone) with a HPLC purity of ˜67-70%. The elution of column was continued further to yield 5- 4-(6-hydroxy-2,5,7,8-tetramethylchroman-2-yl-methoxy)benzyl!2-iminothiazolidine-4-one with HPLC purity of ˜70%.
Lit References:
Oral hypoglycemic agent which improves insulin sensitivity and decreases hepatic glucose production. Prepn: JP Kokai 85 51189; T. Yoshioka et al., US 4572912 (1985, 1986 both to Sankyo); T. Yoshioka et al.,
J. Med. Chem. 32,421 (1989).
Mechanism of action studies: T. P. Ciaraldi et al., Metabolism 39, 1056 (1990); M. Kellerer et al., Diabetes 43, 447 (1994).
Clinical evaluation: T. Kuzuya et al., Diabetes Res. Clin. Pract. 11, 147 (1991).
Clinical metabolic effects: S. L. Suter et al., Diabetes Care 15, 193 (1992).
References
- Fisher, Lawrence (4 November 1997). “Adverse Diabetes Drug News Sends Warner-Lambert Down”. The New York Times. Retrieved 12 December 2012.
- Retired Drugs: Failed Blockbusters, Homicidal Tampering, Fatal Oversights, wired.com
- Cohen, J. S. (2006). “Risks of troglitazone apparent before approval in USA”.Diabetologia 49 (6): 1454–5. doi:10.1007/s00125-006-0245-0. PMID 16601971.
- Henry RR (September 1996). “Effects of troglitazone on insulin sensitivity”. Diabet. Med.13 (9 Suppl 6): S148–50. PMID 8894499.
- Keen H (November 1994). “Insulin resistance and the prevention of diabetes mellitus”. N. Engl. J. Med. 331 (18): 1226–7. doi:10.1056/NEJM199411033311812. PMID 7935664.
- Willman, David (20 December 2000). “NEW FDA: Rezulin Fast-Track Approval and a Slow Withdrawal”. The Los Angeles Times. Retrieved 12 December 2012.
- Willman, David (4 June 2000). “The Rise and Fall of the Killer Drug Rezulin”. The Los Angeles Times. Retrieved 12 December 2012.
- “Report: FDA Removes Medical Officer”.
- Avorn, J (2005). Powerful medicines. New York: Vintage books.
- Gøtzsche, Peter (2013). Deadly medicines and organised crime : how big pharma has corrupted healthcare. London [u.a.]: Radcliffe Publ. p. 185. ISBN 9781846198847.
- Leary, Warren (31 January 1997). “New Class of Diabetes Drug Is Approved”. The New York Times. Retrieved 12 December 2012.
- Sinclair, Neil (31 July 1997). “Glaxo Wellcome gets approval for Romozin”. ICIS News. Retrieved 12 December 2012.
- “www.accessdata.fda.gov”.
- British Broadcasting Corporation (1 December 1997). “Diabetes drug withdrawn from sale”. BBC. Retrieved 12 December 2012.
- Fisher, Lawrence (17 January 1998). “Drug Makers at Threshold of a New Therapy; With a Dose of Biotechnology, Big Change Is Ahead in the Treatment of Diabetes”. The New York Times. Retrieved 12 December 2012.
- Diabetes Prevention Research Group (April 1999). “Design and methods for a clinical trial in the prevention of type 2 diabetes”. Diabetes Care 22 (4): 623–634.doi:10.2337/diacare.22.4.623. Retrieved 12 December 2012.
- Diabetes Prevention Program Research Group (7 February 2002). “Reduction in the Incidence of Type 2 Diabetes with Lifestyle Intervention or Metformin”. The New England Journal of Medicine 346 (6): 393–403. doi:10.1056/NEJMoa012512.PMC 1370926. PMID 11832527. Retrieved 12 December 2012.
- Gale, Edwin (January 2006). “Troglitazone: the lesson that nobody learned?”.Diabetologia 49 (1): 1–6. doi:10.1007/s00125-005-0074-6.
- Willman, David (16 August 2000). “FDA’s Approval and Delay in Withdrawing Rezulin Probed”. The Los Angeles Times. Retrieved 12 December 2012.
- Willman, David (10 March 2000). “Fears Grow Over Delay in Removing Rezulin”. The Los Angeles Times. Retrieved 12 December 2012.
- U.S. Food and Drug Administration. “2000 Safety Alerts for Human Medical Products”. U.S. Food and Drug Administration. Retrieved 12 December 2012.
- Willman, David (March 17, 2000). “Physician Who Opposes Rezulin Is Threatened by FDA With Dismissal”. Los Angeles Times.
- Pfizer. “Pfizer Annual Report 2001”. Pfizer. Retrieved 12 December 2012.
- Feeley, Jef (March 31, 2009). “Pfizer Ends Rezulin Cases With $205 Million to Spare”.Bloomberg. Retrieved 6 April 2014.
- Aljada A, Garg R, Ghanim H, et al. (2001). “Nuclear factor-kappaB suppressive and inhibitor-kappaB stimulatory effects of troglitazone in obese patients with type 2 diabetes: evidence of an antiinflammatory action?”. J. Clin. Endocrinol. Metab. 86 (7): 3250–6.doi:10.1210/jc.86.7.3250. PMID 11443197.
External links
- Diabetes Monitor article on troglit
| US4316849 * | 11 Jul 1980 | 23 Feb 1982 | Blasinachim S.P.A. | Process for preparing a crystalline polymorphous type of chenodeoxycholic acid |
| US4572912 * | 28 Aug 1984 | 25 Feb 1986 | Sankyo Company Limited | Treatment of hyperlipemia and hyperglycemia |
| US5248699 * | 13 Aug 1992 | 28 Sep 1993 | Pfizer Inc. | Hydrochloride salt, antidepressant, anorectic |
| US5319097 * | 11 Dec 1991 | 7 Jun 1994 | Imperial Chemical Industries Plc | Pharmaceutical agents |
| AU3255984A * | Title not available | |||
| EP0014590A1 * | 7 Feb 1980 | 20 Aug 1980 | Eli Lilly And Company | Crystalline forms of N-2-(6-methoxy)benzothiazolyl-N’-phenyl urea and process for their preparation |
| EP0022527A1 * | 4 Jul 1980 | 21 Jan 1981 | BLASCHIM S.p.A. | Process for preparing a solvent-free crystalline polymorphous form of chenodeoxycholic acid |
| EP0490648A1 * | 11 Dec 1991 | 17 Jun 1992 | Zeneca Limited | Pharmaceutical agents |
TAK-733……. clinical studies for cancer treatment.

TAK-733
CAS: 1035555-63-5
Synonym: TAK-733; TAK 733; TAK733.
IUPAC/Chemical name:
(R)-3-(2,3-Dihydroxypropyl)-6-fluoro-5-(2-fluoro-4-iodophenylamino)-8-methylpyrido[2,3-d]pyrimidine-4,7(3H,8H)-dione
Chemical Formula: C17H15F2IN4O4
Exact Mass: 504.01060
Elemental Analysis: C, 40.49; H, 3.00; F, 7.54; I, 25.17; N, 11.11; O, 12.69
Phase I clinical studies for cancer treatment.Takeda Pharmaceutical,
Solid Tumors Therapy
Description of TAK-733: TAK-733 is an orally bioavailable small-molecule inhibitor of MEK1 and MEK2 (MEK1/2) with potential antineoplastic activity. MEK inhibitor TAK-733 selectively binds to and inhibits the activity of MEK1/2, preventing the activation of MEK1/2-dependent effector proteins and transcription factors, which may result in the inhibition of growth factor-mediated cell signaling and tumor cell proliferation. MEK1/2 (MAP2K1/K2) are dual-specificity threonine/tyrosine kinases that play key roles in the activation of the RAS/RAF/MEK/ERK pathway and are often upregulated in a variety of tumor cell types.
Current developer: Millennium Pharmaceuticals, Inc./Takeda Pharmaceutical Company Limited.
TAK-733 is being developed at Millennium Pharmaceuticals for the treatment of adult patients with advanced non-hematological malignancies. Phase I clinical trials are ongoing for the treatment of advanced metastatic melanoma. In preclinical studies, the compound has been shown to bind to and potently inhibit MEK.
………………………………….
Discovery of TAK-733, a potent and selective MEK allosteric site inhibitor for the treatment of cancer
- Takeda San Diego;10410 Science Center Drive, San Diego, CA 92121, United States
http://www.sciencedirect.com/science/article/pii/S0960894X11000941
Synthesis of compounds 26 and 27 (Route 4). Reagents and conditions: (a) 1-chloro-2,4-dinitrobenzene, K2CO3, DMF; (b) (R)-O-((2,2-dimethyl-1,3-dioxolan-4-yl)methyl)hydroxylamine or 2,2-dimethyl-1,3-dioxan-5-amine, K2CO3 or Cs2CO3, DMF; (c) HCl, THF; (d) Selectfluor, CH3CN,DMF.
TAK-733 exhibited potent enzymatic and cell activity with an IC50 of 3.2 nM against constitutively active MEK enzyme and an EC50 of 1.9 nM against ERK phosphorylation in cells. TAK-733 did not inhibit any other kinases, receptors or ion channels that were tested with inhibitor concentrations up to 10 μM. TAK-733 was found to bind plasma protein moderately (ca. 97% for human and 96% for mouse), and exhibit high permeability and high microsomal stability across species. It did not inhibit P450s up to 30 μM.
The co-crystal structure of TAK-733 in the MEK1 allosteric site has been solved (Fig. 3). As predicted, the pyridone oxygen makes a hydrogen bond with the backbone NH of Ser212. The 2-fluoro-4-iodoaniline moeity sits in the deep lipophilic pocket. The pyrimidinone oxygen makes a hydrogen bond with Lys97, and the propanediol terminal hydroxyl interacts with both Lys97 and the ADP phosphate.

(R)-3-(2,3-Dihydroxypropyl)-6-fluoro-5-(2-fluoro-4-iodophenylamino)-8-methylpyrido[2,3-d]pyrimidine-4,7(3H,8H)-dione
| Molecular Weight: | 504.23 |
| TAK-733 Formula: | C17H15F2IN4O4 |
| CAS Number: | 1035555-63-5 |
TAK-733 is an orally bioavailable small-molecule inhibitor of MEK1 and MEK2 (MEK1/2) with potential antineoplastic activity. MEK inhibitor TAK-733 selectively binds to and inhibits the activity of MEK1/2, preventing the activation of MEK1/2-dependent effector proteins and transcription factors, which may result in the inhibition of growth factor-mediated cell signaling and tumor cell proliferation. MEK1/2 (MAP2K1/K2) are dual-specificity threonine/tyrosine kinases that play key roles in the activation of the RAS/RAF/MEK/ERK pathway and are often upregulated in a variety of tumor cell types.

BRAF L597 mutations in melanoma are associated with sensitivity to MEK inhibitors.
Dahlman et al. Cancer Discov. 2012 Jul 13. PMID: 22798288.Discovery of TAK-733, a potent and selective MEK allosteric site inhibitor for the treatment of cancer.
Dong et al. Bioorg Med Chem Lett. 2011 Mar 1;21(5):1315-9. PMID: 21310613.
16: 1652-1659


The reaction of F with the nosylate G gave a mixture of N- and O-alkylation products (8:1) from which the desired N-alkylation product was isolated by crystallization. The mixture of N-methyl pyrrolidine (NMP) and methanol used in the final deprotection step, helped to ensure formation of the desired polymorph. The nine-step discovery synthesis (3% overall yield) is also presented.
|
Information about this agent |
TAK-733 is currently in Phase I clinical trials and is being developed by Millennium Pharmaceuticals, Inc. (a part of Takeda Pharmaceutical Company Limited).
|
References |
1: Acquaviva J, Smith DL, Jimenez JP, Zhang C, Sequeira M, He S, Sang J, Bates RC, Proia DA. Overcoming acquired BRAF inhibitor resistance in melanoma via targeted inhibition of Hsp90 with ganetespib. Mol Cancer Ther. 2014 Feb;13(2):353-63. doi: 10.1158/1535-7163.MCT-13-0481. Epub 2014 Jan 7. PubMed PMID: 24398428.
2: Zhang Y, Xue D, Wang X, Lu M, Gao B, Qiao X. Screening of kinase inhibitors targeting BRAF for regulating autophagy based on kinase pathways. Mol Med Rep. 2014 Jan;9(1):83-90. doi: 10.3892/mmr.2013.1781. Epub 2013 Nov 7. PubMed PMID: 24213221.
3: Nakamura A, Arita T, Tsuchiya S, Donelan J, Chouitar J, Carideo E, Galvin K, Okaniwa M, Ishikawa T, Yoshida S. Antitumor activity of the selective pan-RAF inhibitor TAK-632 in BRAF inhibitor-resistant melanoma. Cancer Res. 2013 Dec 1;73(23):7043-55. doi: 10.1158/0008-5472.CAN-13-1825. Epub 2013 Oct 11. PubMed PMID: 24121489.
4: Garraway LA, Baselga J. Whole-genome sequencing and cancer therapy: is too much ever enough? Cancer Discov. 2012 Sep;2(9):766-8. doi: 10.1158/2159-8290.CD-12-0359. PubMed PMID: 22969114.
5: Dahlman KB, Xia J, Hutchinson K, Ng C, Hucks D, Jia P, Atefi M, Su Z, Branch S, Lyle PL, Hicks DJ, Bozon V, Glaspy JA, Rosen N, Solit DB, Netterville JL, Vnencak-Jones CL, Sosman JA, Ribas A, Zhao Z, Pao W. BRAF(L597) mutations in melanoma are associated with sensitivity to MEK inhibitors. Cancer Discov. 2012 Sep;2(9):791-7. Epub 2012 Jul 13. PubMed PMID: 22798288; PubMed Central PMCID: PMC3449158.
6: von Euw E, Atefi M, Attar N, Chu C, Zachariah S, Burgess BL, Mok S, Ng C, Wong DJ, Chmielowski B, Lichter DI, Koya RC, McCannel TA, Izmailova E, Ribas A. Antitumor effects of the investigational selective MEK inhibitor TAK733 against cutaneous and uveal melanoma cell lines. Mol Cancer. 2012 Apr 19;11:22. PubMed PMID: 22515704; PubMed Central PMCID: PMC3444881.
7: Dong Q, Dougan DR, Gong X, Halkowycz P, Jin B, Kanouni T, O’Connell SM, Scorah N, Shi L, Wallace MB, Zhou F. Discovery of TAK-733, a potent and selective MEK allosteric site inhibitor for the treatment of cancer. Bioorg Med Chem Lett. 2011 Mar 1;21(5):1315-9. doi: 10.1016/j.bmcl.2011.01.071. Epub 2011 Jan 22. PubMed PMID: 21310613.
| US8030317 | Dec 18, 2007 | Oct 4, 2011 | Takeda Pharmaceutical Company Limited | MAPK/ERK kinase inhibitors |
| US20080255160 | Dec 18, 2007 | Oct 16, 2008 | Qing Dong | Mapk/erk kinase inhibitors |
| WO2008000020A1 | Jun 27, 2007 | Jan 3, 2008 | Gary L Corino | Improved process |
| EP1894932A1 | Jun 10, 2005 | Mar 5, 2008 | Japan Tobacco, Inc. | 5-amino-2,4,7-trioxo-3,4,7,8-tetrahydro-2H-pyrido[2,3-d]pyrimidine derivatives and related compounds for the treatment of cancer |
| US20050222177 * | Jul 29, 2004 | Oct 6, 2005 | Irm Llc | Diseases with abnormal activation of the Abl, BCR-Abl, Bmx, CSK, TrkB, FGFR3, Fes, Lck, B-RAF, C-RAF, MKK6, alpha and beta SAPK2 kinases; antiproliferative; pyrrolo[2,3-d]pyrimidine-7-carboxylic acid [3-phenylcarbamoyl-phenyl]-amides and pyrrolo[3,2-c]pyridine analogs |
Aplaviroc, AK602, GSK-873140

Aplaviroc
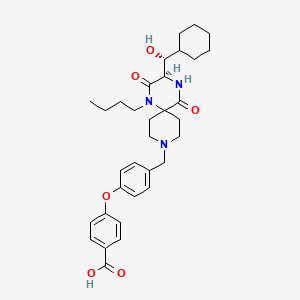
4-(4-{[(3R)-1-butyl-3-[(R)-cyclohexylhydroxymethyl]-2,5-dioxo- 1,4,9-triazaspiro[5.5]undecan-9-yl]methyl}phenoxy)benzoic acid
for the treatment of HIV infection
461023-63-2 of hydrochloride
461443-59-4 (free base)
873140
AK-602
GW-873140
ONO-4128
ono…….innovator
| Ono Pharmaceutical Co., Ltd. |
| Identifiers | |
|---|---|
| CAS number | 461023-63-2 |
| ATC code | None |
| PubChem | CID 3001322 |
| ChemSpider | 2272720 |
| UNII | 98B425P30V |
| KEGG | D06557 |
| ChEMBL | CHEMBL1255794 |
| Chemical data | |
| Formula | C33H43N3O6 |
| Mol. mass | 577.711 g/mol |
Aplaviroc (INN, codenamed AK602 and GSK-873140) is a CCR5 entry inhibitor developed for the treatment of HIV infection.[1][2] It is developed by GlaxoSmithKline.
In October 2005, all studies of aplaviroc were discontinued due to liver toxicity concerns.[3][4] Some authors have claimed that evidence of poor efficacy may have contributed to termination of the drug’s development;[5] the ASCENT study, one of the discontinued trials, showed aplaviroc to be under-effective in many patients even at high concentrations.[6]
Aplaviroc hydrochloride, an orally-effective, long-acting chemokine CCR5 receptor antagonist, had been under development by Ono and GlaxoSmithKline for the treatment of HIV infection. In early 2006, the companies discontinued development of the antagonist based on reports of elevated liver function test values from clinical studies.
Originally developed at Ono, aplaviroc was licensed to GlaxoSmithKline in 2003 for development, manufacturing and marketing. GlaxoSmithKline also obtained rights to evaluate the agent in non-HIV conditions worldwide with the exception of Japan, South Korea and Taiwan.
A low-molecular-weight compound, aplaviroc prevents HIV viral infection by blocking the binding of the virus to the CCR5 receptor
……………….
WO 2002074770
0r
http://www.google.com/patents/EP1378510A1?cl=en
Reference example 3(3)
- (3R)-1-butyl-2,5-dioxo-3-((1R)-1-hydroxy-1-cyclohexyl)-1,4,9-triazaspiro[5.5]undecane • hydrochloride
-
[0136]
TLC:Rf 0.32 (butanol:acetic acid:water = 4:2:1);
NMR (CD3OD): δ 4.16 (d, J = 2.0 Hz, 1H), 3.95 (m, 1H), 3.70 (m, 1H), 3.52 (m, 1H), 3.37 (m, 1H), 3.28 (m, 1H), 3.22-3.13 (m, 2H), 2.46-1.93 (m, 6H), 1.80-1.64 (m, 5H), 1.48-1.15 (m, 6H), 1.02-0.87 (m, 5H);
Optical rotation:[α]D +1.22 (c 1.04, methanol, 26°C).
Example 9(54)
- (3R)-1-butyl-2,5-dioxo-3-((1R)-1-hydroxy-1-cyclohexylmethyl)-9-(4-(4-carboxyphenyloxy)phenylmethyl)-1,4,9-triazaspiro[5.5]undecane • hydrochloride
-
[0359]
TLC:Rf 0.43(chloroform:methanol = 5:1);
NMR (CD3OD):δ 8.05 (d, J = 9.0 Hz, 2H), 7.61 (d, J = 9.0 Hz, 2H), 7.19 (d, J = 9.0 Hz, 2H), 7.08 (d, J = 9.0 Hz, 2H), 4.38 (s, 2H), 4.17 (d, J = 2.1 Hz, 1H), 4.02 (m, 1H), 3.78 (m, 1H), 3.60-3.40 (m, 3H), 3.30-3.10 (m, 2H), 2.56-1.86 (m, 6H), 1.82-1.60 (m, 5H), 1.52-1.16 (m, 6H), 1.06-0.82 (m, 2H), 0.97 (t, J = 7.2 Hz, 3H).
………………….
http://www.beilstein-journals.org/bjoc/single/articleFullText.htm?publicId=1860-5397-9-265
Owing to the special properties of piperazines (increased solubility and H-bond acceptor capability etc.) it is often considered to be a privileged structure and therefore occurs widely, for instance in GlaxoSmithKlines investigational anti-HIV drug aplaviroc (4.37) which, despite being a promising CCR5 receptor antagonist, was discontinued due to hepatotoxicity concerns. In this compound the spirodiketopiperazine unit (4.35) was designed to mimic a type-1 β-turn (4.36) as present in G-protein coupled receptors (Figure 14) [117].
The synthesis of aplaviroc and its analogues can be accomplished via the use of an Ugi multicomponent reaction (Ugi-MCR) [118]. The procedure involved the condensation of piperidone 4.38 and butylamine (4.39) followed by reaction of the resulting imine with isocyanide 4.41 and interception of the nitrilium intermediate with the amino acid4.40 (Scheme 47) [119]. This sequence was completed by structural rearrangement and acid-mediated ring closure to produce the spirocyclic diketopiperazine 4.43. Following debenzylation this material was subjected to a reductive amination finally affording aplaviroc analogues (Scheme 47).
- 117 Habashita, H.; Kokubo, M.; Hamano, S.; Hamanaka, N.; Toda, M.; Shibayama, S.; Tada, H.; Sagawa, K.; Fukushima, D.; Maeda, K.; Mitsuya, H. J. Med. Chem. 2006, 49, 4140–4152. doi:10.1021/jm060051s
- Dömling, A.; Huang, Y. Synthesis 2008, 2859–2883. doi:10.1055/s-0030-1257906
ref 118 - Nishizawa, R.; Nishiyama, T.; Hisaichi, K.; Matsunaga, N.; Minamoto, C.; Habashita, H.; Takaoka, Y.; Toda, M.; Shibayama, S.; Tada, H.; Sagawa, K.; Fukushima, D.; Maeda, K.; Mitsuya, H.Bioorg. Med. Chem. Lett. 2007, 17, 727–731. doi:10.1016/j.bmcl.2006.10.084
ref 119
| Patent | Submitted | Granted |
|---|---|---|
| Triazaspiro[5.5]undecane derivative and pharmaceutical composition comprising the same as active ingredient [US7262193] | 2005-09-29 | 2007-08-28 |
| Drugs containing triazaspiro[5.5]undecane derivatives as the active ingredient [US7285552] | 2004-06-03 | 2007-10-23 |
| Triazaspiro[5.5]undecane derivatives and drugs containing the same as the active ingredient [US7053090] | 2004-04-29 | 2006-05-30 |
| WO1998031364A1 * | Jan 20, 1998 | Jul 23, 1998 | Timothy Harrison | 3,3-disubstituted piperidines as modulators of chemokine receptor activity |
| WO2000014086A1 * | Jan 21, 1999 | Mar 16, 2000 | Kyowa Hakko Kogyo Kk | Chemokine receptor antagonists and methods of use therefor |
| WO2002074769A1 * | Mar 18, 2002 | Sep 26, 2002 | Kenji Maeda | Drugs containing triazaspiro[5.5]undecane derivatives as the active ingredient |
References
- Maeda, Kenji; Ogata, Hiromi; Harada, Shigeyoshi et al. (2004). “Determination of binding sites of a unique CCR5 inhibitor AK602 / ONO-4128/ GW873140 on human CCR5” (PDF). Conference on Retroviruses and Opportunistic Infections. Archived from the original on November 3, 2005.
- Nakata, Hirotomo; Maeda, Kenji; Miyakawa, Toshikazu et al. (February 2005). “Potent Anti-R5 Human Immunodeficiency Virus Type 1 Effects of a CCR5 Antagonist, AK602/ONO4128/GW873140, in a Novel Human Peripheral Blood Mononuclear Cell Nonobese Diabetic-SCID, Interleukin-2 Receptor γ-Chain-Knocked-Out AIDS Mouse Model”. Journal of Virology 79 (4): 2087–96.doi:10.1128/jvi.79.4.2087-2096.2005.
- “Aplaviroc (GSK-873,140)”. AIDSmeds.com. October 25, 2005. Retrieved September 5, 2008.[dead link]
- Nichols WG, Steel HM, Bonny T et al. (March 2008). “Hepatotoxicity Observed in Clinical Trials of Aplaviroc (GW873140)”.Antimicrobial Agents and Chemotherapy 52 (3): 858–65. doi:10.1128/aac.00821-07. PMC 2258506. PMID 18070967.
- Moyle, Graeme (December 19, 2006). “The Last Word on Aplaviroc: A CCR5 Antagonist With Poor Efficacy”. The Body.Archived from the original on 6 October 2008. Retrieved September 5, 2008.
- Currier, Judith; Lazzarin, Adriano; Sloan, Louis et al. (2008). “Antiviral activity and safety of aplaviroc with lamivudine/zidovudine in HIV-infected, therapy-naive patients: the ASCENT (CCR102881) study”. Antiviral Therapy (Lond.) 13 (2): 297–306.PMID 18505181.
Further reading
- Horster, S; Goebel, FD (April 2006). “Serious doubts on safety and efficacy of CCR5 antagonists: CCR5 antagonists teeter on a knife-edge”. Infection 34 (2): 110–13. doi:10.1007/s15010-006-6206-1. PMID 16703305.
Beta carotene may protect people with common genetic risk factor for type-2 diabetes
25 JAN 2013
STANFORD, Calif. — Stanford University School of Medicine investigators have found that for people harboring a genetic predisposition that is prevalent among Americans, beta carotene, which the body converts to a close cousin of vitamin A, may lower the risk for the most common form of diabetes, while gamma tocopherol, the major form of vitamin E in the American diet, may increase risk for the disease.
The scientists used a “big data” approach to hunt down interactions between gene variants previously associated with increased risk for type-2 diabetes and blood levels of substances previously implicated in type-2 diabetes risk. In people carrying a double dose of one such predisposing gene variant, the researchers pinpointed a highly statistically significant inverse association of beta carotene blood levels with type-2 diabetes risk, along with a suspiciously high positive association of gamma tocopherol with risk for the disease.
“Type-2 diabetes affects…
View original post 1,081 more words
New USP Requirements on Plastic Packaging Systems
DRUG REGULATORY AFFAIRS INTERNATIONAL

New USP Requirements on Plastic Packaging Systems |
| The USP describes in an article of the Pharmacopeial Forum the future requirements for plastic packaging systems. Here, the importance is laid on the selection of suitable, safe plastic materials and the verification of potential interactions. More information can be found here in the News. |
GMP News: New USP Requirements on Plastic Packaging Systems
An interesting article from the USP on the future requirements for plastic packaging systems has been published in the Pharmacopoeial Forum 39(6).
In this article, the USP’s experts group provides an overview of the already existing and also the planned General Chapters on pharmaceutical plastic packaging systems. Together both chapters aim to describe a general and chemistry-based approach for the quality and safety of packaging systems and their starting materials for the construction of these packaging systems.
Among the key topics which are discussed, you can find:
- a. The…
View original post 160 more words
SURAMIN

Suramin
A polyanionic compound with an unknown mechanism of action. It is used parenterally in the treatment of African trypanosomiasis and it has been used clinically with diethylcarbamazine to kill the adult Onchocerca. (From AMA Drug Evaluations Annual, 1992, p1643) It has also been shown to have potent antineoplastic properties.
A polyanionic compound with an unknown mechanism of action. It is used parenterally in the treatment of African trypanosomiasis and it has been used clinically with diethylcarbamazine to kill the adult Onchocerca. (From AMA Drug Evaluations Annual, 1992, p1643) It has also been shown to have potent antineoplastic properties. Suramin is manufactured by Bayer in Germany as Germanin®.
Also known as: Naphuride, Germanin, Naganol, Belganyl, Fourneau, Farma, Antrypol, Suramine, Naganin
8,8′-{Carbonylbis[imino-3,1-phenylenecarbonylimino(4-methyl-3,1-phenylene)carbonylimino]}di(1,3,5-naphthalenetrisulfonic acid) …FREE FORM
8,8′-[Ureylenebis[m-phenylenecarbonylimino(4-methyl-m-phenylene)carbonylimino]]di(1,3,5-naphthalenetrisulfonic acid) hexasodium salt
CAS 145-63-1 FREE FORM
129-46-4 of hexa sodium
LAUNCHED 1940 BAYER
| Formula | C51H40N6O23S6 |
|---|---|
| Mol. mass | 1297.29 |
The molecular formula of suramin is C51H34N6O23S6. It is a symmetric molecule in the center of which lies urea, NH-CO-NH. Suramin contains eightbenzene rings, four of which are fused in pairs (naphthalene), four amide groups in addition to the one of urea and six sulfonate groups. When given as drug it usually contains six sodium ions that form a salt with the six sulfonate groups.
Suramin is a drug developed by Oskar Dressel and Richard Kothe of Bayer, Germany in 1916, and is still sold by Bayer under the brand nameGermanin.
Suramin sodium is a heparanase inhibitor that was first launched in 1940 by Bayer under the brand name Antrypol for the treatment of helminthic infection. It was later launched by Bayer for the treatment of trypanosomiasis (African sleeping sickness).
More recently, the product has entered early clinical development at Ohio State University for the treatment of platinum-pretreated patients with stage IIIB/IV non-small cell lung cancer, in combination with docetaxel or gemcitabine.
The National Cancer Institute (NCI) is conducting phase II clinical studies for the treatment of glioblastoma multiforme and for the treatment of adrenocortical carcinoma.
According to the National Cancer Institute there are no active clinical trials (as of April 1, 2008). Completed and closed clinical trials are listed here:[1]
In addition to Germanin, the National Cancer Institute also lists the following “Foreign brand names”: 309 F or 309 Fourneau,[1] Bayer 205, Moranyl, Naganin, Naganine.

It is used for treatment of human sleeping sickness caused by trypanosomes.[2]
It has been used in the treatment of onchocerciasis.[3]
It has been investigated as treatment for prostate cancer.[4]
Also, suramin as treatment for autism is being evaluated. [5]
Suramin is administered by a single weekly intravenous injection for six weeks. The dose per injection is 1 g.
The most frequent adverse reactions are nausea and vomiting. About 90% of patients will get an urticarial rash that disappears in a few days without needing to stop treatment. There is a greater than 50% chance of adrenal cortical damage, but only a smaller proportion will require lifelongcorticosteroid replacement. It is common for patients to get a tingling or crawling sensation of the skin with suramin. Suramin will cause clouding of the urine which is harmless: patients should be warned of this to avoid them becoming alarmed.
Kidney damage and exfoliative dermatitis occur less commonly.
Suramin has been applied clinically to HIV/AIDS patients resulting in a significant number of fatal occurrences and as a result the application of this molecule was abandoned for this condition. http://www.ncbi.nlm.nih.gov/pubmed/3548350
Suramin is also used in research as a broad-spectrum antagonist of P2 receptors[6][7] and agonist of Ryanodine receptors.[8]
![ChemSpider 2D Image | 8,8'-{Carbonylbis[imino-3,1-phenylenecarbonylimino(4-methyl-3,1-phenylene)carbonylimino]}di(1,3,5-naphthalenetrisulfonic acid) | C51H40N6O23S6](https://images-blogger-opensocial.googleusercontent.com/gadgets/proxy?url=http%3A%2F%2Fwww.chemspider.com%2FImagesHandler.ashx%3Fid%3D5168%26w%3D200%26h%3D200&container=blogger&gadget=a&rewriteMime=image%2F*)
Its effect on telomerase has been investigated.[9]
It may have some activity against RNA viruses.[10]
In addition to antagonism of P2 receptors, Suramin inhibits the acitivation of heterotrimeric G proteins in a variety of other GPCRs with varying potency. It prevents the association of heteromeric G proteins and therefore the receptors Guanine exchange functionality (GEF). With this blockade the GDP will not release from the Gα subunit so it can not be replaced by a GTP and become activated. This has the effect of blocking downstream G protein mediated signaling of various GPCR proteins including Rhodopsin, the A1 Adenosine receptor, and the D2 dopamine receptor.[11]
A polyanionic compound with an unknown mechanism of action. It is used parenterally in the treatment of African trypanosomiasis and it has been used clinically with diethylcarbamazine to kill the adult Onchocerca. (From AMA Drug Evaluations Annual, 1992, p1643) It has also been shown to have potent antineoplastic properties. Suramin is manufactured by Bayer in Germany as Germanin®.
|
8-1-2012 |
InCl3-catalysed synthesis of 2-aryl quinazolin-4(3H)-ones and 5-aryl pyrazolo[4,3-d]pyrimidin-7(6H)-ones and their evaluation as potential anticancer agents. |
Bioorganic & medicinal chemistry letters |
|
9-1-2012 |
Identification of a sirtuin 3 inhibitor that displays selectivity over sirtuin 1 and 2. |
European journal of medicinal chemistry |
|
1-1-2013 |
Inhibition of the human deacylase Sirtuin 5 by the indole GW5074. |
Bioorganic & medicinal chemistry letters |
|
5-9-2013 |
Discovery of thieno[3,2-d]pyrimidine-6-carboxamides as potent inhibitors of SIRT1, SIRT2, and SIRT3. |
Journal of medicinal chemistry |
- The formula of suramin was kept secret by Bayer for commercial reasons. But it was elucidated and published in 1924 by Fourneau and his team of the Pasteur Institute, and it is only on this date that its exact chemical composition was known. (E. Fourneau, J. and Th. Tréfouël and J. Vallée (1924). “Sur une nouvelle série de médicaments trypanocides”, C. R. Séances Acad. Sci. 178: 675.)
- Darsaud A, Chevrier C, Bourdon L, Dumas M, Buguet A, Bouteille B (January 2004). “Megazol combined with suramin improves a new diagnosis index of the early meningo-encephalitic phase of experimental African trypanosomiasis”. Trop. Med. Int. Health 9 (1): 83–91.doi:10.1046/j.1365-3156.2003.01154.x. PMID 14728611.
- Anderson J, Fuglsang H (July 1978). “Further studies on the treatment of ocular onchocerciasis with diethylcarbamazine and suramin”. Br J Ophthalmol 62 (7): 450–7.doi:10.1136/bjo.62.7.450. PMC 1043255. PMID 678497.
- Ahles TA, Herndon JE, Small EJ, et al. (November 2004). “Quality of life impact of three different doses of suramin in patients with metastatic hormone-refractory prostate carcinoma: results of Intergroup O159/Cancer and Leukemia Group B 9480”. Cancer 101 (10): 2202–8.doi:10.1002/cncr.20655. PMID 15484217.
- http://medicalxpress.com/news/2013-03-drug-treatment-autism-symptoms-mouse.html
- Abbracchio MP, Burnstock G, Boeynaems JM, Barnard EA, Boyer JL, Kennedy C, Knight GE, Fumagalli M, Gachet C, Jacobson KA, Weisman GA. (september 2006). “International Union of Pharmacology LVIII: update on the P2Y G protein-coupled nucleotide receptors: from molecular mechanisms and pathophysiology to therapy”. Pharmacol Rev. 58 (3): 281–341.doi:10.1124/pr.58.3.3. PMID 16968944.
- Khakh BS, Burnstock G, Kennedy C, King BF, North RA, Séguéla P, Voigt M, Humphrey PP. (march 2001). “International union of pharmacology. XXIV. Current status of the nomenclature and properties of P2X receptors and their subunits”. Pharmacol Rev. 53 (1): 107–118.PMID 11171941.
- Wolner I, Kassack MU, Ullmann H, Karel A, Hohenegger M (October 2005). “Use-dependent inhibition of the skeletal muscle ryanodine receptor by the suramin analogue NF676”. Br. J. Pharmacol. 146 (4): 525–33. doi:10.1038/sj.bjp.0706359. PMC 1751178.PMID 16056233.
- Erguven M, Akev N, Ozdemir A, Karabulut E, Bilir A (August 2008). “The inhibitory effect of suramin on telomerase activity and spheroid growth of C6 glioma cells”. Med. Sci. Monit. 14(8): BR165–73. PMID 18667993.
- Mastrangelo E, Pezzullo M, Tarantino D, Petazzi R, Germani F, Kramer D, Robel I, Rohayem J, Bolognesi M, Milani M (2012) Structure-based inhibition of norovirus RNA-dependent RNA-polymerases. J Mol Biol
- Beindl W, Mitterauer T, Hohenegger M, Ijzerman AP, Nanoff C, Freissmuth M. (August 1996).“Inhibition of receptor/G protein coupling by suramin analogues”. ol. Pharmacology. 50 (2): 415–23. PMID 8700151.
- Drugs Fut 1986, 11(10): 860
- WO 2012159107
- WO 2012087336
- US 2011257109
- WO 2009022897
- WO 2009020613
- WO 2008094027
- EP 0486809
- US 5158940
- US 5173509
- WO 1993007864
- WO 1994008574
SURAMIN
- Suramin bound to proteins in the PDB
- Drug information
- Suramin, drug information by JBC Online
- Suramin in treating patients with recurrent bladder cancer
- National Cancer Institute
Enterovirus-71 (EV71) is one of the major causative reagents for hand-foot-and-mouth disease. In particular, EV71 causes severe central nervous system infections and leads to numerous dead cases. Although several inactivated whole-virus vaccines have entered in clinical trials, no antiviral agent has been provided for clinical therapy. In the present work, we screened our compound library and identified that suramin, which has been clinically used to treat variable diseases, could inhibit EV71 proliferation with an IC50 value of 40μM. We further revealed that suramin could block the attachment of EV71 to host cells to regulate the early stage of EV71 infection, as well as affected other steps of EV71 life cycle. Our results are helpful to understand the mechanism for EV71 life cycle and provide a potential for the usage of an approved drug, suramin, as the antiviral against EV71 infection.
- Suramin Hexasodium
- 129-46-4
Synonyms
- 309 F
- Antrypol
- BAY 205
- Bayer 205
- CI-1003
- EINECS 204-949-3
- Fourneau 309
- Germanin
- Moranyl
- Naganin
- Naganine
- Naganinum
- Naganol
- Naphuride sodium
- NF060
- NSC 34936
- SK 24728
- Sodium suramin
- Suramin Hexasodium
- Suramin sodium
- Suramina sodica
- Suramina sodica [INN-Spanish]
- Suramine sodique
- Suramine sodique [INN-French]
- Suramine sodium
- Suraminum natricum
- Suraminum natricum [INN-Latin]
- UNII-89521262IH
Suramin Sodium, is an anticancer agent with a wide variety of activities.
Recently suramin was shown to inhibit FSH binding to its receptor (Daugherty, R. L.; Cockett, A. T. K.; Schoen, S. R. and Sluss, P. M. “Suramin inhibits gonadotropon action in rat testis: implications for treatment of advanced prostate cancer” J. Urol. 1992, 147, 727-732).
This activity causes, at least in part, the decrease in testosterone production seen in rats and humans that were administered suramin(Danesi, R.; La Rocca, R. V.; Cooper, M. R.; Ricciardi, M. P.; Pellegrini, A.; Soldani, P.; Kragel, P. J.; Paparelli, A.; Del Tacca, M.; Myers, C. E, “Clinical and experimental evidence of inhibition of testosterone production by suramin.” J. Clin. Endocrinol. Metab. 1996, 81, 2238-2246).
Suramin is the only non-peptidic small molecule that has been reported to be an FSH receptor binding antagonist.
Suramin is 8,8′ – (carbonylbis(imino-3,1-phenylenecarbonylimino (4-methyl-3,1-phenylene) carbonylimino)) bis-1,3 ,5-naphthalenetrisulfonic acid (GB Patent No. 224849). This polyanionic compound has been used for many decades as a prophylactic and therapeutic agent for try- panosomiasis. It was subsequently shown that suramin is able to block the activity of a variety of proteins like cellular and viral enzymes and growth factors (Mitsuya, M. et al. Science 226 : 172 (1984), Hosang, M. J. Cell. Biochem. 29 : 265 (1985), De Clercq, E. Cancer Lett. 8 : 9 (1979)).
![]()
|
5-32-1977 |
Complement inhibitors |
|
|
5-25-1977 |
Aromatic amidines as antiviral agents in animals |
|
|
5-4-1977 |
Complement inhibitors |
|
|
5-4-1977 |
Complement inhibitors |
|
|
4-27-1977 |
Cyclodextrin sulfate salts as complement inhibitors |
|
|
4-20-1977 |
Ureylenebis methyl-phenylene-carbonyl-bis-dihydro-2-oxo-naphthoxazine disultonic acids |
|
|
3-30-1977 |
Water treatment for controlling the growth of algae employing biguanides |
|
|
3-2-1977 |
Isoxazole substituted nitroimidazoles |
|
|
2-16-1977 |
Amidophenyl-azo-naphthalenesulfonic complement inhibitors and method of use thereof |
|
|
2-9-1977 |
Complement inhibitors |
|
2-10-2011 |
MODULATION OF HUMAN MAST CELL ACTIVATION MODULATION OF HUMAN MAST CELL ACTIVATION |
|
|
11-18-2010 |
Admixtures for inorganic binders based on a hydrogenated disaccharide, inorganic binders containing these admixtures and process for their preparation Admixtures for inorganic binders based on a hydrogenated disaccharide, inorganic binders containing these admixtures and process for their preparation |
|
|
10-28-2010 |
THERAPEUTIC INHIBITORS OF VASCULAR SMOOTH MUSCLE CELLS |
|
|
9-9-2010 |
APPARATUS FOR USING ELECTROPORATION MEDIATED DELIVERY OF DRUGS AND GENES |
|
|
4-8-2010 |
PREPARATION AND USE OF SULFATED OLIGOSACCHARIDES |
|
|
10-29-2009 |
THERAPEUTIC INHIBITOR OF VASCULAR SMOOTH MUSCLE CELLS THERAPEUTIC INHIBITOR OF VASCULAR SMOOTH MUSCLE CELLS |
|
|
8-20-2009 |
METHOD OF MAKING MINERAL FIBRES METHOD OF MAKING MINERAL FIBRES |
|
|
6-25-2009 |
OXYGEN-FUEL BOOST REFORMER PROCESS AND APPARATUS |
|
|
4-23-2009 |
METHODS OF TREATING VASCULAR DISEASE WITH TNF ANTAGONISTS METHODS OF TREATING VASCULAR DISEASE WITH TNF ANTAGONISTS |
|
|
3-26-2009 |
COPOLYMER COMPOSITIONS FOR ORAL DELIVERY |
|
5-3-1978 |
1,3,5- Or 1,3,6-naphthalenetriyltris(sulfonylimino)aryl acids and salts |
|
|
3-22-1978 |
Nitroimidazoles |
|
|
2-15-1978 |
Treatment of rheumatoid arthritis and related diseases |
|
|
1-4-1978 |
AROMATIC AMIDINES AS ANTIVIRAL AGENTS IN ANIMALS |
|
|
1-4-1978 |
Malto-dextrin poly(H-)sulfates |
|
|
12-14-1977 |
Disazo compounds useful as complement inhibitors |
|
|
12-7-1977 |
Bis-substituted naphthalene-azo phenyleneazo-stilbene-disulfonic and naphthalene-sulfonic acid |
|
|
9-28-1977 |
UREIDOPHENYLENEBIS(CARBONYLIMINO)DINAPHTHALENETRISULFONIC ACID COMPOUNDS |
|
|
9-21-1977 |
Substituted bisnaphthylazo diphenyl ureido complement inhibitors |
|
|
9-7-1977 |
Substituted-hydroxy-naphthalenedisulfonic acid compounds |
|
1-12-1977 |
Complement inhibitors |
|
|
12-22-1976 |
Complement inhibitors |
|
|
10-13-1976 |
Complement inhibitors |
![]()
| EP0183352A2 * | Sep 27, 1985 | Jun 4, 1986 | THE UNITED STATES OF AMERICA as represented by the Secretary United States Department of Commerce | Use of suramin for clinical treatment of infection with any of the members of the family of human-t-cell leukemia (htvl) viruses including lymphadenopathy virus (lav) |
| EP0205077A2 * | Jun 3, 1986 | Dec 17, 1986 | Bayer Ag | Suramin sodium for use as an immunostimulant |
![]()
| EP0515523A1 * | Feb 13, 1991 | Dec 2, 1992 | THE UNITED STATES OF AMERICA as represented by the Secretary United States Department of Commerce | Use of suramin to treat rheumatologic diseases |
| EP0755254A1 * | Mar 24, 1995 | Jan 29, 1997 | The Trustees Of The University Of Pennsylvania | Prevention and treatment of ischemia-reperfusion and endotoxin-related injury using adenosine and purino receptor antagonists |
| EP1460087A1 * | Feb 17, 1997 | Sep 22, 2004 | The Kennedy Institute Of Rheumatology | Methods of treating vascular disease with TNF antagonists |
| EP1940376A2 * | Oct 3, 2006 | Jul 9, 2008 | Rottapharm S.P.A. | Use of neboglamine in the treatment of toxicodependency |
| EP1945204A2 * | Oct 27, 2006 | Jul 23, 2008 | Brane Discovery S.R.L. | V-atpase inhibitors for use in the treatment of septic shock |
| US5453444 * | Oct 6, 1994 | Sep 26, 1995 | Otsuka Pharmaceutical Co., Ltd. | Method to mitigate or eliminate weight loss |
| US5534539 * | Jun 12, 1995 | Jul 9, 1996 | Farmitalia Carlo Erba S.R.L. | Biologically active ureido derivatives useful as anit-metastic agenst |
| US5596105 * | Jan 13, 1995 | Jan 21, 1997 | Farmitalia Carlo Erba S.R.L. | Therapeutically active naphthalenesulfonic pyrrolecarboxamido derivatives |
| US7476693 | Mar 26, 2003 | Jan 13, 2009 | Eastern Virginia Medical School | Suramin and derivatives thereof as topical microbicide and contraceptive |
| US7608262 | Feb 16, 1996 | Oct 27, 2009 | The Kennedy Institute Of Rheumatology | Methods of preventing or treating thrombosis with tumor necrosis factor antagonists |
| US8552064 | Dec 19, 2008 | Oct 8, 2013 | Eastern Virginia Medical School | Suramin and derivatives thereof as topical microbicide and contraceptive |
| WO1994008574A1 * | Oct 12, 1993 | Apr 28, 1994 | Otsuka America Pharmaceutical | Treatment of cachexia and inhibition of il-6 activity |
| WO1994010990A1 * | Nov 12, 1993 | May 26, 1994 | British Bio Technology | Inhibition of tnf production |
| WO1997030088A2 * | Feb 17, 1997 | Aug 21, 1997 | Kennedy Inst Of Rheumatology | Methods of treating vascular disease with tnf antagonists |
| WO2004113920A1 * | Jun 18, 2004 | Dec 29, 2004 | Babon Jeff James | Screening method for substances binding to merozoite surface protein-1/42 |
| WO2008138943A2 * | May 14, 2008 | Nov 20, 2008 | Mara Galli | Prophylactic and therapeutic use of sirtuin inhibitors in tnf-alpha mediated pathologies |
| WO2009137471A2 * | May 5, 2009 | Nov 12, 2009 | University Of Miami | Azo dye related small molecule modulators of protein-protein interactions |
| WO2010016628A1 * | Jul 10, 2009 | Feb 11, 2010 | Sammy Opiyo | Conjugated suramin amino compounds for medical conditions |
| WO2012159107A1 * | May 21, 2012 | Nov 22, 2012 | Rhode Island Hospital | Inhibition of renal fibrosis |
Title: Suramin Sodium
CAS Registry Number: 129-46-4
CAS Name: 8,8¢-[Carbonylbis[imino-3,1-phenylenecarbonylimino(4-methyl-3,1-phenylene)carbonylimino]]bis-1,3,5-naphthalenetrisulfonic acid hexasodium salt
Additional Names: hexasodium sym-bis(m-aminobenzoyl-m-amino-p-methylbenzoyl-1-naphthylamino-4,6,8-trisulfonate) carbamide
Manufacturers’ Codes: Bayer 205; Fourneau 309
Trademarks: Antrypol (AstraZeneca); Germanin (Bayer); Moranyl (Specia); Naganol; Naphuride
Molecular Formula: C51H34N6Na6O23S6
Molecular Weight: 1429.17
Percent Composition: C 42.86%, H 2.40%, N 5.88%, Na 9.65%, O 25.75%, S 13.46%
Literature References: Discovered in 1917 by O. Dressel and R. Kothe: J. Dressel, J. Chem. Educ. 38, 620 (1961). Prepn: E. Fourneau et al., Compt. Rend. 178, 675 (1924); J. Trefouel, E. Fourneau, GB 224849 (1923); B. Heymann, Angew. Chem. 37, 585 (1924). Pharmacology, toxicology and clinical antiparasitic activity: F. Hawking, Adv. Pharmacol. Chemother. 15, 289-322 (1978). Inhibition of reverse transcriptase in vitro: E. De Clercq, Cancer Lett. 8, 9 (1979); vs HIV: H. Mitsuya et al., Science 226, 172 (1984). HPLC determn in plasma: R. W. Klecker, J. M. Collins, J. Liq. Chromatogr. 8, 1685 (1985). Pharmacokinetics: J. M. Collins et al., J. Clin. Pharmacol. 26, 22 (1986). Pharmacology and virustatic effect in AIDS: S. Broder et al., Lancet 2, 627 (1985); A. M. Levine et al., Ann. Intern. Med. 105, 32 (1986). Clinical trial in onchocerciasis: H. Schultz-Key et al., Trop. Med. Parasitol. 36, 244 (1985); in prostate cancer: C. Myers et al., J. Clin. Oncol. 10, 881 (1992). Review: Olenick in Antibiotics vol. 3,J. W. Corcoran, F. E. Hahn, Eds. (Springer-Verlag, New York, 1975) pp 699-703; R. La Rocca et al., Cancer Cells 2, 106-115 (1990).
Properties: White or slightly pink or cream-colored powder. Slightly bitter taste. Hygroscopic. Freely sol in water, in physiological saline; sparingly sol in 95% alcohol. Insol in benzene, ether, petr ether, chloroform. Aq solns are neutral to litmus. LD50 in mice (mg/kg): ~620 i.v. (Hawking).
Toxicity data: LD50 in mice (mg/kg): ~620 i.v. (Hawking)
Therap-Cat: Anthelmintic (Nematodes); antiprotozoal (Trypanosoma).
Therap-Cat-Vet: Antiprotozoal (Trypanosoma).
Keywords: Anthelmintic (Nematodes); Antiprotozoal (Trypanosoma); Reverse Transcriptase Inhibitor.

![]()

THANKS AND REGARD’S
DR ANTHONY MELVIN CRASTO Ph.D
GLENMARK SCIENTIST , NAVIMUMBAI, INDIA
did you feel happy, a head to toe paralysed man’s soul in action for you round the clock
need help, email or call me
MOBILE-+91 9323115463
web link
I was paralysed in dec2007, Posts dedicated to my family, my organisation Glenmark, Your readership keeps me going and brings smiles to my family
Summary of Metabolomics
Leaders in Pharmaceutical Business Intelligence Group, LLC, Doing Business As LPBI Group, Newton, MA
Summary of Metabolomics
Author and Curator: Larry H. Bernstein, MD, FCAP
This concludes the series on metabolomics, a rapidly developing science that is interconnected with a group termed – OMICS: proteomics, transcriptomics, genomics, and metabolomics. This chapter is most representative of the many important studies being done in the field, which ranges most widely because it has opened doors into nutrition and nutritional supplements, plant biochemistry, agricultural crops and breeding, animal breeding, worldwide malnutrition, diabetes, cancer, neurosciences, circulatory, respiratory, and musculosletal disorders, infectious diseases and immune system disorders. Obviously, it is not possible to cover the full range of activity, but metabolomics is most comprehensive in exploring the full range of metabolic changes that occur in health during the full age range from development to the geriatric years. It can be integrated well with gene expression, proteomics studies, and epidemiological investigations.
The subchapters are given here:
7.1 Extracellular evaluation of intracellular flux in yeast cells
View original post 1,051 more words
Flow Chemistry test facility in India
Flow Chemistry test facility in India
BOOK YOUR TRIAL
on Plantrix® Industrial system.
Contacts:

India
Vijay Kirpalani
vk@pi-inc.co
0091 9821 3420 22
More information
Stan Hoeijmakers
info@chemtrix.com
0031 (0)46 70 22 600
EVENTS
Chemtrix at CPhI India
2 – 4 December 2014
Mumbai, India
Booth H47, Hall 5
Pi Process Intensification
read at
http://hosted.verticalresponse.com/721499/f9f4fc970b/285875213/4942751fec/
|
Plantrix® Industrial Flow Chemistry Test Facility in India
|
||||||||

|
||||||||
|
|
|||||||
|
|
||||||||
Chemtrix Bv.
Urmonderbaan 22
Geleen, 6167RD
NL
Yoga back bends: feels yummy on the autonomic nervous system
Beyond Meds: Alternatives to Psychiatry
 I’m reposting this because I’ve been going through another backbend stage and I thought of this post from a while back. I like to help people see how easy yoga can be. You can start with something as simple as this and see where it takes you. Being a yogi is about listening to your body and learning from it and it really doesn’t matter if you can do really complicated poses or not. Start simple and see what happens.
I’m reposting this because I’ve been going through another backbend stage and I thought of this post from a while back. I like to help people see how easy yoga can be. You can start with something as simple as this and see where it takes you. Being a yogi is about listening to your body and learning from it and it really doesn’t matter if you can do really complicated poses or not. Start simple and see what happens.
I’ve been using yoga as a main source of rehabilitation and recovery since I was bedridden. I began doing yoga while still in bed. Now it continues to be a primary source of continued healing. Lately I’ve been doing backbends and while all the yoga I do feels like it profoundly helps my nervous system, these bends have really been making me think about my autonomic nervous system and how…
View original post 744 more words

 DRUG APPROVALS BY DR ANTHONY MELVIN CRASTO
.....
DRUG APPROVALS BY DR ANTHONY MELVIN CRASTO
.....



















![[1860-5397-9-265-14]](https://i0.wp.com/www.beilstein-journals.org/bjoc/content/figures/1860-5397-9-265-14.png)
![[1860-5397-9-265-i47]](https://i0.wp.com/www.beilstein-journals.org/bjoc/content/inline/1860-5397-9-265-i47.png)







